Rheumatoid Arthritis Vs Osteoarthritis - Key Differences And How Each Is Treated

Showing the inner bone structure of a person.
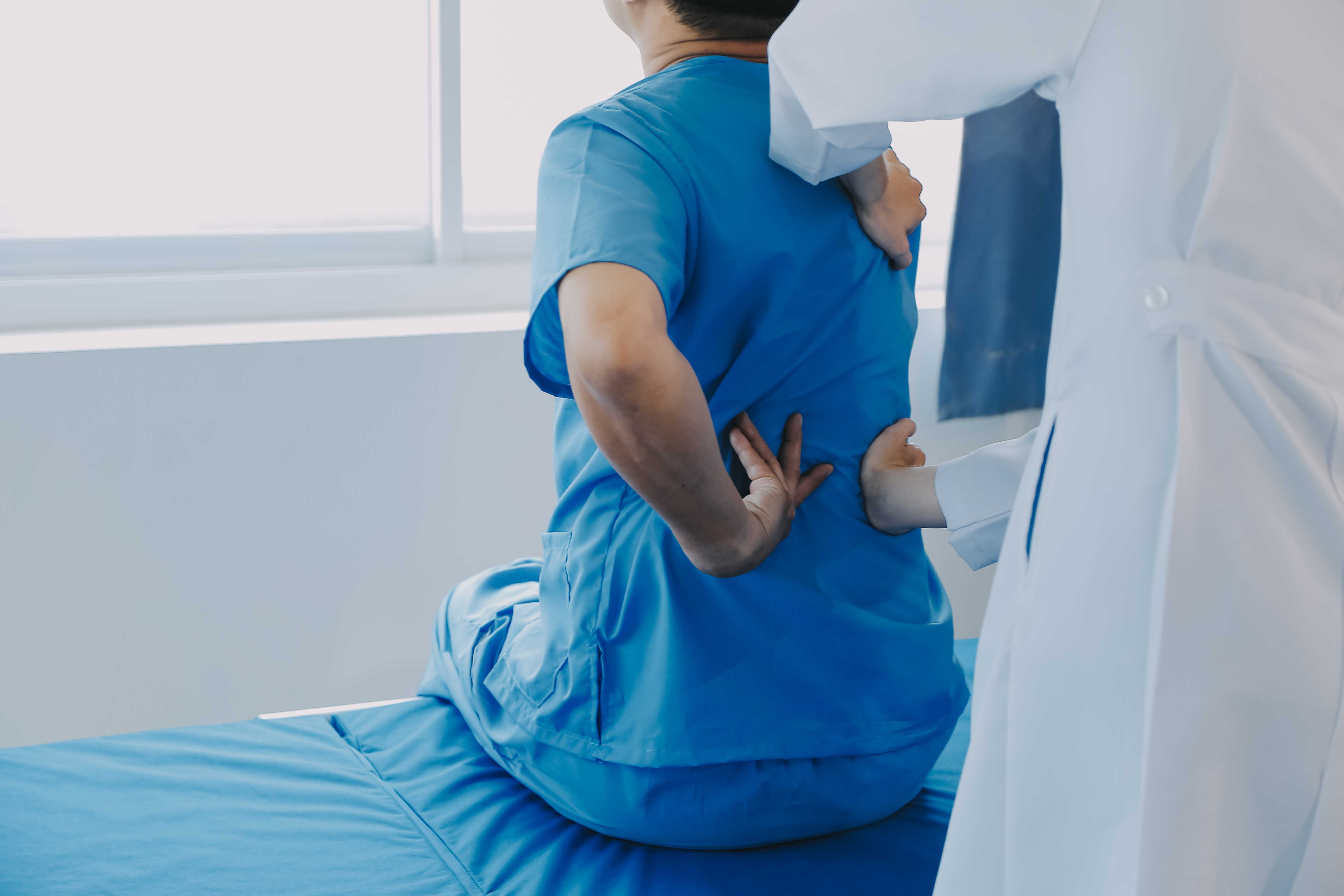
Joint pain and stiffness. Both conditions cause them. Both are called "arthritis." Both affect millions of people in India. And yet treating one the way you'd treat the other is one of the most common and most costly mistakes in orthopedic care.
Rheumatoid arthritis and osteoarthritis share a name and some surface-level symptoms, but they are fundamentally different diseases. One is a mechanical problem; the joints are wearing out. The other is an immune system problem, where the body attacks itself. The medications that slow one do not affect the other. The surgical interventions that help one may be premature or inappropriate for the other.
Getting this distinction right is not a minor clinical detail. It's the difference between treatment that works and treatment that doesn't. This guide explains both conditions in detail, what they are, how they differ, how they're diagnosed, and how each is treated specifically in the context of patients consulting orthopedic specialists in Noida and Greater Noida.
What Is Osteoarthritis?
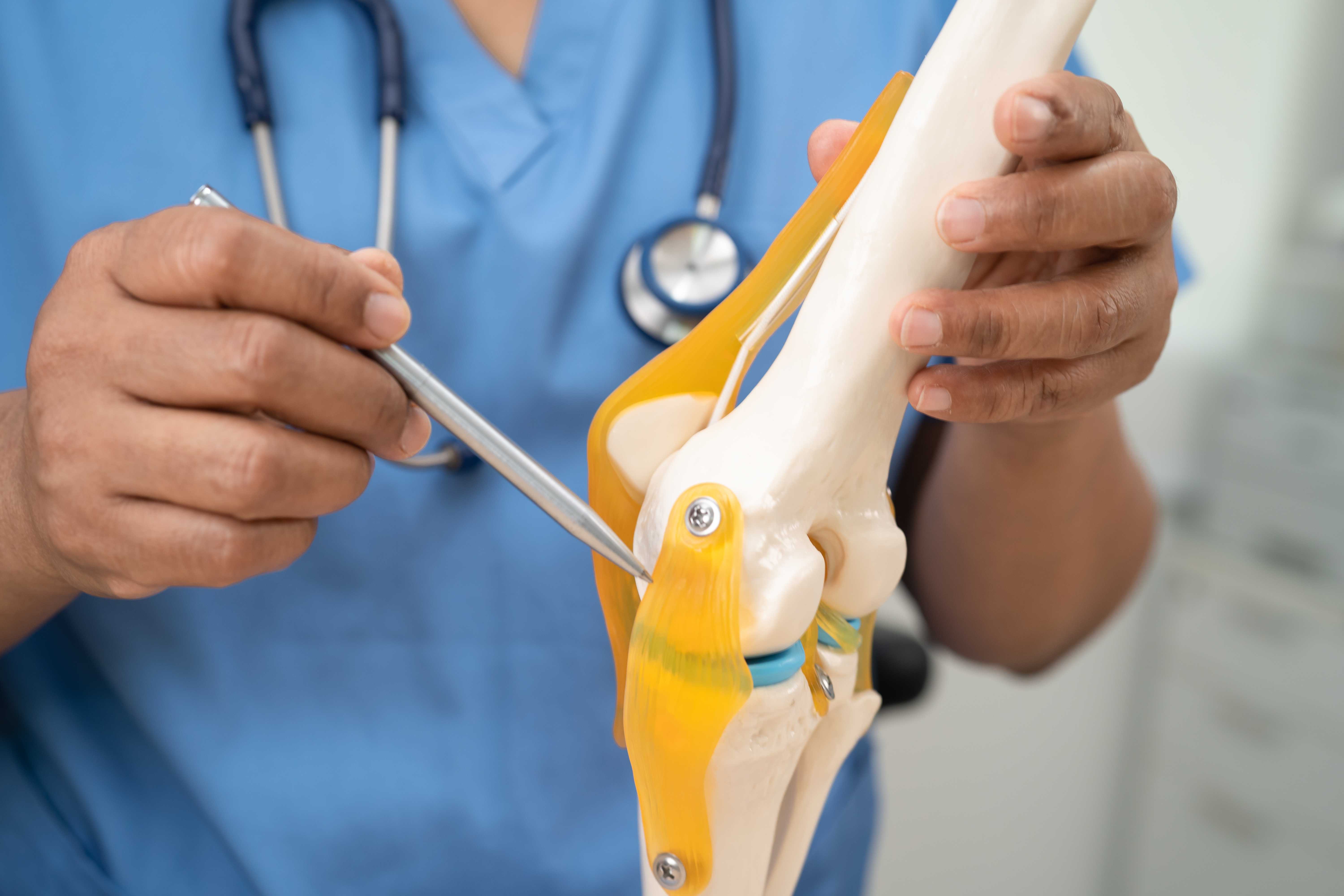
Osteoarthritis (OA) is the most common form of arthritis in the world and in India. It is a degenerative joint disease, meaning it results from the gradual breakdown of the cartilage that cushions the ends of bones. Think of healthy cartilage as a smooth, shock-absorbing surface between two bones. In osteoarthritis, the cartilage thins and cracks over time. As it erodes, the bones begin to rub against each other. This friction causes pain, swelling, stiffness, and eventually visible deformity of the joint.
OA is primarily a disease of aging and mechanical wear. It doesn't spread from joint to joint through an inflammatory process; it develops where the wear and tear is greatest. In most people, that means the knees, hips, spine, and hands. And typically more on one side than the other.
Who gets OA:
- Most commonly affects people over 50, though increasingly seen in people in their 40s.
- More common in women, especially after menopause.
- Risk increases significantly with obesity (extra load on weight-bearing joints), previous joint injuries, repetitive physical work, and family history.
- By age 70, most people have some degree of knee OA on X-ray, though not all of them have significant symptoms.
What Is Rheumatoid Arthritis?
Rheumatoid arthritis (RA) is an autoimmune disease. The immune system, which normally protects the body from infections, mistakenly identifies the synovium (the thin membrane lining the joints) as a threat and attacks it. This immune attack causes chronic inflammation inside the joint. Over time, that inflammation damages cartilage, bone, and the surrounding tissues.
RA is not about mechanical wear. It's about the immune system misfiring. This is why RA is systemic; it doesn't just affect joints. It can affect the lungs, heart, eyes, and blood vessels. It causes fatigue and a general feeling of being unwell that goes beyond joint pain. And it can progress rapidly if not treated with the right medications.
Who gets RA:
- Affects approximately 0.5–1% of the Indian population.
- Women are 2–3 times more likely to develop RA than men.
- Can develop at any age, including in young adults and, rarely, in children (juvenile idiopathic arthritis).
- Has a genetic component but is not directly hereditary.
- Onset can be gradual or sudden.
The Critical Differences - Side By Side
1. Cause
- OA: Mechanical wear and cartilage breakdown. Not an inflammatory disease at its core, though secondary inflammation occurs.
- RA: Autoimmune. The immune system attacks the joint lining directly.
2. Pattern of Joint Involvement
- OA: Asymmetric. May affect the right knee more than the left, or one hip more than the other. Large weight-bearing joints (knees, hips) and the spine are most common.
- RA: Symmetric. When the right wrist is involved, the left wrist is typically involved too. Starts in smaller joints — fingers, wrists, feet before progressing to larger joints.
3. Morning Stiffness Duration
This is one of the most useful clinical distinguishing features:
- OA: Morning stiffness typically resolves within 30 minutes of getting up and moving.
- RA: Morning stiffness lasts more than 1 hour, often described as the joints needing a long time to "warm up" before functioning normally.
4. Systemic Symptoms
- OA: A joint disease. No fever, no significant fatigue, no effect on other organs.
- RA: A systemic disease. Fatigue is a prominent and often debilitating symptom. Low-grade fever during flares. Can affect the heart, lungs, eyes, and skin.
5. Speed Of Onset
- OA: Develops gradually over years and decades. Patients often notice pain building slowly and attribute it to "ageing."
- RA: Can develop within weeks to months. Sometimes begins suddenly with acutely swollen, painful, warm joints.
6. Blood Test Results
- OA: Blood tests are typically normal. The diagnosis is clinical and radiological.
- RA: Elevated inflammatory markers (CRP, ESR). Positive Rheumatoid Factor (RF) in about 70–80% of patients. Positive anti-CCP antibodies (a more specific marker). Note: Some RA patients are "seronegative," with negative blood tests, but still have clinical RA.
7. X-Ray Appearance
- OA: Joint space narrowing (cartilage thinning), osteophytes (bone spurs), subchondral sclerosis (hardening of bone below cartilage). Asymmetric findings.
- RA: Joint space narrowing (from cartilage destruction), erosions at the joint margins (bone being destroyed), osteopenia (bone thinning around the joint from inflammation). Symmetric findings.
8. Who Treats It
- OA: Primarily managed by orthopedic surgeons for the joint involvement, in coordination with a pain management specialist or physiotherapist.
- RA: Primarily managed by a rheumatologist with disease-modifying medications. The orthopedic surgeon becomes involved when joint damage reaches the point where surgical reconstruction or replacement is needed.
How Is Each Diagnosed?
1. Diagnosing OA

An anatomical illustration comparing a normal bone structure to one affected by severe osteoporosis. On the left, the normal bone displays a dense and healthy structure, while on the right, the severe osteoporosis shows a porous and weakened bone.
Diagnosis of osteoarthritis is primarily clinical, based on the patient's symptoms, age, risk factors, and physical examination findings.
Key diagnostic elements:
- Age over 45 with joint pain.
- No morning stiffness or stiffness that resolves within 30 minutes.
- Crepitus (creaking/grinding) in the joint on movement.
- Activity-related pain that improves with rest.
Investigations:
- X-ray (weight-bearing): The standard imaging for OA. Shows joint space narrowing, osteophytes, and deformity. An X-ray that shows bone-on-bone contact in the knee, alongside appropriate symptoms, is the primary basis for surgical decision-making.
- MRI: Used selectively to assess cartilage, meniscus, and ligament status when X-ray findings don't fully explain symptoms.
- Blood tests: Ordered mainly to rule out RA and gout. In pure OA, inflammatory markers are normal or minimally elevated.
2. Diagnosing RA
RA diagnosis uses a combination of clinical criteria, blood tests, and imaging.
Key diagnostic elements (ACR/EULAR criteria):
- Symmetric joint swelling involving small joints (MCP, PIP joints of hands and feet).
- Morning stiffness lasting over 60 minutes.
- Elevated CRP or ESR.
- Positive RF or anti-CCP antibodies.
- Characteristic X-ray or ultrasound findings (erosions).
Investigations:
- Blood tests: RF, anti-CCP, CBC, CRP, ESR, the core panel.
- X-ray: Of hands and feet initially looking for erosions and periarticular osteopenia.
- Ultrasound: Increasingly used to detect early synovitis (joint lining inflammation) before X-ray changes appear.
- MRI: For complex cases or to assess early joint damage.
Treatment: Where The Paths Completely Diverge
1. Treating Osteoarthritis
OA management is staged by severity and is focused on managing symptoms, slowing progression, and preserving function for as long as possible.
Stage 1 - Conservative management:
- Weight loss (every kg lost reduces knee load by 4 kg)
- Low-impact exercise: swimming, cycling, walking
- Physiotherapy: quadriceps strengthening, gait training
- Proper footwear and assistive devices
- Heat and cold therapy for symptom relief
Stage 2 - Medications:
- Paracetamol and topical NSAIDs (first line)
- Oral NSAIDs (ibuprofen, etoricoxib) for moderate pain
- Supplements (glucosamine, chondroitin, evidence mixed but safe)
Stage 3 - Injections:
- Corticosteroid injections provide fast relief for 3–6 months
- Hyaluronic acid (viscosupplementation) - joint lubricant, 6–12 months of relief
- PRP (Platelet-Rich Plasma) - growing evidence for early-moderate OA
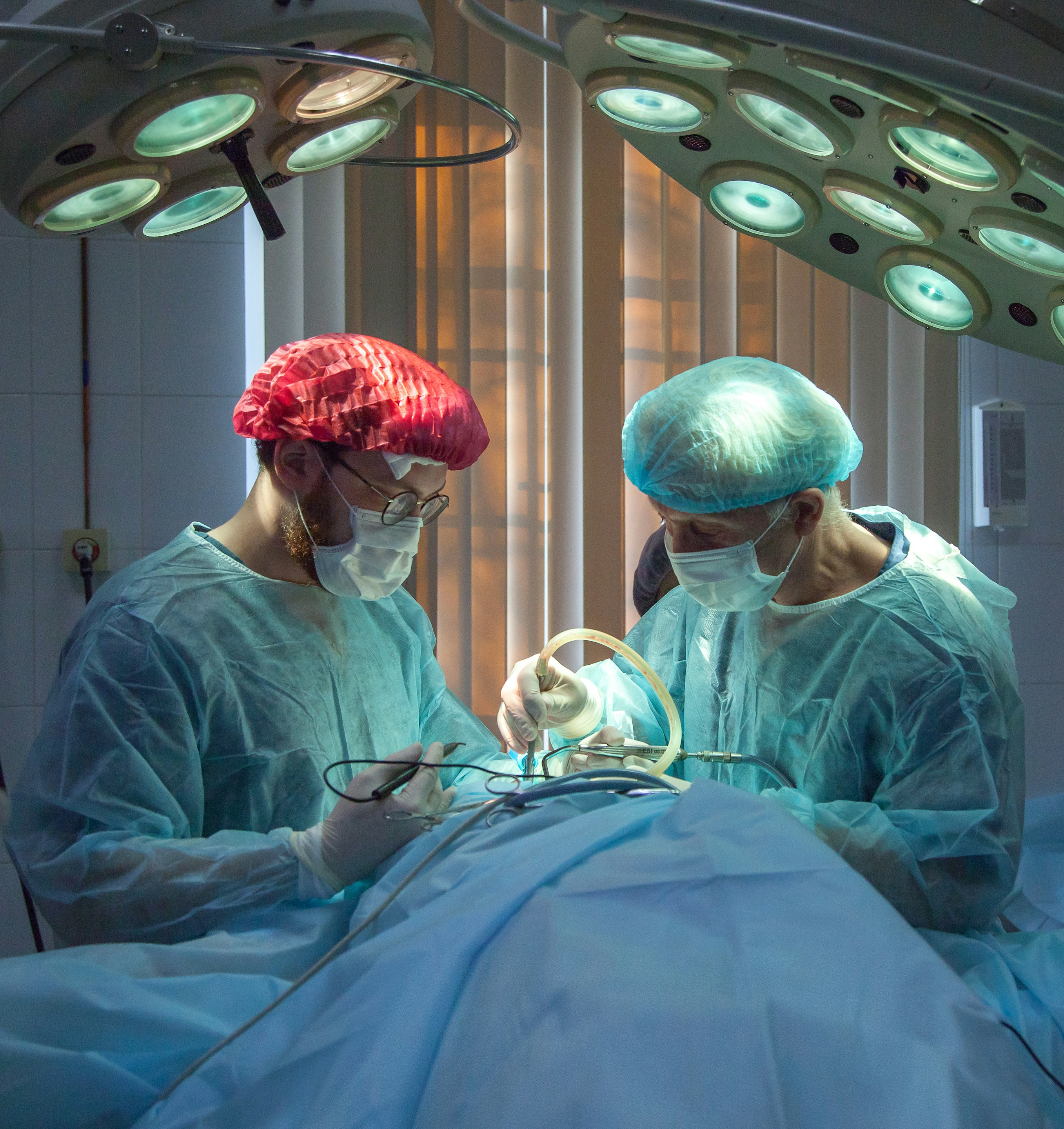
Stage 4 - Surgery:
- High Tibial Osteotomy (HTO) - realignment surgery for younger patients with isolated medial compartment OA
- Partial Knee Replacement - for isolated single-compartment OA
- Total Knee Replacement - for advanced, multi-compartment OA
Treating Rheumatoid Arthritis
RA treatment is fundamentally different; it targets the immune system, not the joint mechanics.
Disease-Modifying Anti-Rheumatic Drugs (DMARDs) - the backbone of RA treatment:
- Methotrexate - the most commonly used first-line DMARD. Reduces immune system activity and slows joint destruction. Requires regular blood monitoring.
- Hydroxychloroquine - often used in combination, particularly for milder RA
- Sulfasalazine - another DMARD used in combination therapy
- Leflunomide - an alternative to methotrexate in patients who cannot tolerate it
Biologics - for patients who don't respond adequately to DMARDs:
- TNF-inhibitors (adalimumab, etanercept, infliximab) - block the inflammatory cytokine TNF-alpha
- IL-6 inhibitors, JAK inhibitors, and other targeted therapies
Corticosteroids: Used to control acute flares, prednisone or prednisolone. Important for short-term symptom control, but long-term use has significant side effects and is avoided where possible.
The orthopedic role in RA:
When RA has destroyed joints to the point where function is significantly impaired, and medications no longer control the joint damage, surgical options include synovectomy (removing the inflamed joint lining), joint fusion, or joint replacement. RA patients can and do have knee and hip replacements, but the pre- and post-operative management requires coordination between the rheumatologist and the orthopedic surgeon.
Can You Have Both?
Yes. OA and RA can coexist in the same patient, particularly in older adults who already have underlying OA and then develop RA. When this happens, the management is more complex: the rheumatologist manages the autoimmune component while the orthopedic surgeon addresses the mechanical joint damage.
Orthopedic Care In Noida For Both Conditions
Dr. Mayank Chauhan, Senior Orthopedic Surgeon at Prakash Hospital, Sector 33, Noida, evaluates and manages patients with both osteoarthritis and rheumatoid arthritis. For OA patients, Dr. Chauhan provides the full spectrum of non-surgical and surgical management from physiotherapy guidance and injection therapy through to partial and total knee replacement.
For RA patients, the orthopedic role begins with a proper differential diagnosis confirming whether the joint condition is mechanical or inflammatory, and then coordinating with rheumatology for medical management. When RA patients reach the point where joint replacement is needed, Dr. Chauhan manages the surgical planning in coordination with their rheumatologist to ensure the best possible outcome.
Many patients in Noida and Greater Noida arrive at orthopedic consultations with a diagnosis of "arthritis" without clarity on which type. Getting that clarity is the first step because everything that follows depends on it. To book a consultation with Dr. Mayank Chauhan, call the number listed on the website.
The Bottom Line

3D illustration of a human bone with calcium molecules around it on a blue background.
Rheumatoid arthritis and osteoarthritis are not the same disease. They share joint pain as a symptom, but their causes, patterns, blood test profiles, X-ray appearances, and treatments are completely different. If you have joint pain and are not sure which type of arthritis you have or if you've been told you have "arthritis" without any specificity, a proper evaluation with appropriate blood tests and imaging will give you the clarity you need to pursue the right treatment.
Don't treat a problem you don't fully understand. Get the diagnosis right first. To consult Dr. Mayank Chauhan, Senior Orthopedic Surgeon in Noida, call the number listed on the website.