Joint Pain Treatment in Noida: Causes, Diagnosis and When to See an Orthopedic Surgeon

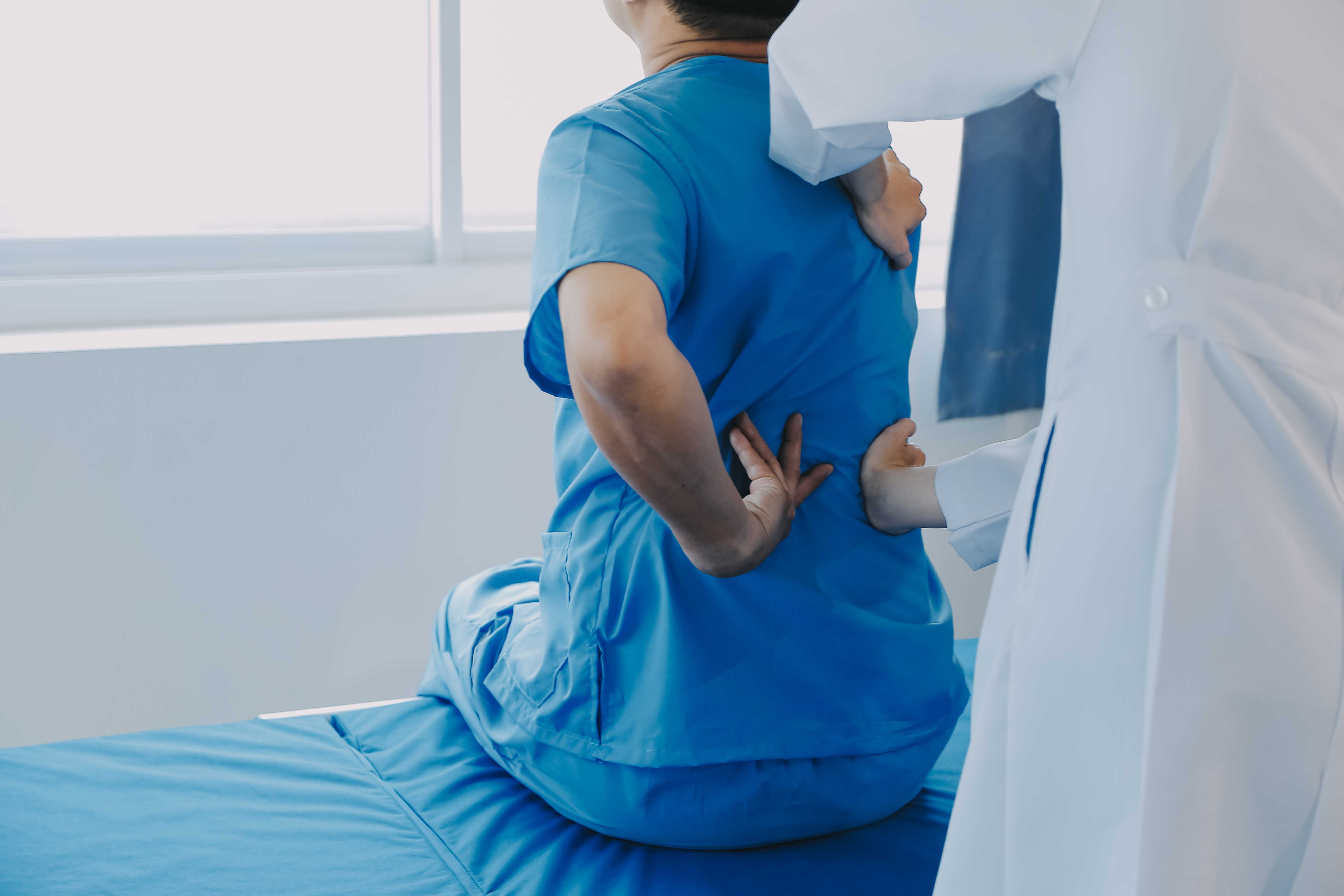
An orthopedic specialist assessing knee joint movement to identify the cause of persistent pain.
Joint pain is one of the most common reasons people visit a doctor in India. It affects people of every age — from 25-year-old software engineers with early disc problems showing up as knee strain, to 70-year-old grandparents with advanced arthritis who've been managing pain for decades. And yet, "joint pain" is so broad a term that it tells you almost nothing about what's actually wrong.
That's the frustration most patients in Noida describe. The pain is there. The X-ray gets done. The report says "mild degenerative changes" or "soft tissue swelling." The doctor prescribes a painkiller and physiotherapy. But three months later, the pain is still there — or it's moved to a different joint, or it's woken you up at 2 AM two nights in a row.
The reason this keeps happening is that joint pain has dozens of possible causes, and many of them look similar on the surface while requiring completely different treatment. Getting to the right diagnosis is the only way to get to the right treatment.
This guide covers the most common causes of joint pain seen by orthopedic specialists in Noida, the warning signs that should prompt you to seek evaluation sooner rather than later, and what a proper diagnostic and treatment process actually looks like.
What Causes Joint Pain?
A joint is formed anywhere two bones meet — surrounded by cartilage (the cushioning surface), synovial fluid (the lubricant), ligaments (the stabilisers), tendons (which attach muscles to bone), and the joint capsule (the outer wrapper). Pain can originate from any of these structures.
Here are the most common underlying causes
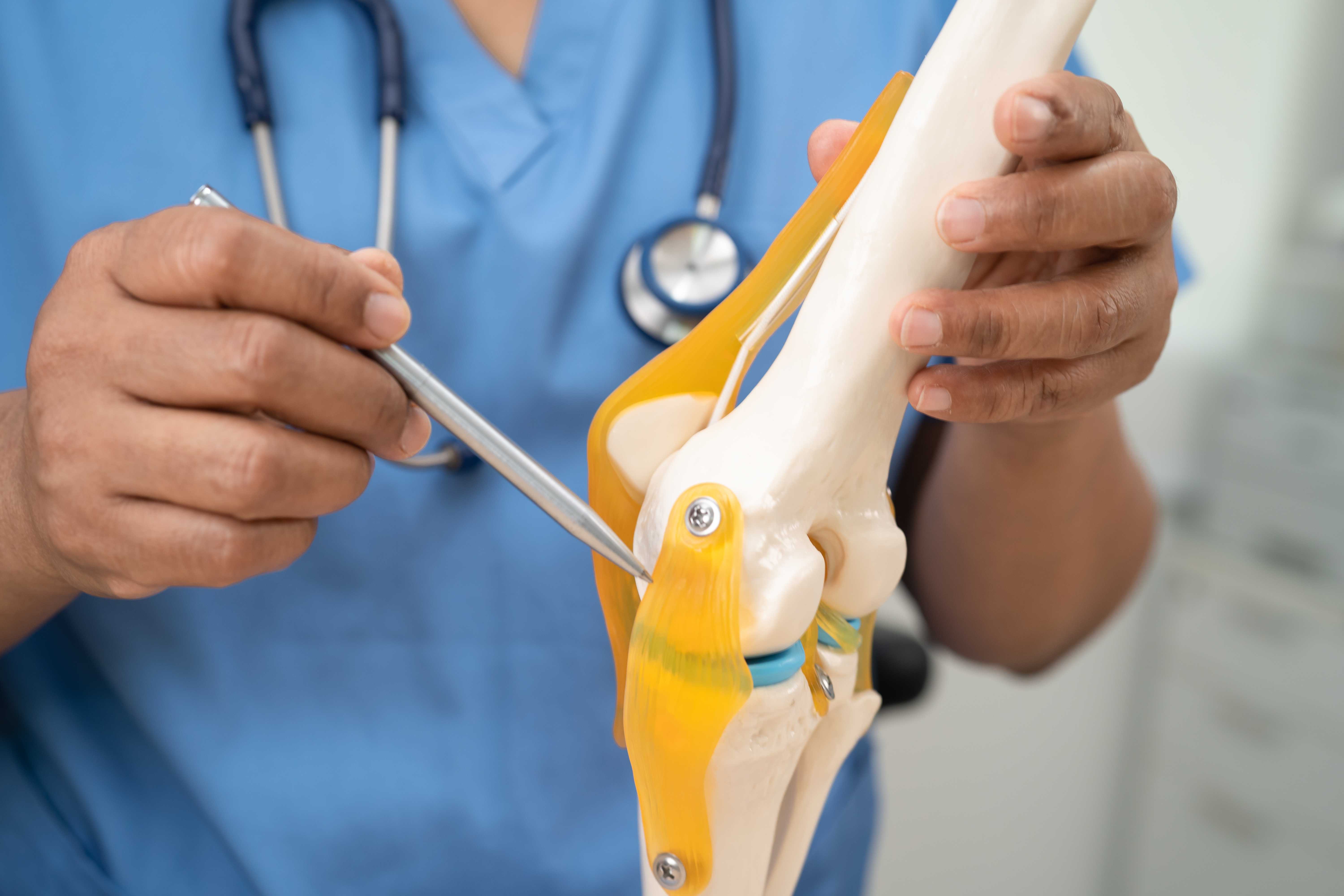
1. Osteoarthritis — Wear-and-Tear of the Joint
The most frequent cause of chronic joint pain in adults over 45 in Noida. Osteoarthritis (OA) happens when the cartilage protecting the joint surfaces wears down over time. With less cushioning, the bones begin to rub against each other, causing pain, stiffness, and swelling.
OA most commonly affects the knee, hip, spine, and hands. The pain is typically worse after prolonged activity and eases with rest. Morning stiffness is common but resolves within 30 minutes.
2. Rheumatoid Arthritis — When the Immune System Attacks the Joints
Rheumatoid arthritis (RA) is an autoimmune condition — the immune system mistakenly attacks the joint lining. It causes joint inflammation that's often symmetrical (affecting both knees, both hands, or both ankles at the same time). Morning stiffness lasting more than an hour is a hallmark. RA is more common in women and can start at any age, including in young adults.
Unlike OA, RA is a systemic disease — it can also affect the lungs, heart, and eyes. Blood tests (RF and anti-CCP antibodies) help confirm the diagnosis.
3. Gout — Uric Acid Crystals in the Joint
Gout causes sudden, intense joint pain — often in the big toe, but also in the ankle, knee, or wrist. The joint becomes red, hot, and extremely tender. Attacks are often triggered by alcohol, certain foods (red meat, organ meats, shellfish), or dehydration.
Gout is caused by elevated uric acid in the blood. It's diagnosed by testing uric acid levels and, definitively, by identifying crystals in joint fluid analysis.
4. Bursitis — Inflammation of the Fluid Sacs
Bursae are small fluid-filled sacs that cushion joints and reduce friction. When they become inflamed — due to repetitive movement, pressure, or infection — they cause localised pain and swelling. Bursitis is common in the knee (prepatellar bursitis, or "housemaid's knee"), shoulder, and hip.
5. Tendinitis — Inflamed Tendons
The tendons that attach muscles to bone around a joint can become inflamed through overuse or sudden strain. Patellar tendinitis (knee), Achilles tendinitis (heel), and lateral epicondylitis (tennis elbow) are common presentations.
6. Ligament Injuries
Ligament sprains — from sports injuries, falls, or sudden twisting movements — cause joint pain, swelling, and instability. The knee's ACL (anterior cruciate ligament) and ankle ligaments are among the most commonly injured. These don't always require surgery, but they do require proper evaluation.
7. Post-Viral Arthritis — After Chikungunya, Dengue, or COVID
Joint pain following viral infections is extremely common in Delhi NCR. Chikungunya in particular is notorious for causing severe, multi-joint pain that can persist for months — sometimes called post-chikungunya arthritis. COVID-19 has also been associated with joint pain as a post-infection symptom.
8. Psoriatic Arthritis
An inflammatory arthritis that occurs in people with psoriasis (a skin condition causing scaly patches). It can affect any joint and may cause "sausage digits" — swelling of entire fingers or toes. It's frequently under-diagnosed because the skin symptoms may be subtle.
9. Joint Pain from Vitamin D and Calcium Deficiency
This is extremely common in Noida and Delhi NCR. Vitamin D deficiency (in a city that ironically gets substantial sunshine) is widespread because most people spend their working hours indoors. Vitamin D deficiency causes bone and muscle pain that mimics joint pain, along with fatigue and weakness. A simple blood test (25-OH Vitamin D) confirms it.
10. Referred Pain from the Spine
Not all "joint" pain originates in the joint. Pain felt in the knee can actually originate from a problem in the hip. Pain felt in the hip can come from the lumbar spine. A slip disc in the lower back almost always causes pain that travels through the buttock and down the leg — which patients often describe as "knee pain" or "leg joint pain."
This is why a proper physical examination matters so much. The location of the pain is not always where the problem is.
Warning Signs That Need Urgent Evaluation
Most joint pain can be evaluated in a scheduled clinic appointment. But some symptoms require prompt attention.
See a specialist urgently if you have:
- Joint pain with fever and chills — this can indicate septic arthritis (infection inside the joint), which is a medical emergency that can destroy the joint permanently if not treated within hours to days
- A hot, severely swollen joint that appeared suddenly — especially in someone with a history of gout or who has been on steroids
- Joint pain following significant trauma (a fall, car accident, or sports injury) with immediate swelling and inability to bear weight
- Weakness, numbness, or tingling accompanying joint pain — suggests nerve involvement
- Joint pain with skin rashes, eye inflammation, or mouth ulcers — could indicate a systemic autoimmune condition
- Unexplained weight loss with joint pain — needs investigation to rule out malignancy
Diagnosing Joint Pain — What a Proper Evaluation Looks Like
The problem with treating joint pain effectively is that an accurate diagnosis is harder to get than most patients expect.
1. History
A detailed history is the foundation. How long has the pain been present? Which joint is affected? Is it both sides or one side? Is the pain worse in the morning or evening? Does it improve with movement or worsen with it? Does it radiate anywhere? Are there any other symptoms? Have you had recent infections?
2. Physical Examination
An experienced orthopedic surgeon uses physical examination to narrow down the cause significantly. Range of motion, joint line tenderness, swelling, muscle strength, ligament stability tests, and neurological assessment (sensation, reflexes) all contribute to the clinical picture.
3. Imaging
X-ray: The first-line investigation for most joint pain. Shows bone changes, joint space narrowing, fractures, and deformities. Normal X-rays don't rule out joint problems — cartilage and soft tissue damage don't show on X-ray.

An X-ray of the knee joint is taken and kept against a white background.
MRI: The most informative investigation for soft tissue problems — ligament tears, cartilage damage, meniscus tears, disc herniation, tendon injuries. It's more expensive and not always necessary, but for complex or undiagnosed joint pain, it's often essential.
Ultrasound: Useful for assessing fluid in the joint, bursitis, tendon problems, and guiding injections.
4. Blood Tests
For suspected inflammatory or autoimmune arthritis:
- CBC (Complete Blood Count)
- ESR and CRP (inflammatory markers)
- Rheumatoid Factor and anti-CCP (for RA)
- Serum uric acid (for gout)
- ANA (anti-nuclear antibody) for lupus
For suspected nutritional causes:
- Serum Vitamin D (25-OH)
- Calcium, Phosphorus
- Thyroid function (hypothyroid can cause joint pain)
Joint Pain Treatment — A Staged Approach
Treatment is matched to the diagnosis, severity, and the patient's individual circumstances.
1. Conservative Measures
RICE protocol for acute joint pain: Rest, Ice, Compression, Elevation — for the first 48 hours after an acute injury or flare.
Physical therapy: Strengthening the muscles around a joint protects it from further damage. A good physiotherapist is worth their weight in gold for most joint conditions.
Weight management: For lower-limb joints (knee, hip, ankle), every kilogram lost reduces load significantly. This is not advice to dismiss lightly — it's one of the most effective non-surgical interventions available.
Activity modification: This doesn't mean stopping all activity. It means choosing lower-impact activities (swimming, cycling) over high-impact ones (running, jumping) when joints are inflamed.
2. Medications
- NSAIDs (ibuprofen, diclofenac, etoricoxib) — for pain and inflammation. Short courses are effective and safe.
- Topical agents — diclofenac gel applied locally can provide relief with fewer systemic effects.
- DMARDs — for rheumatoid arthritis specifically. Methotrexate, hydroxychloroquine, sulfasalazine.
- Colchicine and allopurinol — for gout (acute treatment and long-term uric acid lowering respectively).
- Vitamin D supplementation — for confirmed deficiency.
3. Injections
- Corticosteroid injections — fast, effective relief for inflammatory joint pain and bursitis. Typically effective for 3–6 months.
- Hyaluronic acid — a joint lubricant injected into arthritic joints, particularly the knee. Provides sustained relief in patients with moderate OA.
- PRP (Platelet-Rich Plasma) — growing in popularity in Noida and Delhi NCR for knee OA and tendon problems. Uses the patient's own blood-derived growth factors to reduce inflammation and promote tissue repair.
4. Surgical Options
When conservative and interventional treatments have been adequately tried without sufficient improvement:
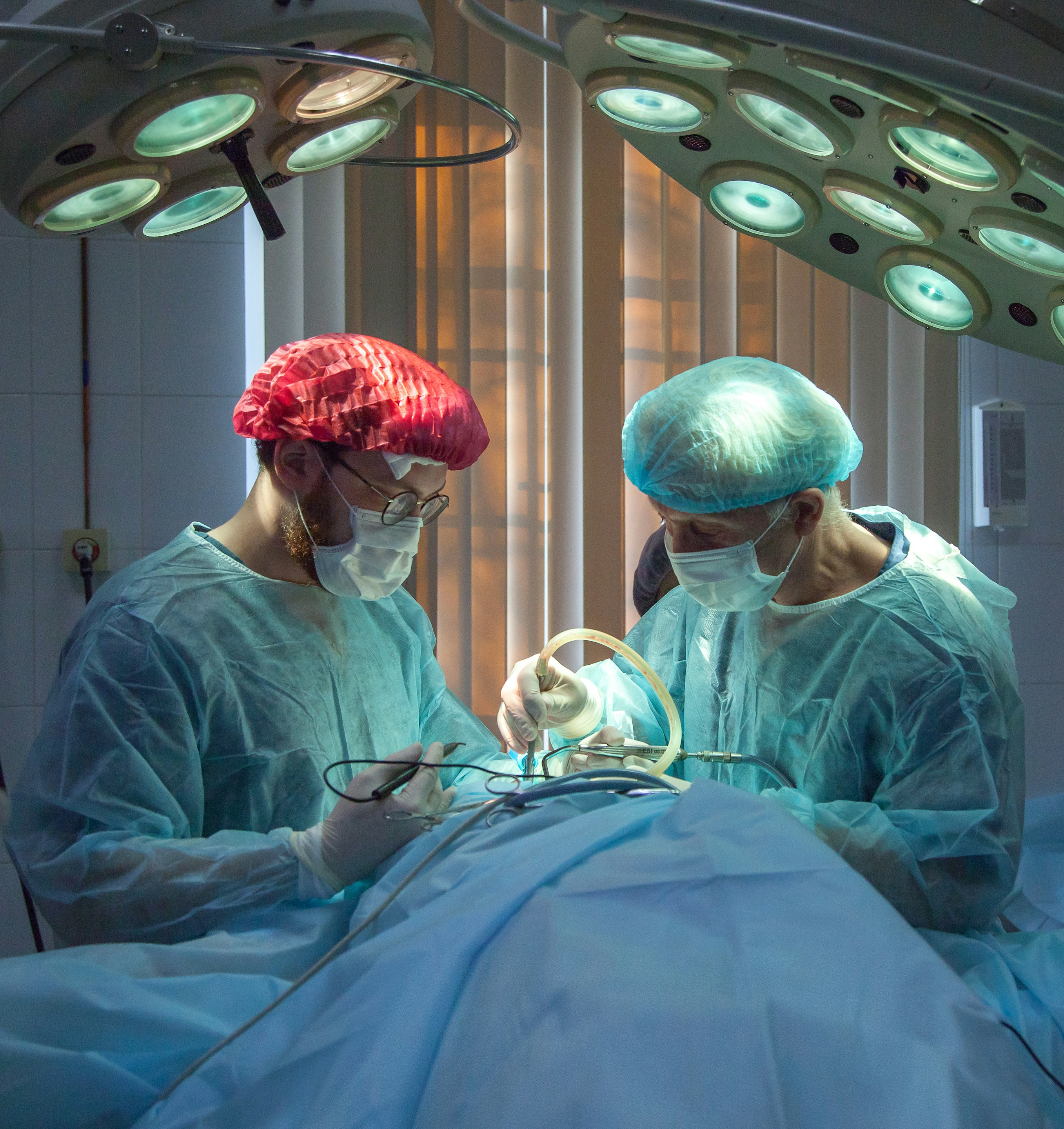
- Arthroscopy — for ligament repair, meniscus surgery, cartilage procedures
- Partial or Total Joint Replacement — for end-stage arthritis of the knee or hip
- Microdiscectomy or Spinal Surgery — when joint pain is actually referred pain from a spinal problem

A team of surgeons is operating on the knee of a patient lying on the bed through an arthroscopy procedure in the operating room.
Joint Pain Specialist in Noida — Why Choosing Right Matters
The most common mistake patients make with joint pain in Noida is bouncing between general practitioners, homeopaths, physiotherapists, and ortho clinics without anyone ever sitting down to do a thorough evaluation and establish a proper diagnosis.
Joint pain is complex. The causes range from the straightforward to the systemic. And the treatments range from a simple supplement to a major operation. Getting that diagnostic step right — the physical examination, the right blood tests, the right imaging — is what separates a patient who improves from one who keeps managing the same pain for years.
Dr. Mayank Chauhan, Senior Orthopedic Surgeon at Prakash Hospital, Sector 33, Noida, evaluates and treats the full spectrum of joint conditions — from sports injuries and bursitis to advanced arthritis requiring knee or hip replacement. For patients who need non-surgical management, the clinic also coordinates with physiotherapy and pain management. For those who need surgical intervention, Dr. Chauhan's focus is on outcomes that last — not just immediate pain relief.
Patients across Noida, Greater Noida, Ghaziabad, and Delhi NCR come to Prakash Hospital for orthopedic consultation. The waitlists are manageable, and most patients can be seen within a reasonable timeframe for a first consultation.
To book an appointment with Dr. Mayank Chauhan in Noida, call the number listed on the website.
The Bottom Line
Joint pain is almost always treatable. The outcome depends heavily on three things: an accurate diagnosis, the right treatment plan, and the patient's commitment to seeing that plan through — whether it involves physiotherapy, weight loss, medication, or eventually surgery.
Don't normalise joint pain. Don't accept "just take these tablets and come back in three months" as a complete response to a problem that's affecting your sleep, your movement, and your daily life. You deserve a clear answer about what's wrong and a clear plan for fixing it.
If you're in Noida or Greater Noida and dealing with persistent joint pain, book a proper evaluation.
To consult Dr. Mayank Chauhan, Senior Orthopedic Surgeon in Noida, call the number listed on the website.