Osteochondral Lesions: What to Do When Cartilage Damage Worsens?

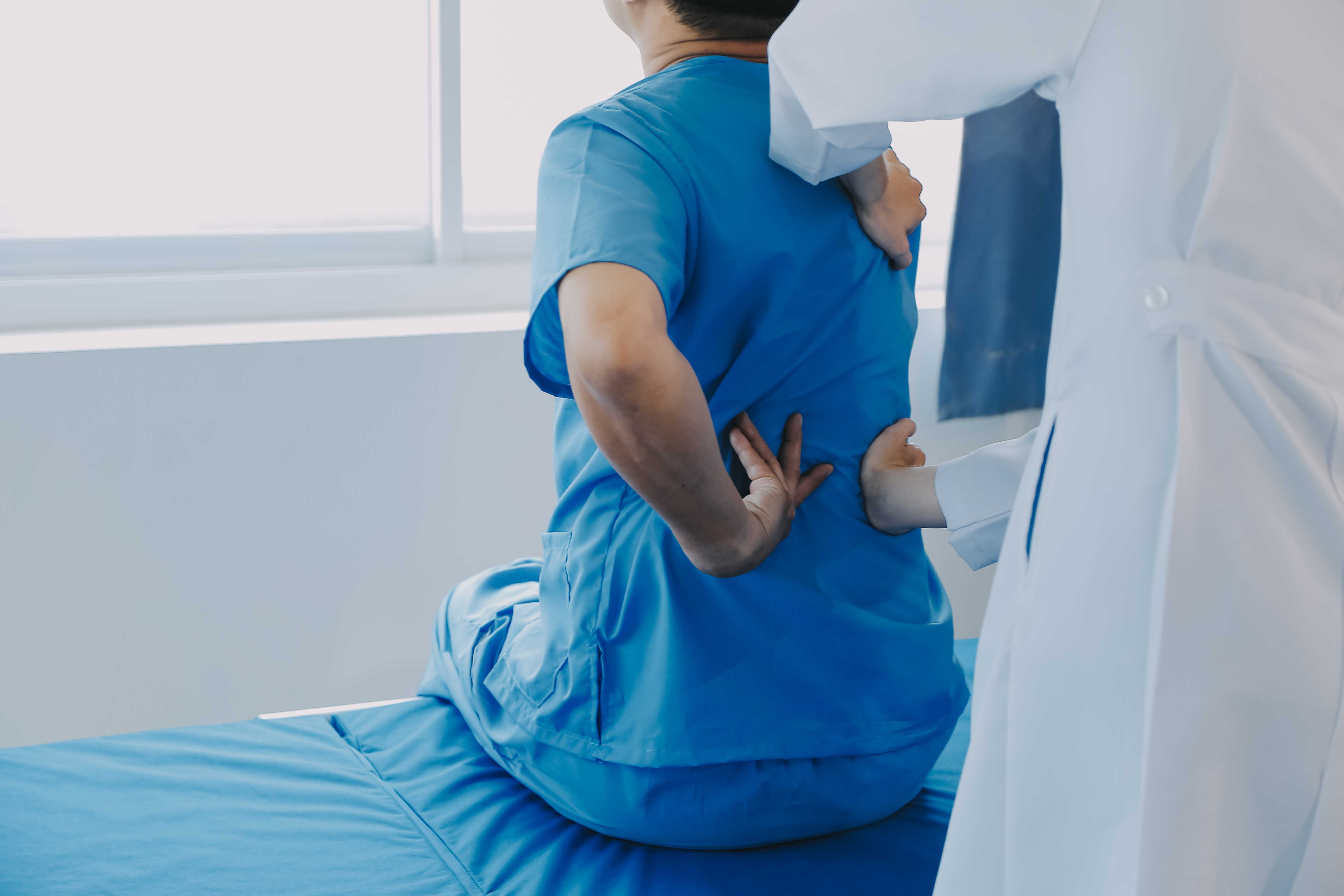
A man holds his knee in pain, with a red highlight indicating discomfort.
Most people don’t really think about cartilage until something goes wrong. It’s that smooth layer in the joints that keeps movement easy and pain-free. But when it starts getting damaged, things change quickly.
Osteochondral lesions happen when both the cartilage and the underlying bone are affected. This isn’t just about mild discomfort. It can lead to persistent pain, stiffness, swelling, and in some cases, difficulty even walking or performing everyday activities.
Athletes, active individuals, or even people with past injuries are more likely to experience it, but it can happen to anyone. The tricky part is that cartilage doesn’t heal easily on its own. Instead of ignoring the symptoms or relying only on temporary fixes, it’s important to understand what’s happening inside the joint and take the right steps early.
In this guide, let’s break down what osteochondral lesions are, why they worsen, and when it’s time to consult an orthopedic specialist for proper treatment and recovery.
What Are Osteochondral Lesions?
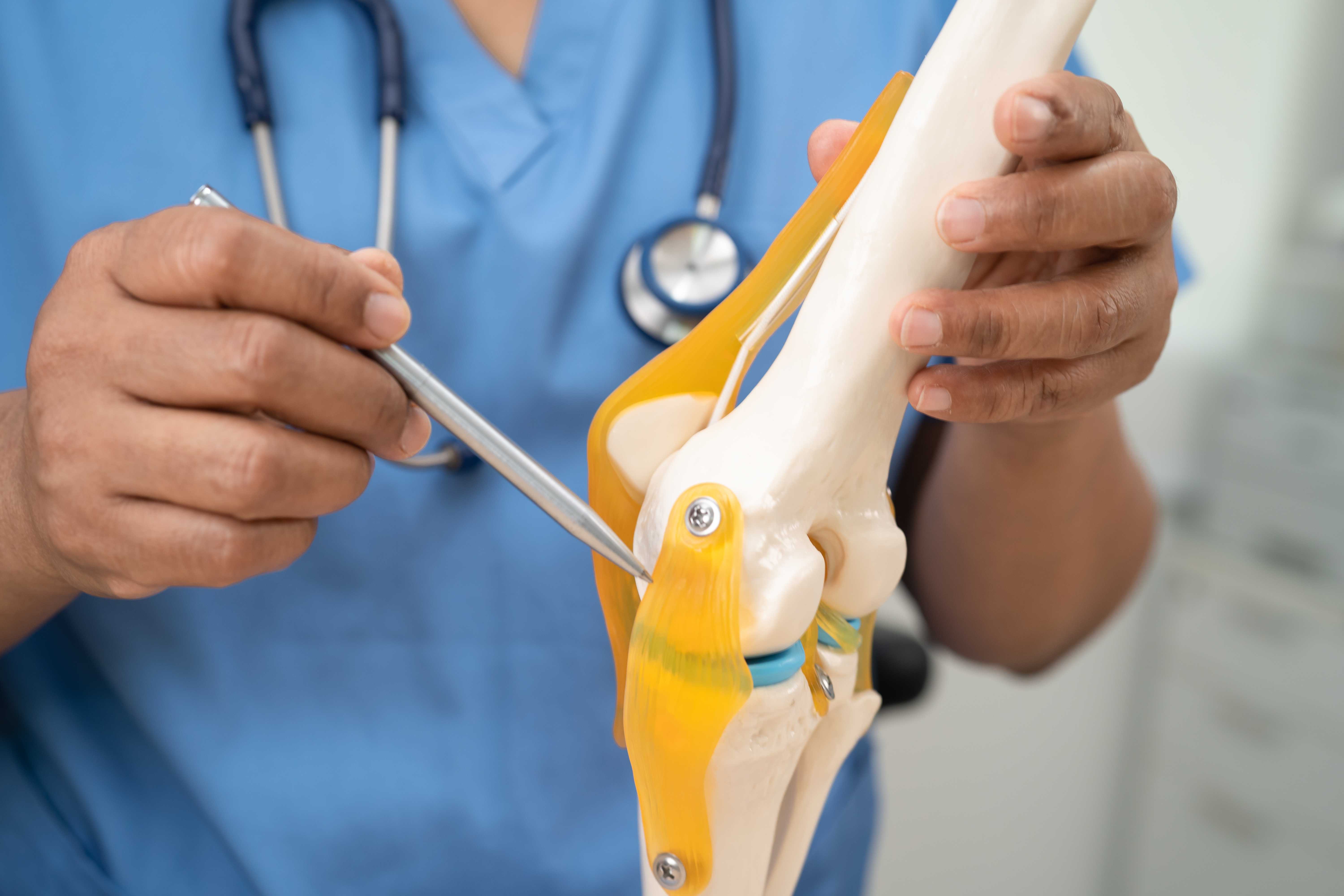
Osteochondral lesions refer to damage that affects both the cartilage and the bone beneath it within a joint. These lesions are most commonly seen in the knee, ankle, or elbow. Cartilage normally acts like a cushion, allowing smooth movement. When the joint is injured along with the bone, the joint loses its natural glide, leading to pain and restricted motion. In some cases, small fragments of cartilage or bone may even loosen and float inside the joint, making movement more uncomfortable.
Why Osteochondral Lesions Worsen?
These injuries don’t always stay the same. In many cases, they gradually get worse if not treated properly. Poor blood supply to cartilage slows down healing, making recovery difficult. Continued stress on the joint, especially through sports or heavy physical activity, can increase the damage. Over time, untreated lesions may lead to joint instability, chronic pain, and even early arthritis. That’s why early diagnosis and management are critical.
Causes Of Osteochondral Lesions
Osteochondral lesions don’t just appear suddenly; they usually develop due to specific underlying factors.
- Joint Injuries or Trauma - Sudden impact during sports or accidents can damage cartilage and bone.
- Repetitive Stress - Continuous strain on joints, especially in athletes, can lead to gradual wear and tear.
- Poor Blood Supply - Reduced blood flow affects the healing ability of the bone beneath the cartilage.
- Genetic Predisposition - Some individuals may naturally have weaker cartilage structures.
- Underlying Conditions - Disorders like osteochondritis dissecans can contribute to lesion formation.
Common Symptoms To Watch For
Osteochondral lesions can present in different ways depending on severity.
- Persistent joint pain - Pain that doesn’t go away with rest is often the first sign. It may worsen during activity.
- Swelling and inflammation - The affected joint may appear swollen, especially after movement or exertion.
- Limited range of motion - Stiffness or difficulty bending and straightening the joint is common.
- Clicking or locking sensation - Some people feel a catching or locking sensation due to loose fragments in the joint.
- Joint instability - The joint may feel weak or unstable, especially while walking or bearing weight.
Treatment Options For Osteochondral Lesions
Treatment depends on the size, location, and severity of the lesion, along with the patient’s age, activity level, and overall joint condition. The goal is not just to reduce pain, but to restore joint function and prevent long-term damage.
1. Rest And Activity Modification
Limiting high-impact activities like running, jumping, or heavy lifting helps reduce pressure on the affected joint. This allows the damaged cartilage and bone to recover without further strain.
2. Physiotherapy
A structured physiotherapy program helps strengthen the muscles around the joint, which improves stability and reduces load on the damaged area. It also focuses on restoring range of motion, correcting movement patterns, and preventing further injury.
3. Medications
Anti-inflammatory medications may be prescribed to manage pain and swelling. While they don’t heal the lesion, they make it easier for patients to stay active and participate in rehabilitation.
4. Bracing And Support

A healthcare professional examines a patient's knee, which is in a support brace.
Braces or supports help offload pressure from the affected joint and provide stability during movement. This is especially useful in weight-bearing joints like the knee or ankle.
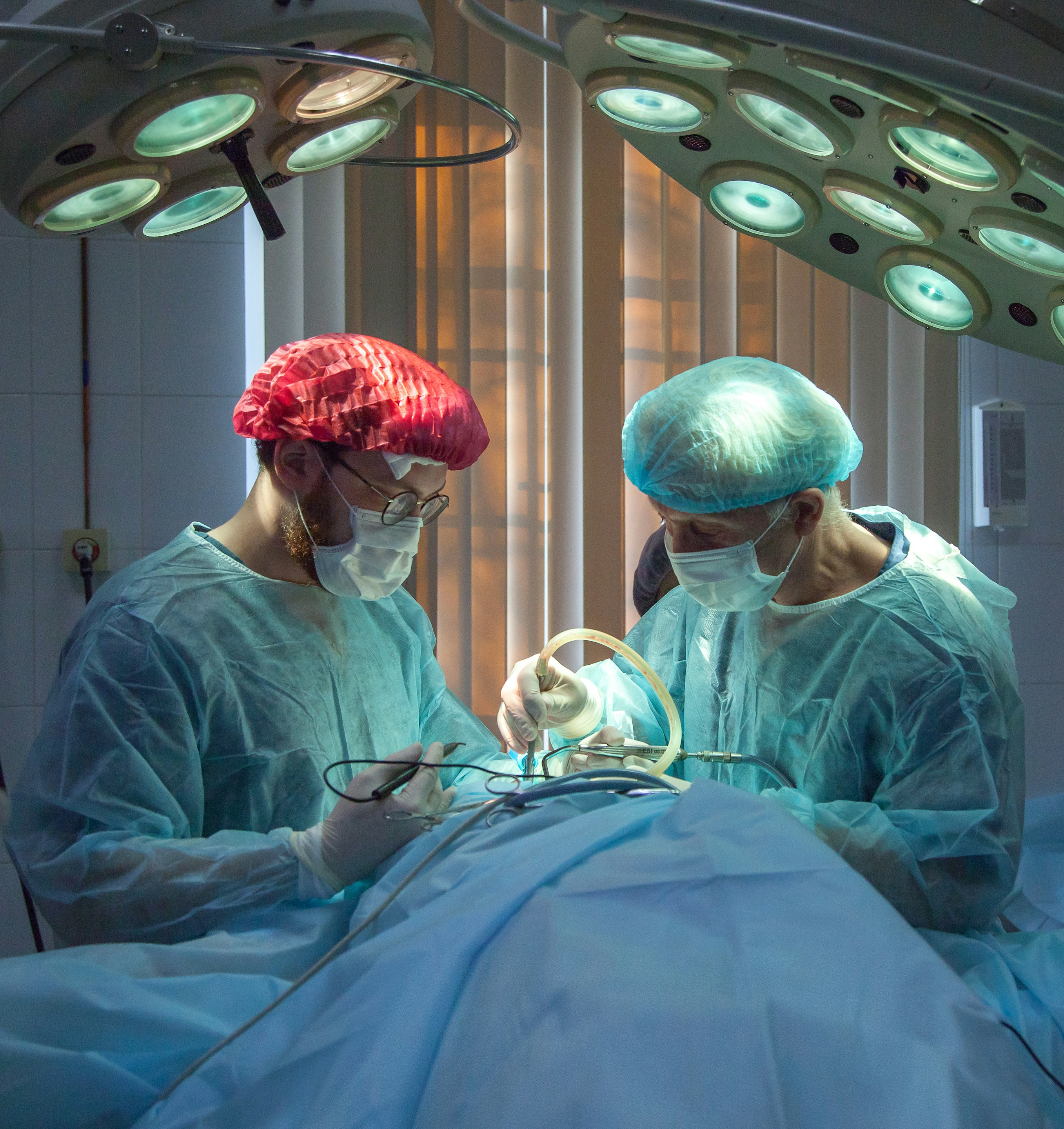
5. Arthroscopic Debridement
This minimally invasive procedure involves cleaning the joint by removing loose cartilage or bone fragments. It helps reduce pain, improve joint movement, and prevent further irritation.
6. Microfracture Surgery
In this technique, tiny holes are created in the underlying bone to stimulate the body’s natural healing response. This encourages the formation of new cartilage-like tissue, which helps cover the damaged area.
7. Osteochondral Grafting
Healthy cartilage and bone are transplanted either from another part of the patient’s joint or from a donor. This procedure is often used for larger defects and aims to restore the joint surface more effectively.
8. Autologous Chondrocyte Implantation (ACI)
A two-stage regenerative procedure where cartilage cells are first harvested, grown in a lab, and then implanted back into the damaged area. It is especially beneficial for younger, active individuals with larger cartilage defects.
9. Platelet-Rich Plasma (PRP) Therapy
PRP involves using a concentrated form of the patient’s own blood platelets, which are rich in growth factors. When injected into the affected joint, PRP helps reduce inflammation, promotes tissue healing, and may improve cartilage health over time.
10. Stem Cell Therapy
Stem cell therapy uses the body’s regenerative cells, usually derived from bone marrow or fat tissue, to repair damaged cartilage and bone. These cells have the potential to develop into cartilage-like tissue, supporting healing in osteochondral lesions, especially in early to moderate cases.
To ensure the most effective treatment plan is followed, consulting Dr. Mayank Chauhan in Noida allows patients to receive a detailed evaluation and personalized care. With the right combination of treatment and rehabilitation, it becomes possible to reduce pain, restore joint function, and return to an active lifestyle safely.
Complications If Left Untreated
Ignoring osteochondral lesions can lead to more serious joint problems over time.
- Chronic Joint Pain that becomes difficult to manage
- Progressive Cartilage Damage leading to joint degeneration
- Joint Locking Or Instability affecting movement
- Early Onset Osteoarthritis due to continuous wear
Timely intervention can help avoid these long-term complications.
Key Benefits Of Early Treatment

A woman in a gray coat checks her phone while walking in a park.
Addressing osteochondral lesions early can make a significant difference in recovery outcomes.
- Prevents Further Joint Damage - Early care stops the lesion from worsening and protects surrounding structures.
- Reduces Pain And Discomfort - Targeted treatment helps relieve pain and improve overall comfort.
- Restores Mobility - Improves joint function and allows smoother movement.
- Avoids Complex Surgery - Timely intervention may reduce the need for advanced surgical procedures.
- Improves Quality Of Life - Helps patients return to daily activities and physical routines without limitations.
When To See An Orthopedic Specialist
Sometimes, the body gives clear signals that shouldn’t be ignored.
- If discomfort continues despite rest, it needs medical attention.
- Struggling with basic activities is a strong indicator of joint issues.
- Frequent swelling suggests underlying damage that needs evaluation.
- Joints are locking or catching, which means loose cartilage or bone fragments inside the joint.
- Past injuries increase the risk of developing osteochondral lesions.
Final Thoughts
Osteochondral lesions are more than just a minor joint problem. If left untreated, they can gradually worsen and impact overall mobility and quality of life. Recognizing the symptoms early and taking the right steps can prevent long-term complications.
For accurate diagnosis and advanced treatment options, consulting Dr. Mayank Chauhan in Noida ensures patients receive expert care tailored to their condition. With the right approach, it becomes possible to reduce pain, restore movement, and get back to an active lifestyle with confidence.
Frequently Asked Questions (FAQs)
1. What is an osteochondral lesion?
An osteochondral lesion is damage to both the cartilage and underlying bone within a joint, commonly affecting the knee or ankle.
2. Can osteochondral lesions heal without surgery?
Mild osteochondral lesions may heal with rest, physiotherapy, and activity modification, but severe cases often require surgical treatment.
3. What causes osteochondral lesions?
They are usually caused by joint injuries, repetitive stress, reduced blood supply, or conditions like osteochondritis dissecans.
4. How long does it take to recover from an osteochondral lesion?
Recovery can take a few weeks to several months, depending on severity, treatment method, and adherence to rehabilitation.