Knee Replacement Recovery - Week-By-Week Guide (What To Really Expect)

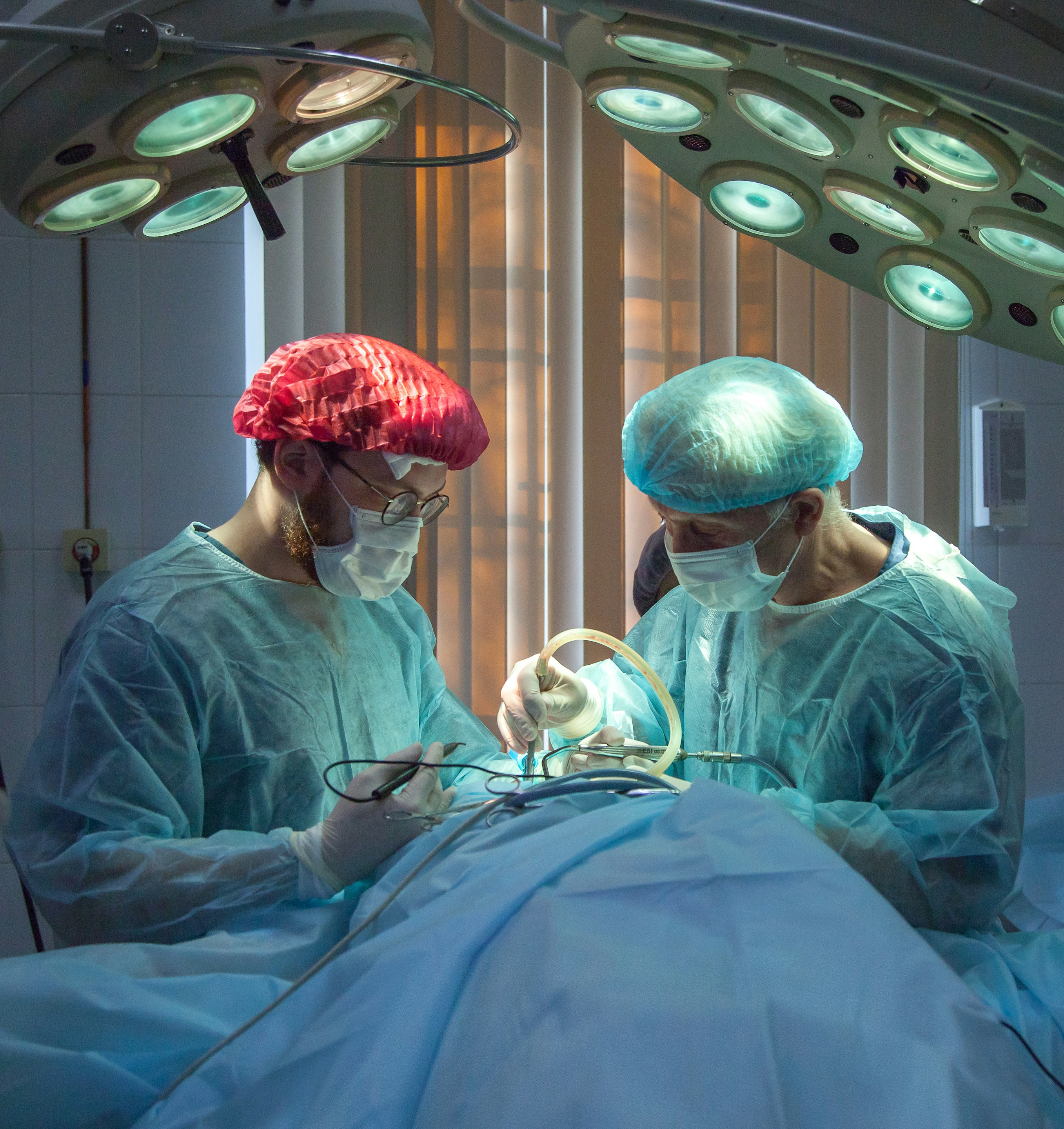
An operation that is taking place in a hospital operating room with two surgeons in surgical gear working on a person's knee. The person's body is not shown below the sterile drapes but is implied as under them.
Most patients going into knee replacement surgery have heard two things: "You'll be walking in a day or two" and "Full recovery takes six months." Both of these are true. But neither one tells you what actually happens in the weeks between those two points, and that gap is where most patients feel lost, frustrated, or unprepared.
This guide fills that gap. It's a realistic, week-by-week breakdown of knee replacement recovery - what you'll experience, what's normal, what's worth calling your surgeon about, and what you can do to recover as well as possible. It's specifically written for patients in Noida and Greater Noida preparing for surgery with Dr. Mayank Chauhan at Prakash Hospital, Sector 33, Noida, but the timeline applies to any total or partial knee replacement patient.
Before We Start: What Affects How You Recover
Recovery after knee replacement is not the same for every patient. Several factors significantly influence how quickly and completely you recover:
- Age - Younger patients generally have stronger healing responses and more energy for physiotherapy
- Pre-operative fitness - Patients who were more mobile before surgery tend to regain function faster
- Body weight - Excess weight adds stress to the new joint and can slow recovery
- Consistency with physiotherapy - This is the single biggest variable within your control
- Mental attitude - Patients who stay motivated and engaged with their recovery plan do measurably better
- Chronic conditions - Diabetes, heart disease, and other conditions can slow healing and need to be well-managed
What this means in practice: don't compare your progress to a friend who had the same surgery. Compare your progress week to week against your own baseline.
The Day Of Surgery
You check in to the hospital, change into a hospital gown, and go through final pre-operative checks, like blood pressure, blood sugar, and a brief review of your medications. An IV line goes into your arm. A catheter may be placed to manage urination while you're immobile in the immediate post-op period.
The surgery itself takes approximately 90 minutes to 2 hours. Under spinal or general anaesthesia, the surgeon removes the damaged joint surfaces, precisely shapes the bone ends, and fits the prosthetic components. The wound is closed in layers and covered with a sterile dressing.
When you wake up in the recovery area, your knee will be wrapped, slightly elevated, and surrounded by cold therapy packs to manage swelling. Pain is managed with intravenous medication initially. Most patients describe the immediate post-op sensation as pressure and heaviness rather than sharp pain.
Day 1–3: Hospital Phase
What happens: Within 12 to 24 hours of surgery, the physiotherapy team will come to see you. This is not optional, and not premature; early movement is one of the most important factors in preventing blood clots and joint stiffness.
You'll sit up, move your legs, and, with the physiotherapist's support, stand at the bedside. Many patients take their first assisted steps with a walker on the first day after surgery. This typically feels both more manageable than expected and more exhausting than expected.
Exercises during this phase:
- Ankle pumps - Moving the foot up and down to encourage blood circulation
- Quad sets - Tightening the thigh muscles while the leg is flat
- Assisted knee bending - Gently bending the new knee with support
What's normal: Significant swelling. Bruising around the knee and sometimes extending down the calf or shin. Moderate pain managed well with prescribed medication. Surgery is a physical stress on the body, and recovery uses energy.
Target by discharge: Walking short distances with a walker. Knee bending of approximately 60–70 degrees. Ability to manage basic daily activities with assistance.
Hospital discharge typically happens between day 3 and day 5, depending on your general health, how well the knee is moving, and your home support situation.
Week 1: Home - The Hardest Week
This is the week most patients find toughest. You're home, the hospital structure is gone, and the reality of what recovery actually involves becomes clear. What to focus on:
- Walking with a walker inside the house, and aim for short distances every 1–2 hours rather than long exhausting walks.
- Doing your physiotherapy exercises 2–3 times a day as prescribed.
- Keeping the leg elevated when sitting or resting, as this significantly reduces swelling.
- Applying ice packs for 15–20 minutes at a time, several times a day.
- Taking prescribed pain medication on schedule; don't wait until pain becomes severe before taking it.
Sleep: Most patients struggle with sleeping in the first week. The knee is uncomfortable, and finding the right position takes time. Sleeping on your back with a pillow under the calf (not under the knee, which can cause flexion contracture) is typically the most comfortable.
Wound care: Keep the dressing clean and dry. Don't get the wound wet until cleared by your surgeon. Watch for signs of infection: increasing redness, warmth, discharge, or fever above 38°C.
What's normal: Significant swelling is normal, and it will not look like your other knee for several weeks. Bruising may spread. Clicking or crackling sounds in the new knee are common and not cause for alarm. Emotional ups and downs, frustration, even brief depression are more common than patients expect, and they pass.
Target by end of week 1: Knee bending of 70–90 degrees. Walking within the house with a walker. Managing stairs with support if needed.
Week 2: Small Milestones Start To Appear
Things typically start to feel more manageable in week two. Pain levels come down. Sleep improves slightly. Most patients start to feel like recovery is actually happening. Stitches or staples are usually removed around day 10–14. This is typically an outpatient appointment with your surgeon for a wound check and progress assessment.
Physiotherapy steps up: Exercises become more involved. Straight leg raises, heel slides, and assisted knee bending push the range of motion toward 90 degrees and beyond.
Walking: Distances within the house increase. Some patients begin short walks outside, like to a car, to the building gate with the walker.
Target by end of week 2: Knee bending of 90 degrees. Walking with a walker with more confidence. Reduced pain medication dependency compared to week one.
Week 3–4: Transition To A Walking Stick
For many patients, this is the phase when they feel genuine progress for the first time. The walker starts to feel unnecessary for some movements, and the transition to a cane or walking stick often begins around week 3 or 4, guided by your physiotherapist, not by your own eagerness. Physiotherapy additions:
- Resistance exercises using therabands or light weights.
- Mini squats against the wall.
- Balance and proprioception exercises.
- Stair practice; step up with the good leg leading, step down with the operated leg leading (up with the good, down with the bad).
Driving: Most patients are advised not to drive for at least 6 weeks after surgery on the operated leg. This is both a safety concern and a legal one.
Going out: Short trips outside the home, like to a clinic appointment, a short walk in the neighbourhood become possible for most patients. Plan them for your better time of day (morning for most patients) and don't overdo it.
Target by end of week 4: Knee bending of 100–110 degrees. Managing most indoor activities without a walker. Stairs possible with a railing.
Week 5–6: Approaching Independence

A nurse is helping a patient with a knee brace and a clutch with walking in a physiotherapy room.
This is often when patients start feeling like themselves again. Pain is much reduced. Walking distances are significantly longer. Most daily household activities, like cooking at a counter, going to the bathroom independently, and sitting comfortably, are manageable.
Physiotherapy continues: This is not the phase to ease off, even though it's tempting to think you're done. Muscle strength is still rebuilding, and stopping physiotherapy at 6 weeks typically leads to a plateau that limits outcomes.
Follow-up appointment: Most surgeons schedule a formal follow-up around 6 weeks. This includes a review of your X-ray, assessment of range of motion, and discussion of progress toward full recovery goals.
Driving (for the operated leg): Often permitted around the 6-week mark, depending on your surgeon's assessment and whether you can perform an emergency stop safely.
Target by end of week 6: Knee bending of 110–120 degrees. Walking medium distances without a stick. Driving approved (if the operated leg is involved). Return to a desk job possible for many patients.
Months 2–3: Building Strength And Endurance
By the end of month two, most patients are walking without any support and managing most daily activities comfortably. But the knee is not yet fully recovered, and this is where some patients make the mistake of stopping physiotherapy entirely. The muscles around the knee, particularly the quadriceps and hamstrings, take longer to regain full strength than the joint takes to heal. Continuing targeted strengthening exercises through months 2 and 3 is what separates a very good outcome from a merely decent one.
Activities that become possible:
- Swimming (once the wound is fully healed, usually from 6–8 weeks)
- Stationary cycling (low resistance, seat positioned high to avoid deep bending initially)
- Short shopping trips
- Light gardening
- Going to a temple or place of worship (with appropriate footwear and avoiding prolonged deep bending)
Activities still to avoid:
- Running and high-impact sports
- Carrying heavy loads
- Prolonged standing without a break
- Squatting deeply until cleared by your surgeon
Months 3–6: Full Recovery
This is the phase where most patients say "I finally feel like my knee is normal again." Pain is minimal or absent. Walking is comfortable. Sleep is uninterrupted. Most activities of daily life, and many recreational ones, are possible.
The knee continues to improve in this phase as strength and endurance keep building, and the sense of the implant feeling like "your own knee" grows over time. Some patients describe a fully natural-feeling knee by month 4; others reach that point closer to month 6. Both are normal.
At 6 months: A final assessment with your surgeon confirms that recovery is complete. Low-impact activities like swimming, cycling, yoga, and light hiking are typically encouraged long-term to maintain muscle strength and joint health.
Warning Signs - When To Call Your Surgeon
Most discomfort during recovery is normal. But some symptoms require prompt attention. Call your surgeon if you experience:
- Fever above 38°C, as it can indicate infection.
- Increased redness, warmth, or discharge from the wound.
- Sudden severe increase in knee pain, especially after initial improvement.
- Significant calf swelling or tenderness; possible blood clot (DVT), which requires same-day evaluation.
- Shortness of breath or chest pain; possible pulmonary embolism, a medical emergency.
- The knee appears to lock or give way; possible implant complication.
Practical Tips From Patients Who've Done It

In a clinic, a female doctor is doing physiotherapy on the knee of a male patient who is lying down and looks relaxed.
- Set up your home before surgery - Move a bed to the ground floor if needed. Get a raised toilet seat. Remove loose rugs. Keep frequently used items at waist height so you're not bending or reaching. Have a stable chair with armrests in the room where you'll spend the most time.
- Have someone with you for the first two weeks - Getting in and out of bed, going to the bathroom, managing medications; all of this is much harder than it sounds in those early days.
- Do your physiotherapy even when you don't feel like it - Especially when you don't feel like it. The patients who recover fastest are the ones who do their exercises consistently every single day.
- Don't use the good knee to compensate too much - It's natural to favour the operated leg, but putting excessive load on the other knee for extended periods causes its own problems.
- Be patient with the swelling - Knee swelling after replacement takes weeks to months to fully resolve. The knee will look swollen for longer than it feels painful. This is normal.
The Bottom Line
Knee replacement recovery is not complicated, but it requires consistency, patience, and realistic expectations. The patients who do best are not necessarily the youngest or the fittest. They're the ones who commit to their physiotherapy, follow their surgeon's guidance, and don't compare their timeline to anyone else's.
If you're preparing for knee replacement surgery in Noida or Greater Noida, or if you have questions about what recovery involves for your specific situation, book a consultation with Dr. Mayank Chauhan at Prakash Hospital, Sector 33, Noida. To book your appointment, call the number listed on the website.