Top 5 Mistakes People Make After Knee Replacement Surgery (And How To Avoid Them)

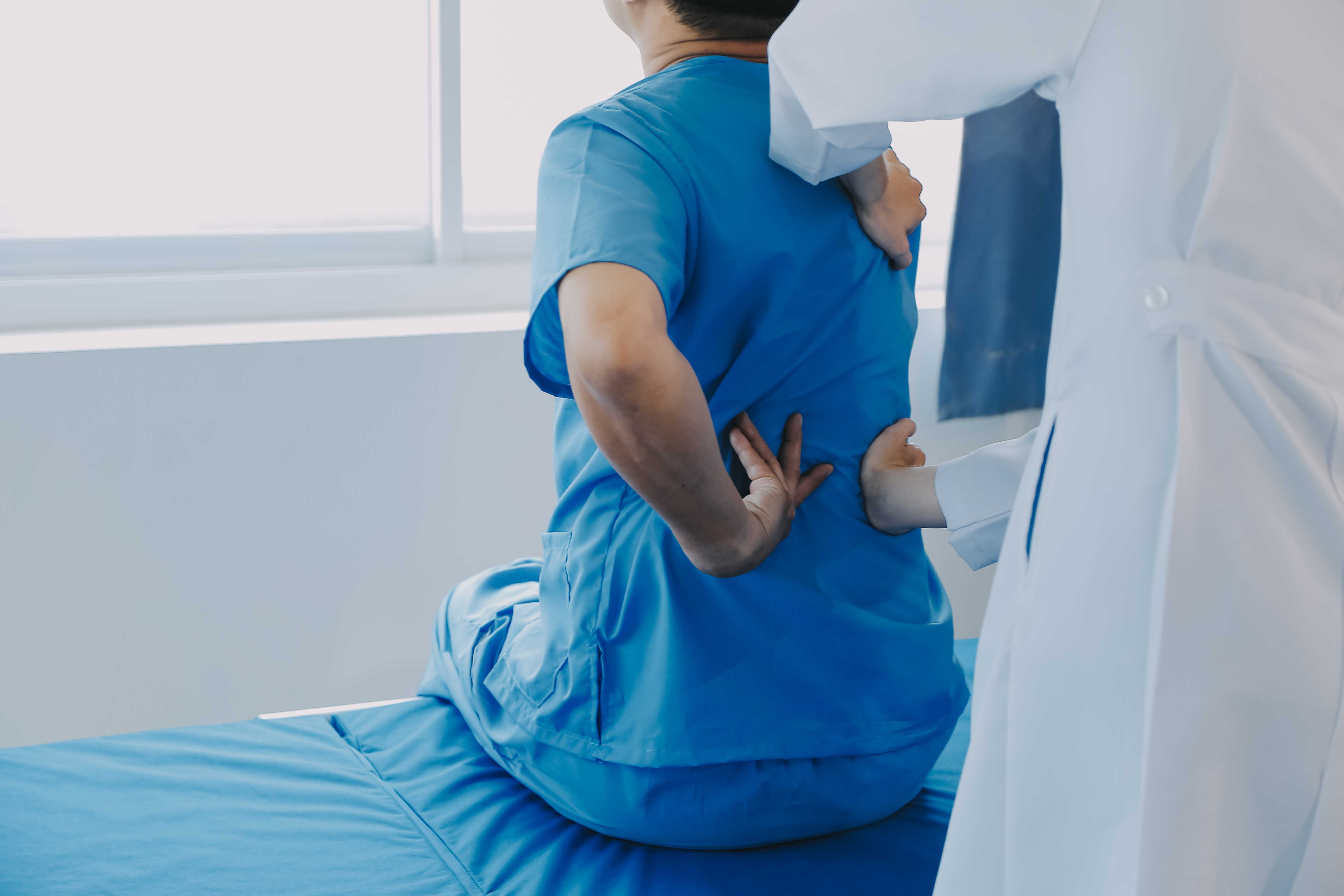
A healthcare professional examining a knee after surgery during recovery.
Knee replacement surgery is one of the most studied, most refined, and most successful procedures in modern orthopedics. When it goes right, and it usually does, the transformation is dramatic. Patients who couldn't walk to the kitchen without stopping in pain are climbing stairs, going on evening walks, and visiting temples within months.
But the surgery is only half the equation. What happens in the 3 to 6 months after the operation determines how complete, how lasting, and how satisfying that recovery is. And in that recovery period, patients make mistakes; some from impatience, some from ignorance, some from simply not being told what to watch out for.
These are the five mistakes that orthopedic surgeons in Noida and across India see most frequently. If you're preparing for knee replacement, or if you're currently recovering from one, this is worth reading carefully.
Mistake 1: Skipping Or Shortcutting Physiotherapy
This is the single most common and most damaging mistake patients make after knee replacement. And it comes in several forms:
- Not starting physiotherapy soon enough after discharge.
- Doing the exercises once or twice a day instead of as prescribed.
- Stopping physiotherapy when the pain reduces, typically around week 4 or 5, and assuming the job is done.
- Avoiding the harder exercises because they're uncomfortable.
Here's the reality: The surgery replaces the damaged joint surface. But the muscles, tendons, and stabilising structures around that new joint have been weakened by both the pre-existing arthritis and the operation itself. Physiotherapy is what rebuilds those structures. Without it, the joint functions below its potential, and patients end up with a new knee that works, but not as well as it could.
Specific consequences of inadequate physiotherapy:
- Flexion contracture - The knee gets stuck in a slightly bent position because scar tissue forms without the joint being regularly straightened and bent through its full range.
- Stiffness - The most feared long-term complication of inadequate rehab.
- Muscle weakness - Quads and hamstrings that remain weak put excessive stress on the implant.
- Slower return to independence - Everything takes longer.
What to do instead: Start physiotherapy within 24 hours of surgery, as guided by your physiotherapy team in hospital. After discharge, treat your home exercise programme the way you'd treat a prescribed medication, as it's not optional. Attend all outpatient physiotherapy sessions. Keep going with strengthening exercises even when pain is minimal, because that's when building muscle matters most.
The target range of motion milestones to work toward:
- 90 degrees by end of week 2
- 100–110 degrees by week 4
- 120+ degrees by week 6–8
A patient who achieves these milestones consistently with good physiotherapy has a significantly better long-term outcome than one who doesn't.
Mistake 2: Pushing Too Hard, Too Soon
This is the mirror image of mistake 1, and it's almost as common. It typically happens around weeks 3 to 5, when patients start feeling noticeably better and interpret that improvement as a signal that they're ready to return to full activity. Common versions of this mistake:
- Walking much longer distances than the physiotherapist recommended.
- Climbing stairs repeatedly instead of limiting it to what's necessary.
- Resuming driving before the surgeon has cleared it.
- Returning to physically demanding work before the joint is ready.
- Attempting low-impact exercise like swimming or cycling before wound healing is confirmed.
Why this is a problem: The new knee feels better, but the supporting structures, like the muscles, ligaments, and the surrounding soft tissue, are still healing. The implant itself is still integrating with the bone. Overloading the joint before these structures are ready causes pain and swelling to spike. Worse, it can cause implant displacement or damage to the healing tissue around the prosthesis.
What to do instead: Follow your surgeon's and physiotherapist's timeline, not your neighbour's, not what you read in a WhatsApp group, and not what your own optimism is telling you. If the physiotherapist says "short walks of 10 minutes twice a day," that's what you do. If your surgeon says no driving for 6 weeks, you do not drive at 4 weeks because you feel fine.
Progress in knee replacement recovery should be steady and gradual. Sudden increases in activity almost always result in setbacks. Take the conservative path as it gets you to full recovery faster, not slower.
Mistake 3: Ignoring Warning Signs

A sports person clutching their knee in pain after a sudden twist, represented by a red light.
Some symptoms after knee replacement are normal, like swelling, bruising, discomfort with movement, clicking sounds, stiffness in the morning. But some symptoms are not normal and require prompt medical attention.
The mistake here is patients convincing themselves that something concerning is "just part of recovery" when it isn't; either because they don't want to bother their surgeon, or because they're afraid of hearing bad news, or because no one told them what to watch for.
Symptoms that need prompt evaluation - don't wait:
- Increasing redness around the wound (not just bruising — spreading redness).
- Wound discharge, especially if it's yellow, green, or foul-smelling.
- Increasing warmth at the surgical site — after the first week, the wound should be getting less warm, not more.
- Fever above 38°C.
Signs of possible blood clot (DVT):
- Significant calf swelling, tenderness, or warmth; especially if it appears suddenly.
- One leg is noticeably more swollen than the other in the calf area.
- If accompanied by shortness of breath or chest pain, call emergency services immediately as this is a pulmonary embolism.
Signs of possible implant issues:
- Pain that was improving but has suddenly and significantly worsened.
- The knee suddenly feels unstable or gives way.
- You feel a grinding or catching sensation that wasn't there before.
What to do instead: Know these warning signs before you're discharged from the hospital. Keep your surgeon's contact number easily accessible. If something seems wrong, call. Most of the time, you'll be reassured that it's normal, but the times when it isn't, catching it early makes a critical difference.
Mistake 4: Neglecting Wound Care And Nutrition
Two things patients consistently underestimate: how much proper wound care matters in the first 2–3 weeks, and how significantly nutrition affects healing speed and outcome. Wound care errors:
- Getting the wound wet before it's healed and approved by the surgeon.
- Not checking the wound daily for warning signs.
- Removing the dressing without instruction.
- Applying creams, oils, or home remedies to the wound without medical approval.
The surgical wound after knee replacement is large, and it's the entry point through which infection can reach the prosthesis. An infected knee implant is one of the most serious complications in orthopedic surgery, as it typically requires a second operation to clean or remove the prosthesis. Proper wound care dramatically reduces this risk.
Nutritional neglect: Patients often focus entirely on their knee and forget that the entire body is healing from a major surgery. Poor nutrition slows everything down, like tissue repair, muscle building, bone integration of the implant, and immune function.
What to eat more of after knee replacement:
- Protein - Eggs, dal, paneer, chicken, fish. The body uses protein to repair tissue. Most post-surgical patients are protein-deficient without even realising it.
- Vitamin C - Amla, citrus fruits, guava. Essential for collagen formation and wound healing.
- Vitamin D and calcium - Important for bone health and implant integration. Supplement if deficient (very common in Noida given indoor lifestyles).
- Iron - Surgery causes blood loss, and iron supports red blood cell production and energy. Palak, jaggery, lentils.
- Water - Dehydration causes fatigue, muscle cramps, and constipation (a real problem when you're less mobile and taking pain medication).
What to reduce:
- Excessive salt as it worsens swelling.
- Highly processed foods and refined sugar as they promote inflammation.
- Alcohol interferes with medication and healing.
Mistake 5: Abandoning Follow-Up Appointments
Patients feel better. The pain is down, the walking is good, physiotherapy is going well. And so the follow-up appointment scheduled at 6 weeks or at 3 months gets postponed, skipped, or forgotten. This is a mistake for several important reasons. Follow-up appointments are when your surgeon:
- Takes an X-ray to confirm that the implant is seated correctly and the bone is integrating properly.
- Assesses your range of motion against expected milestones and identifies any correction needed.
- Checks for subtle signs of problems that you might not have noticed.
- Clears you for the next stage of activity (driving, returning to work, resuming exercise).
- Adjusts your physiotherapy programme based on your actual progress.
Implant loosening, early scar tissue formation, and subclinical infections can all be identified and addressed at a follow-up appointment before they become major problems. Caught late, these conditions require much more significant intervention.
What to do instead: Treat follow-up appointments as part of the treatment, not an optional extra. Your surgeon has structured them at specific intervals for clinical reasons. Keep them even if you feel completely fine. The typical follow-up schedule after knee replacement is:
- 2 weeks (wound check and stitch removal)
- 6 weeks (mobility assessment, X-ray, activity clearance)
- 3 months (progress review)
- 6 months (recovery assessment)
- Annual (implant check and long-term monitoring)
A Note On Indian-Specific Considerations
Patients in Noida and across India face some specific challenges that aren't always addressed in general knee replacement guides.
Sitting cross-legged (Padmasana/sitting on the floor): Many Indian patients, for prayer, cultural habits, or simply household routines, want to sit cross-legged on the floor. This requires deep knee flexion (typically 120+ degrees) and puts significant stress on the joint. It is generally not recommended until at least 3–6 months post-surgery and only when range of motion is clearly adequate. Discuss this specifically with your surgeon before attempting it.
Using an Indian-style toilet (low-seated): This is an early challenge. Using a Western-style raised toilet seat in the first 6–8 weeks is strongly advised. Indian-style toilets require deep squatting that the new knee cannot manage safely in the early recovery phase.
Attending religious events: If you need to go to a mandir or religious gathering that involves floor seating or removing footwear and walking on uneven surfaces, plan this carefully. Wearing supportive footwear wherever possible, using a walking stick, and avoiding crowded situations where you might be jostled are all important precautions.
The Bottom Line

A male patient is sitting with a knee brace and a female doctor is examining it.
Knee replacement works. It works remarkably well when the surgery is performed correctly, and the recovery is managed properly. These five mistakes don't ruin outcomes for everyone, but they do limit them. They turn what could be a very good result into a merely adequate one, or they turn a manageable recovery into a complicated one.
If you're preparing for knee replacement surgery with Dr. Mayank Chauhan at Prakash Hospital, Sector 33, Noida, or if you have questions about your recovery, don't hesitate to ask. The team is there to help you through every stage and not just the surgery itself. To book a consultation or discuss your recovery, call the number listed on the website.