Slip Disc Causes, Symptoms and Treatment in Noida

Medical illustration showing a herniated spinal disc pressing on a nerve, with some diagrams of a human body showing the spine and areas of pain in the back.
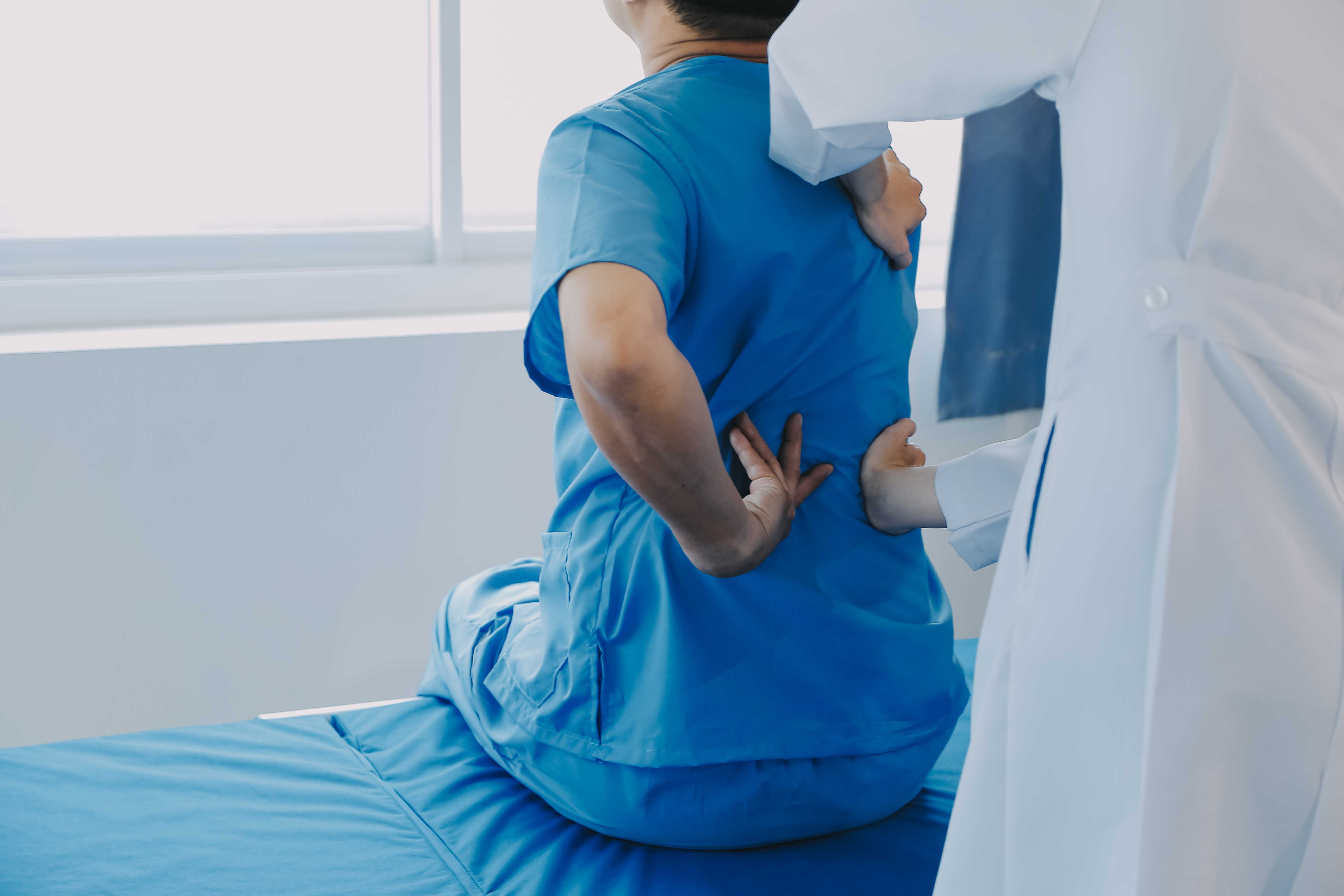
There's back pain, and then there's this — the kind of pain that starts in your lower back and then, one day, travels down your hip, through your thigh, and sometimes all the way to your foot. You might feel a burning sensation, or sharp electric shocks with certain movements. Sometimes it's numbness. Sometimes it's weakness. You try rest. You try a hot water bottle. You try ignoring it. None of it really works.
That pattern — back pain with radiating leg symptoms — is one of the most recognisable signs of a slip disc. And it's far more common in Noida, Greater Noida, and Delhi NCR than most people realise, particularly among working adults who spend long hours sitting at desks, driving, or doing repetitive physical work.
This guide explains what a slip disc actually is, why it happens, what the symptoms tell you, and what treatment looks like in 2025 — from the most conservative options all the way to surgery.
What Is a Slip Disc?
The term "slip disc" is widely used in India but medically imprecise. The disc doesn't actually slip out of place. What happens is this:
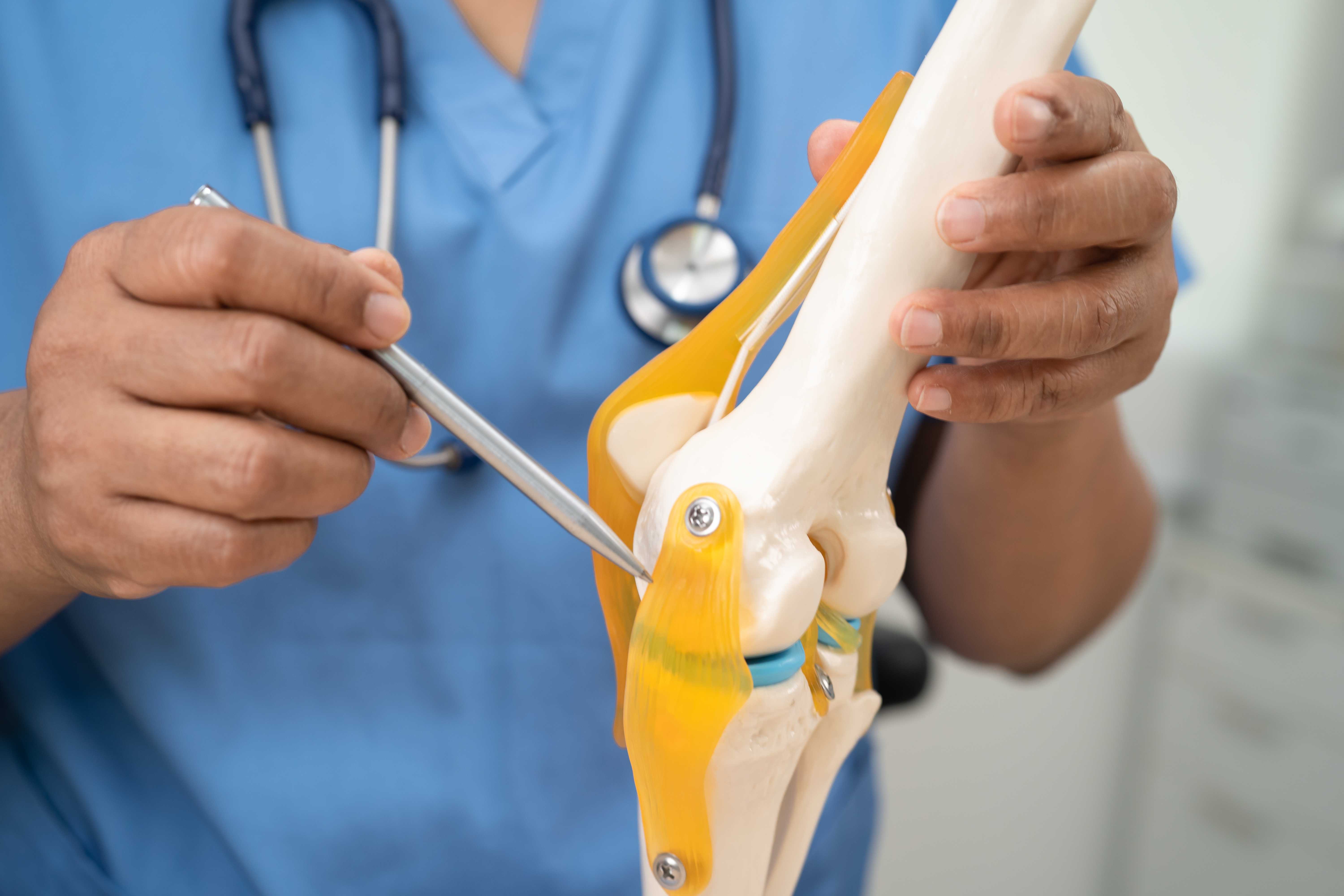
Your spine is made up of vertebrae — the bones of your backbone — stacked on top of each other. Between each pair of vertebrae sits a disc: a small, round cushion with a tough outer ring (called the annulus fibrosus) and a soft, gel-like centre (called the nucleus pulposus). These discs act as shock absorbers for the spine, allowing it to bend, rotate, and carry load without the bones grinding together.
A slip disc occurs when the soft inner gel pushes through a crack or tear in the outer ring. This is medically called a herniated disc, prolapsed disc, or PIVD (Prolapsed Intervertebral Disc). When the gel-like material presses against nearby spinal nerves, it causes pain, numbness, tingling, and sometimes weakness in the areas supplied by those nerves.
Most slip discs occur in the lower back (lumbar spine), particularly at the L4-L5 and L5-S1 levels — the two discs that bear the greatest load during sitting and lifting. Cervical (neck) disc herniation also occurs and typically causes symptoms in the arm and hand rather than the leg.
Why Does a Slip Disc Happen?
Disc herniation doesn't usually happen because of a single dramatic event. In most cases, the disc has been weakening slowly over time, and it eventually gives way — sometimes from something as ordinary as bending to pick up a bag.
The most common causes and risk factors:
1. Prolonged Sitting With Poor Posture
If you work in a Noida office, spend hours commuting on the Delhi Metro or in a car, or work in an environment that keeps you seated all day — you're putting sustained pressure on your lumbar discs. Over time, this compresses the disc and weakens the outer ring.
2. Improper Lifting
Bending at the waist and lifting heavy objects puts enormous shear force on the lumbar spine. The correct way to lift is by bending the knees and using the legs — a habit most people never develop.

An athlete executes a deadlift with controlled knee bend and proper hip hinge in an indoor gym.
3. Age-Related Disc Degeneration
Discs contain water. As we age, they lose hydration and flexibility — they become less able to absorb shock and more prone to cracking. Most people begin experiencing some disc degeneration by their 30s and 40s, even without symptoms.
4. Obesity
Excess body weight increases the constant load on spinal discs. Combined with poor posture and physical inactivity, it significantly raises the risk of disc herniation.
5. Smoking
Less talked about, but smoking reduces blood supply to spinal discs, which accelerates their degeneration.
6. Sudden Physical Strain
A heavy lift, a fall, a sudden twist — any of these can push a weakened disc over the edge.
7. Genetics
Disc structure and degeneration patterns are partly hereditary. Some people are simply more predisposed to disc problems than others.
The 4 Stages of Disc Herniation
A herniated disc doesn't happen all at once. There's a progression
Stage 1 — Disc Bulge: The outer ring weakens and bulges outward, but remains intact. Often causes mild or no symptoms.
Stage 2 — Disc Protrusion: The soft inner gel begins to push against the outer ring, which is still intact. Symptoms become more noticeable.
Stage 3 — Disc Extrusion: The inner gel breaks through the outer ring and enters the spinal canal, but remains connected to the disc. This is when nerve compression becomes significant and symptoms are typically severe.
Stage 4 — Disc Sequestration: A fragment of the disc material breaks free into the spinal canal. This can cause significant nerve compression and often requires medical intervention.
Symptoms: What a Slip Disc Actually Feels Like
The symptoms depend on which level of the spine is affected and which nerve is being compressed.
1. Lumbar Slip Disc (Lower Back) — Most Common
Sciatica is the hallmark symptom — pain that radiates from the lower back, through the buttock, down the back of the thigh, and sometimes into the calf and foot. It usually affects one leg.
Other symptoms include:
- A dull, constant ache in the lower back
- Sharp pain when coughing, sneezing, or straining
- Tingling or pins-and-needles in the leg or foot
- Numbness in parts of the thigh, leg, or foot
- Weakness in the foot or leg (difficulty lifting the foot, called "foot drop," in severe cases)
2. Cervical Slip Disc (Neck)
- Pain radiating into the shoulder, arm, forearm, or hand
- Numbness or tingling in the fingers
- Weakness in the arm or grip
- Neck pain that worsens with certain head positions
3. Red Flags — Seek Urgent Medical Attention
These symptoms require same-day medical evaluation:
- Loss of bladder or bowel control — this is a medical emergency (cauda equina syndrome)
- Sudden severe weakness in both legs
- Numbness in the inner thighs and groin area
These are not symptoms to wait and see about.
How Is a Slip Disc Diagnosed?
A proper diagnosis involves more than just telling the doctor your symptoms.
Physical examination: The surgeon will check your reflexes, muscle strength, and sensation. They'll perform specific tests — like the Straight Leg Raise — that help identify which nerve is compressed.
MRI scan: This is the gold standard for diagnosing a disc herniation. An MRI shows the soft tissues — discs, nerves, spinal cord — in detail. It confirms the level of herniation, the direction, and the degree of nerve compression.
CT scan: Sometimes used when MRI isn't available or when bony details need closer examination.
X-ray: Does not show discs directly, but helps rule out other causes of back pain like fractures or tumours.
Slip Disc Treatment Options
The good news: the vast majority of slip disc cases — estimated at 80–90% — resolve with non-surgical treatment over 6 to 12 weeks. Surgery is needed for a minority of patients, and the decision to operate is based on specific criteria.
1. Non-Surgical Treatment
Rest (Short-Term)
Complete bed rest for extended periods is no longer recommended. Short rest (1–2 days) during the acute pain phase is acceptable, but staying active with modified movements is better for recovery.
Medication
Anti-inflammatory medications (NSAIDs like ibuprofen or diclofenac) reduce inflammation around the nerve. Muscle relaxants help with spasm. In more severe cases, short courses of oral steroids or nerve pain medications (like pregabalin or gabapentin) are used.
Physiotherapy
Targeted exercises — particularly the McKenzie method for lumbar disc herniation — help retract the disc material and reduce nerve pressure. Physiotherapy also strengthens the core muscles that support the spine, reducing recurrence risk.

A woman in a physiotherapy session, guided by a therapist who helps her perform controlled exercises or stretches.
Epidural Steroid Injections
When pain is severe and not responding to medication, an injection of corticosteroid directly around the compressed nerve (under imaging guidance) can provide significant relief and allow physiotherapy to progress.
Traction
Mechanical traction gently pulls the spine apart, creating negative pressure inside the disc that may help draw the herniated material back. Results vary by patient.
2. Surgical Treatment
Surgery is considered when:
- Conservative treatment has been tried for 6+ weeks without adequate improvement
- Pain is severe and significantly disabling
- There's progressive neurological deterioration (worsening weakness or numbness)
- Bladder or bowel symptoms are present (this is an emergency)
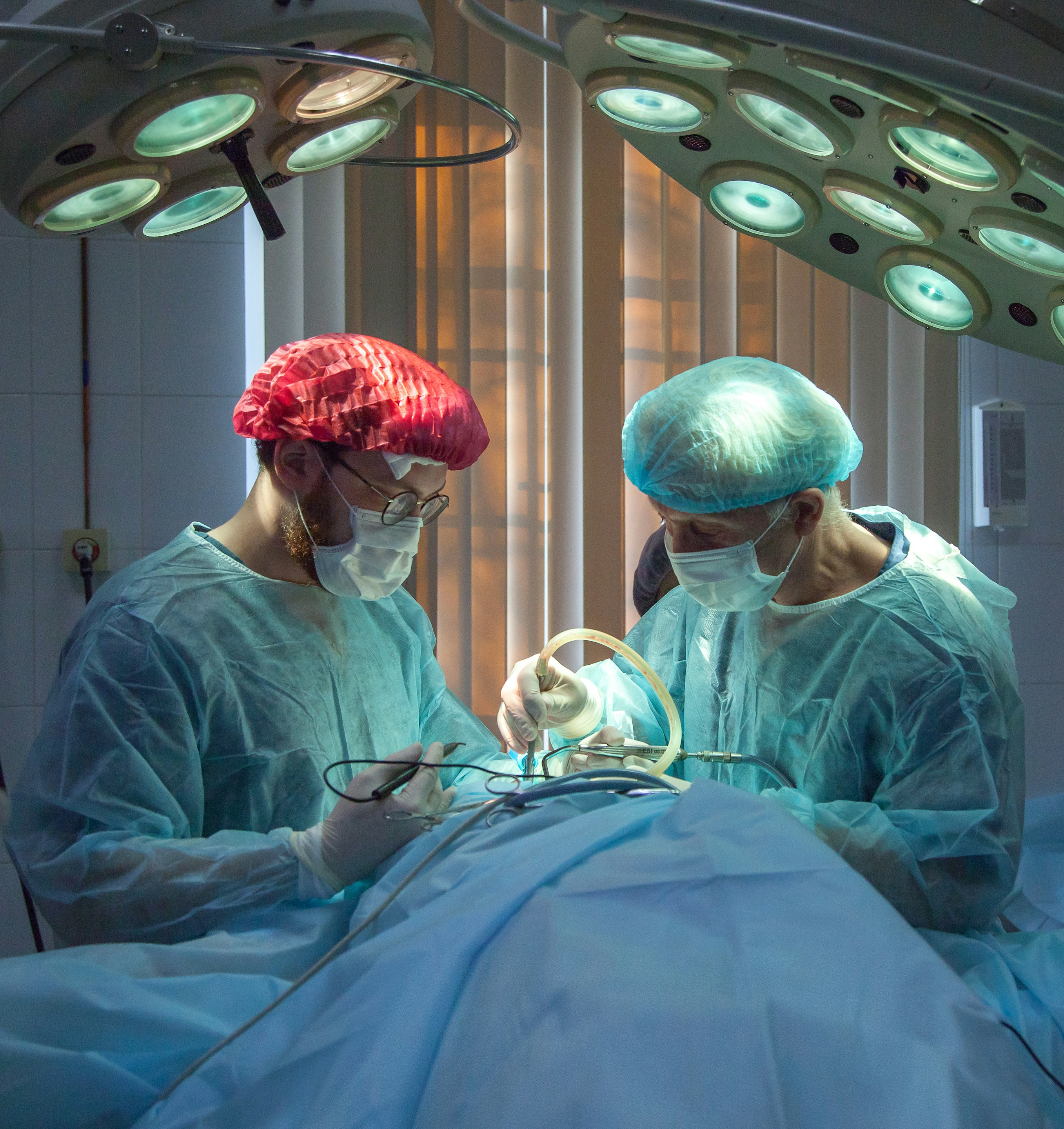
Microdiscectomy is the most common surgery for lumbar disc herniation. A small incision is made, and the herniated disc fragment pressing on the nerve is carefully removed. The recovery is significantly faster than open surgery — most patients walk the same day and are discharged within 2–3 days. Success rates are high.
For cervical disc herniation, procedures include anterior cervical discectomy and fusion (ACDF) or disc replacement surgery.
Slip Disc Treatment in Noida
Noida has seen a significant rise in slip disc cases over the past decade — driven by the city's growing corporate sector, long commutes, sedentary desk jobs, and the overall pace of urban life that doesn't leave much room for spinal health.
Dr. Mayank Chauhan, Senior Orthopedic Surgeon at Prakash Hospital, Sector 33, Noida, treats both lumbar and cervical disc herniation with a structured, step-by-step approach. The goal is always to try the least invasive path first — medication, physiotherapy, injections — and reserve surgery for patients who genuinely need it.
If you've had back pain with leg symptoms for more than 3–4 weeks, or if the pain is severe enough to affect your sleep or daily function, it's worth getting a proper evaluation. A physical examination and an MRI will tell you exactly where things stand.
To book a consultation with Dr. Mayank Chauhan in Noida, call the number listed on the website.
Can a Slip Disc Heal on Its Own?
This is the question most patients want answered first.
Yes — in many cases, the herniated disc material gradually reabsorbs over time. The body has a natural mechanism for breaking down the herniated tissue. Studies show that in patients who manage their symptoms conservatively, a significant percentage see complete or near-complete resolution of the disc herniation on follow-up MRI.
This process takes weeks to months. During that period, the goal of treatment is to manage pain, keep the patient functional, and prevent the disc from herniating further.
Preventing Recurrence
Once you've had a disc herniation, the risk of it happening again is real — unless you make some changes. The most effective long-term protection is:
- Core strength: Strong abdominal and back muscles take load off the spinal discs. Regular physiotherapy and targeted exercises are non-negotiable after a disc episode.
- Correct posture: At a desk, in a car, while lifting. This is a daily habit, not a one-time fix.
- Weight management: Every kilogram of excess weight adds pressure to spinal discs.
- Regular movement: Staying seated for hours at a stretch is one of the worst things you can do for disc health. Stand up, walk, stretch — every 45 minutes is ideal.
The Bottom Line
A slip disc is uncomfortable, sometimes severely so. But it's not a life sentence. Most patients recover fully with the right treatment and the right habits. The ones who struggle tend to be those who ignore symptoms too long, skip physiotherapy, or return to the same patterns that caused the problem in the first place.
If you're in Noida or Greater Noida and experiencing back pain with radiating leg symptoms, don't wait for it to get worse. Get evaluated, get the right diagnosis, and start treatment properly.
To book a consultation with Dr. Mayank Chauhan, Senior Orthopedic Surgeon in Noida, call the number listed on the website.