The Hidden Damage After Injury: Post-Traumatic Arthritis Explained

A man is holding his plastered arm in pain.
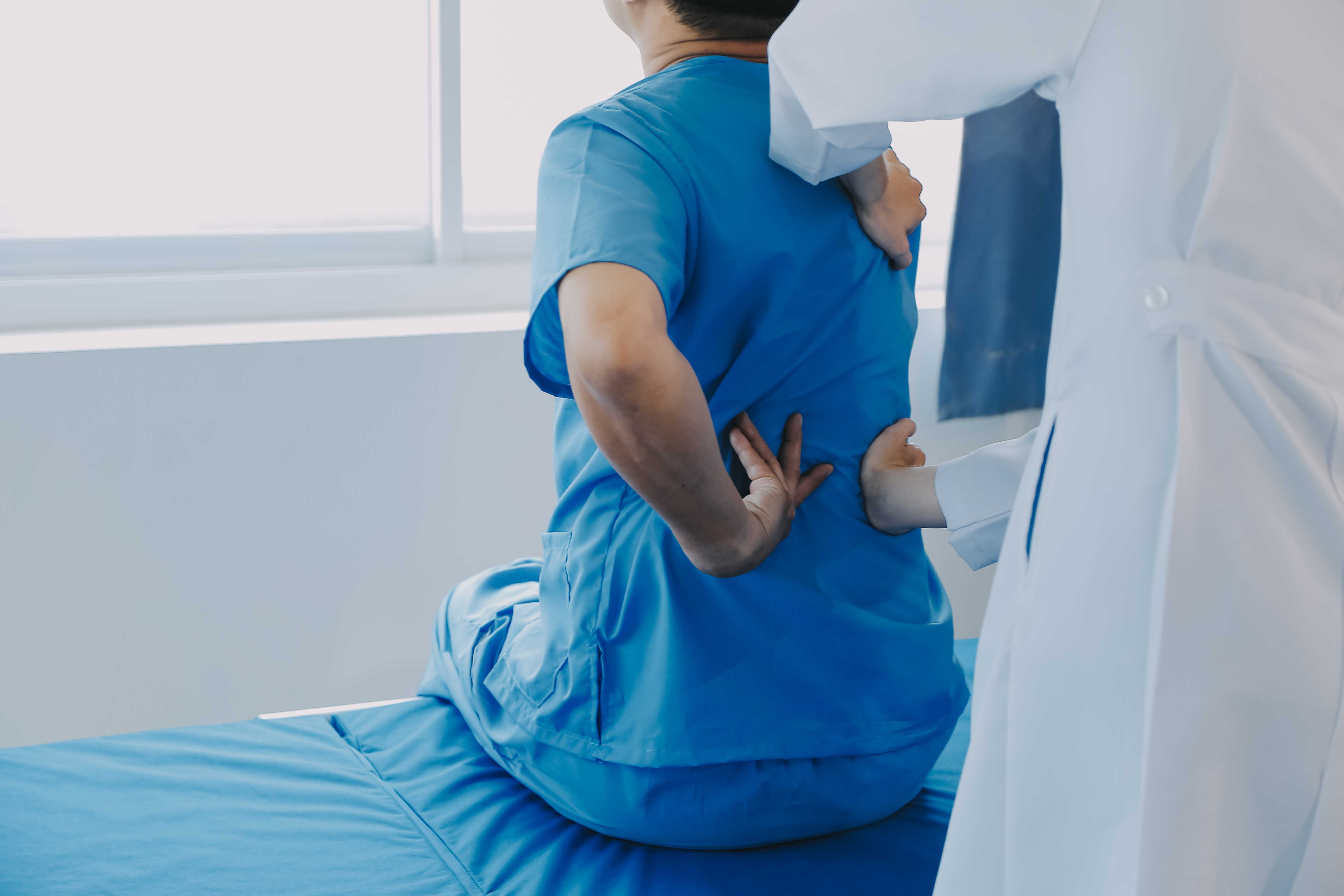
A lot of people believe that an injury is cured once the initial signs have resolved. However, it is sometimes possible for an injury to cause hidden damage that doesn't manifest itself until later in the form of post-traumatic arthritis.
Post-traumatic arthritis is a slow-developing condition caused by trauma to a joint, such as a break, sprain, or tear in the ligaments. The joint might seem to have healed, with pain resolved and movement returning, but the joint may not be working properly on the inside, and damage may build up in the joint, which could cause the joint to feel stiff and painful, swell up, and become less mobile in the long term.
It can affect not only athletes but also those with minor injuries. It is crucial to know how the condition develops as well as the signs of the problem, so that appropriate treatment can be sought. In this guide, we look in detail at what is really involved with post-traumatic arthritis and when you might want to speak to an orthopaedic specialist about the condition.
What is Post-Traumatic Arthritis?
Post-traumatic arthritis (PTA) is defined as arthritis that develops secondary to a traumatic event occurring at a joint. It can present months or years following a previous injury. Following injury, wear and tear on the articular cartilage covering the joint surfaces, as well as slight alteration in alignment and stability, results in an increased breakdown rate of cartilage, which subsequently leads to pain, swelling, and diminished mobility. Post-traumatic arthritis, unlike age-related OA, has a direct cause (a previous trauma) and emphasizes the critical need for immediate management and follow-up of joint injuries.
How Post-Traumatic Arthritis Develops?
There may be imperfect healing after the injury. This means that although the joint surface may look alright, there could still be damage in the joint's depths.
- Cartilage Damage - The cartilage that lines your joint surfaces and allows smooth movement may deteriorate at an increased rate following injury.
- Joint Instability - Damage to ligaments means that the joint could be less stable, causing more stress when moved.
- Inflammation - There may be inflammation inside the joint lasting over time due to the response to injury.
- Misalignment - If fractures do not heal perfectly straight, it alters the weight-bearing load on the joint surfaces.
Common Symptoms To Watch For
In post-traumatic arthritis, the symptoms develop insidiously-they may creep up unnoticed and are only diagnosed relatively late. The usual signs and symptoms include:
- Joint pain - It tends to be intermittent at first and then slowly increases in frequency and intensity
- Stiffness - Initially most noticeable when you first get up in the morning or after long periods of rest
- Swelling - Can be intermittent or continuous.
- Lowered range of movement - The joint moves through a lesser range of motion compared to before the injury.
- Grinding/rubbing sensation - A feeling of movement against some grit or of rubbing while the joint is moved.
An awareness of the initial symptoms will greatly contribute to the control and effective management of the condition. Seeing an orthopedics specialist, such as Dr. Mayank Chauhan in Noida, is essential for a correct diagnosis and appropriate treatment for effective symptom control and prevention of further joint damage.
Joints Most Commonly Affected
The joints most frequently affected are those most frequently injured, generally bearing weight or being actively used every day.
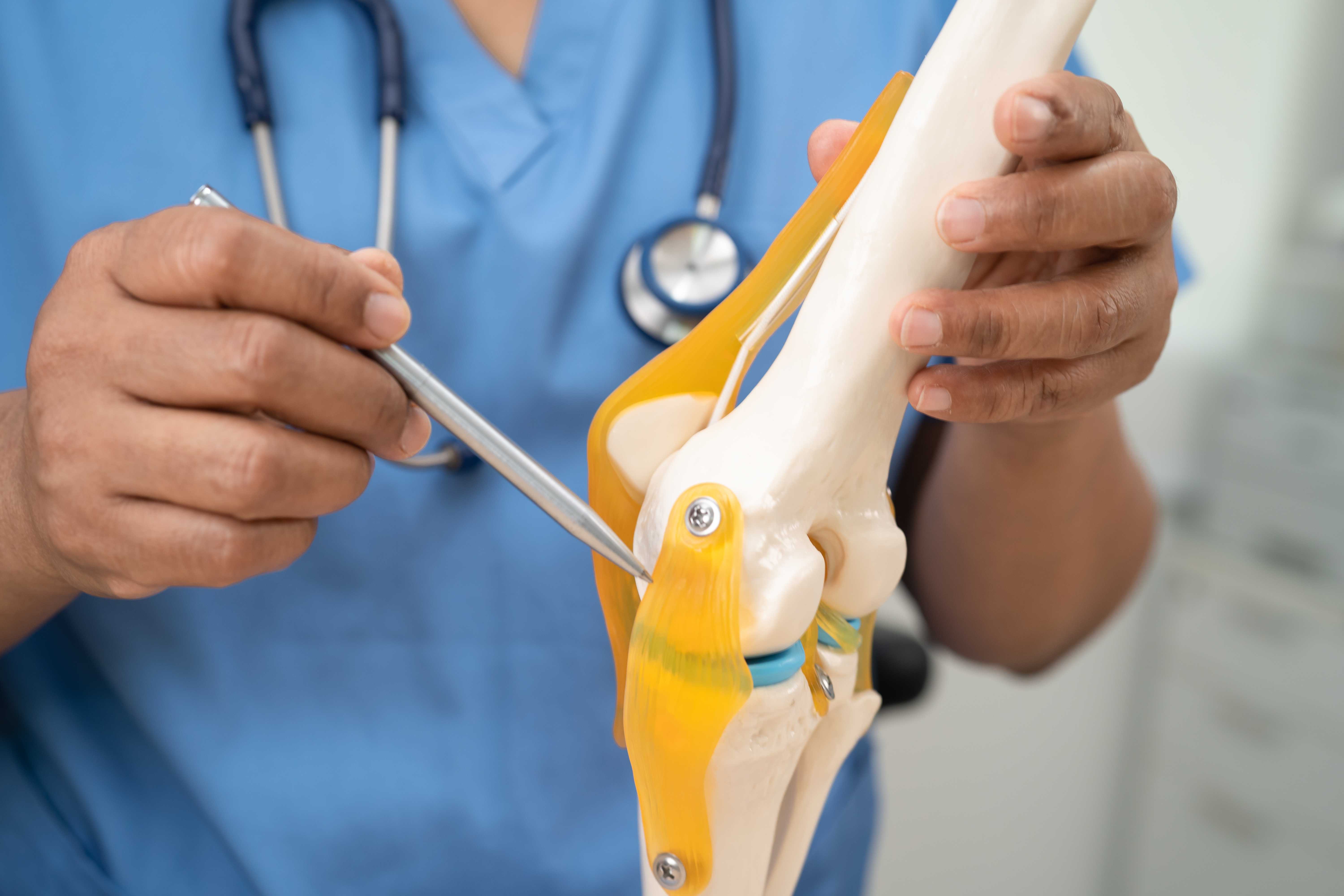
1. Knee Joint

A man is holding his knee.
It is one of the joints most frequently damaged from sports injuries and accidental injuries. The knee supports your weight, and you use it in nearly every movement-walking, running, and climbing up the stairs, hence when there is even slight damage, it tends to wear out quickly with time.
2. Ankle Joint
Sports injuries such as sprains can lead to long-term ankle joint issues. Recurrent damage from repeated twisting or instability weakens the joint, leading to cartilage damage and chronic pain.
3. Hip Joint
Dislocations and fractures of the hip joint make it prone to arthritis over time. As it supports your weight and is used in most body movements, malalignment after an injury tends to cause problems in the smoothness of the movement.
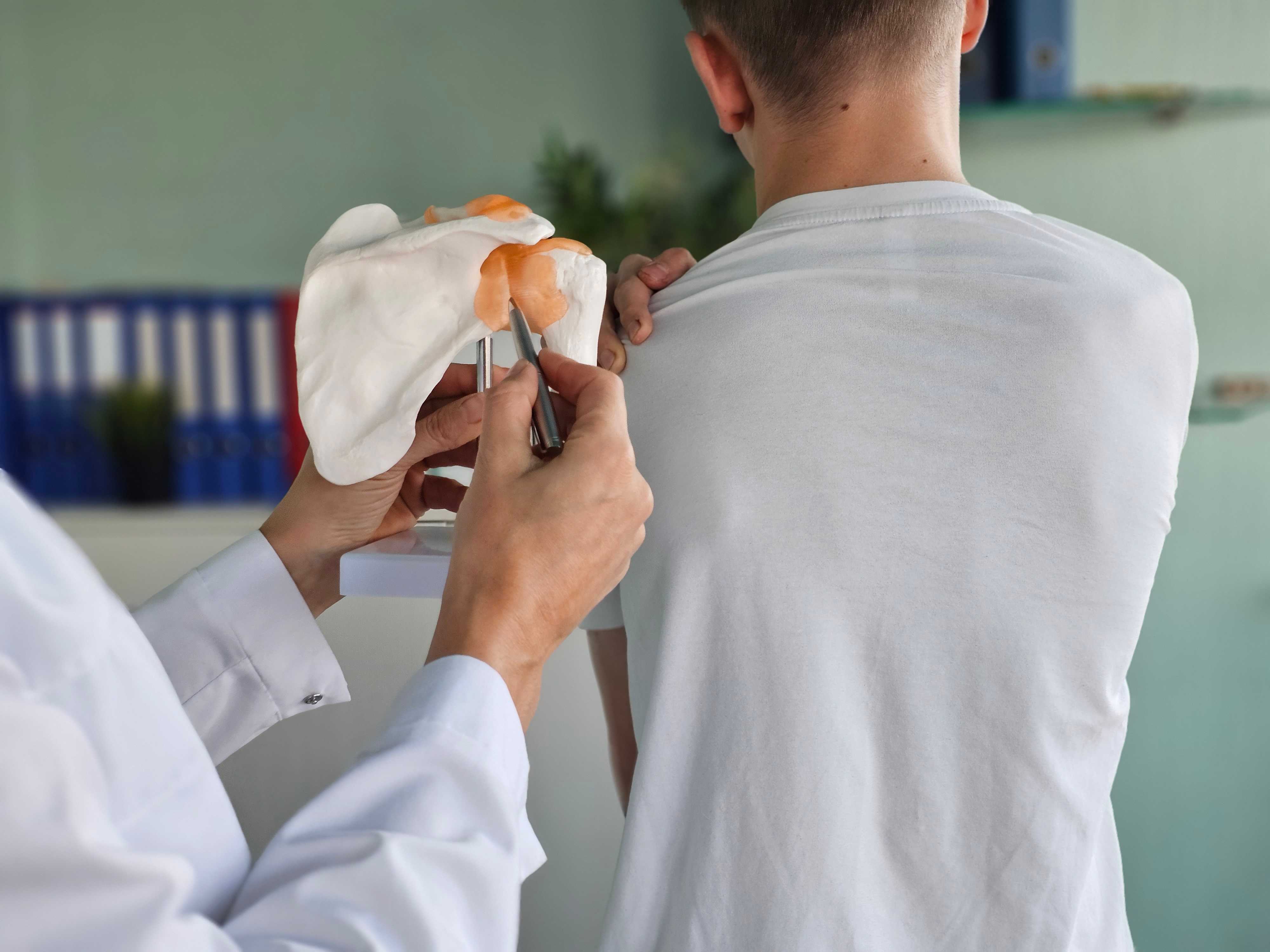
4. Shoulder Joint
Repeated injuries at this joint are likely to cause degeneration of the shoulder. It has a greater range of movement, and any laxity present in the joint structure after an injury is more likely to have damaging effects with time.
Risk Factors For Post-Traumatic Arthritis
Some factors put a person at higher risk for post-traumatic arthritis after an injury:
- Serious joint injury - A fracture or torn ligament can greatly increase the risk.
- Poor alignment after injury - Rehabilitation is incomplete, or there is poor alignment.
- Re-injury - Repeated injury of the same joint reduces its structure.
- Extra body weight - Additional weight on a stressed joint.
- Strenuous activities - Activities that put a great deal of stress on the joints.
Treatment Options For Post-Traumatic Arthritis
Treatment for post-traumatic arthritis centers on reducing pain and improving joint movement while slowing the rate of damage to the joint. Treatment choices vary in accordance with the severity and the functional impact on day-to-day living activities.
Management via non-surgical means. Many cases of post-traumatic arthritis will initially respond to non-surgical treatments to ease pain and enhance the function of the joint. If non-surgical forms of management prove to be unsuccessful in controlling pain that significantly impedes day-to-day tasks, surgical options will be considered.
1. Medication
Pain relievers and anti-inflammatories should be prescribed to help reduce pain and swelling. Medications cannot cure the underlying problem, but they alleviate the symptoms sufficiently to make day-to-day movements easier and pain-free, particularly flare-ups.
2. Physiotherapy
It is particularly effective at strengthening the muscles supporting the damaged joint in order to increase stability, reduce pressure on the damaged joint itself, and facilitate range of motion, smoothing out movements and decreasing pain levels.
3. Lifestyle Modifications
Many simple adjustments to day-to-day life may significantly improve quality of life and pain levels. Weight loss can make a significant impact by decreasing the pressure on load-bearing joints, such as the knees and hips. Minimizing involvement in high-impact activity and adopting lower-impact forms of exercise (e.g., walking and swimming) is of great importance in reducing wear and tear on the joint.
4. Support Devices
Braces, orthotics, or artificial supports are devices that can be worn on the joint to aid mobility. They improve stability and help the weight distribution be more even throughout the joint to lessen the stress imposed upon the affected joint during activity or prolonged standing.
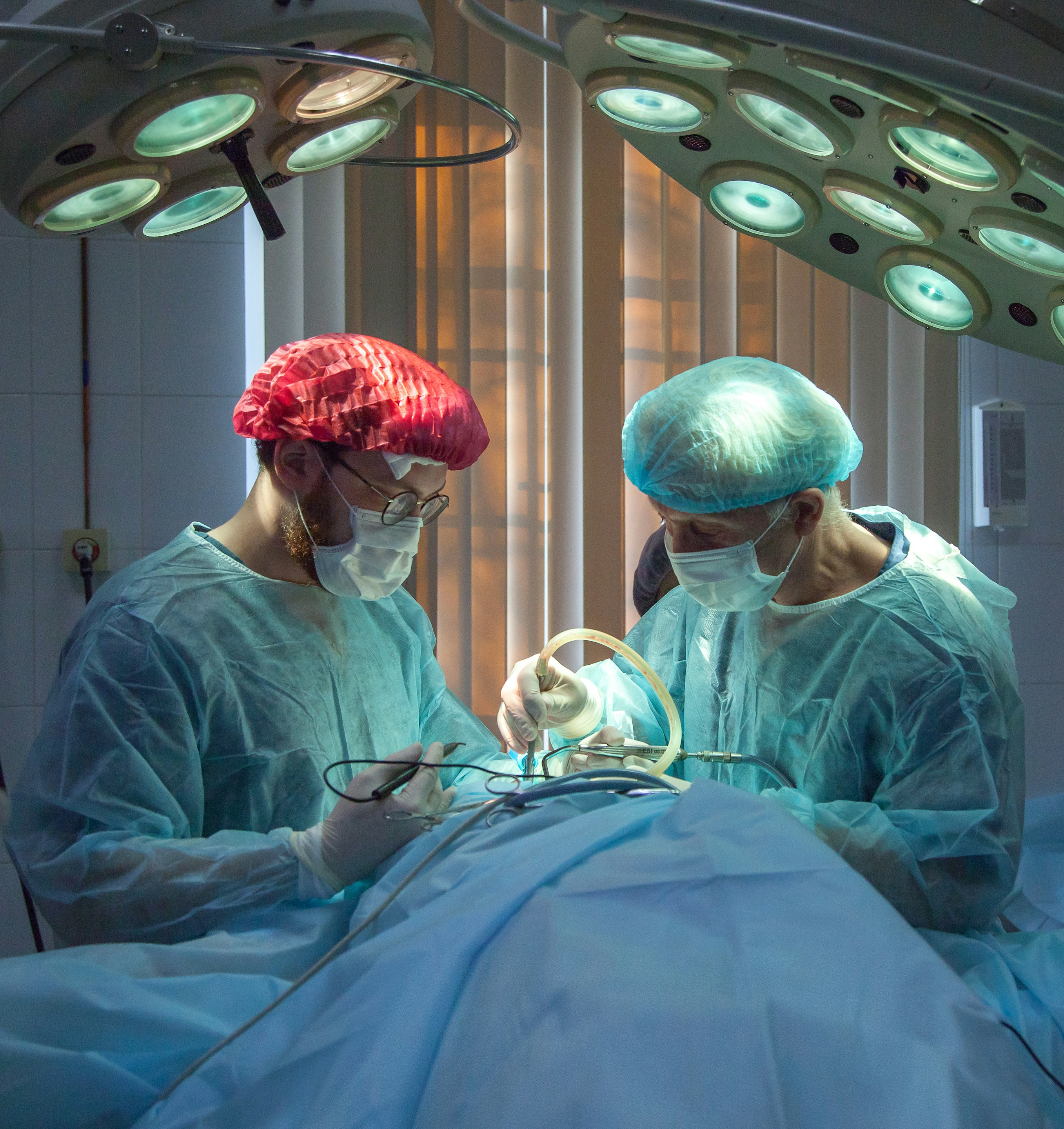
5. Arthroscopy

Diagram of knee arthroscopy using surgical instruments.
This is an operation that involves using a small camera and tools to clear the joint. In doing so, the loose bits of cartilage are removed, the rough surfaces of the bone are smoothed down, and inflammation is removed from within the joint; this results in a better and less painful range of movement.
6. Osteotomy
If, following the injury, the joint becomes so misshapen that weight bearing occurs primarily through the damaged region, this procedure is employed. By changing the orientation of the bone surfaces, weight is re-apportioned across the whole of the joint, thus reducing the strain on the area of damaged bone and delaying the necessity of joint replacement.
7. Joint Replacement
This is for the very severely degenerated joint. Here, artificial bearing surfaces are used instead of the biological ones, and this should provide the best possible functional capacity and a reduction in the level of pain, and so an increase in quality of life when other treatments are no longer sufficient.
How To Prevent Further Joint Damage
It's not always possible to prevent post-traumatic arthritis altogether, but it can be managed.
- Full rehabilitation - It is important to make a full recovery after a traumatic injury to minimize any long-term complications.
- Stay active - Low-impact activity can keep your joints supple and strong
- Keep your weight healthy - Excessive weight adds unnecessary strain to your joints
- Avoid overloading the joint - Don't carry on putting stress on the affected joint in the way that caused the injury in the first place.
- Address symptoms early - Take notice of the signs below before the joint is damaged permanently.
When To Visit An Orthopedic Specialist
Your body will give signs when things aren't quite right, and you should take note of these signs:
- If there is persistent pain after the injury.
- A joint that becomes increasingly stiff, and this starts to limit everyday activities.
- Swelling that reoccurs at a particular joint.
- Every day movements are difficult and painful.
Final Thoughts
Post-traumatic arthritis serves as an important reminder that not all injuries end when the discomfort disappears. It’s also crucial to know that some of these injuries will accumulate in the body quietly and silently, and may have long-term implications for the health of the joints.
Ensuring proper handling of injuries and rehabilitation of any damage caused, and being aware of the signs and symptoms, can be highly influential. The quicker the symptoms are handled, the better the long-term outcomes.
Undergoing a diagnostic process from an experienced orthopedic professional, such as Dr. Mayank Chauhan, Noida, ensures that a systematic treatment plan is formulated and executed efficiently. Through expert consultation, individuals will experience optimal results to keep their joints pain-free and active in the years to come.
Frequently Asked Questions (FAQs)
1. Can post-traumatic arthritis develop years after an injury?
Yes, it may develop months or even years after the joint has been injured.
2. Is post-traumatic arthritis a permanent condition?
It is a condition with long-term consequences, although its symptoms can be very successfully managed by appropriate treatment.
3. Can exercise have an impact on post-traumatic arthritis?
Low-impact exercises can improve joint flexibility and muscle strength.
4. How is post-traumatic arthritis diagnosed?
It may be diagnosed by a physician through a combination of physical examination, patient history, and an X-ray or MRI.