Joint Pain In The Elderly - Causes, Risks, And The Best Treatment Options

An elderly man with gray hair and glasses stands against a light blue background, wincing as he clutches the back of his neck with one hand.
Most families in Noida have a version of the same story. An elderly parent or grandparent who used to walk to the market every morning started doing it less. Then stopped. Now they say getting up from a chair hurts. Climbing stairs is difficult. They sleep poorly because the knee or hip aches through the night. The family assumes it's just old age. The elder has accepted it as their lot. And months or years pass without anyone asking whether something could actually be done about it. Something usually can.
Joint pain in elderly people is common, but "common" does not mean "inevitable" or "untreatable." A significant proportion of mobility loss, fall risk, and loss of independence in older adults can be traced to musculoskeletal conditions that respond well to the right treatment. The earlier that treatment begins, the better the outcome.
This guide is for families in Noida and Greater Noida whose elderly parents or grandparents are dealing with joint pain, and for the elderly individuals themselves who are tired of being told to "just manage."
Why Do Joints Deteriorate With Age?
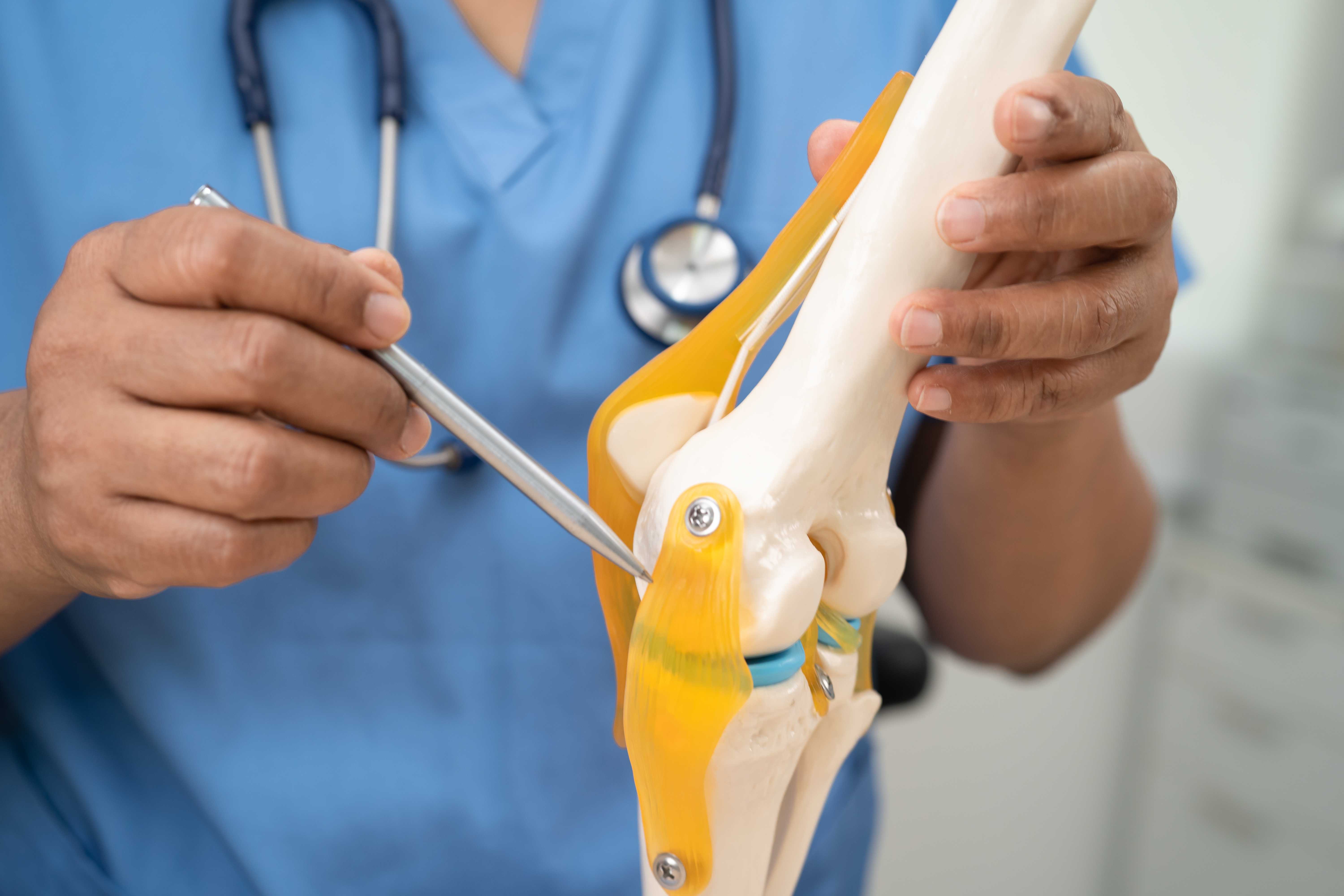
Understanding why this happens makes it easier to understand what can be done about it.
Cartilage thinning: Articular cartilage, the smooth cushioning surface at the ends of bones, gradually loses water content and elasticity with age. It becomes thinner and less able to absorb shock. In weight-bearing joints like the knee and hip, this thinning accelerates with the forces applied over decades of walking, standing, and climbing stairs.
Synovial fluid changes: The lubricating fluid inside the joint decreases in volume and changes in viscosity with age. Less effective lubrication means more friction between joint surfaces during movement.
Muscle mass loss (sarcopenia): From around age 30 onwards, adults lose muscle mass steadily, a process called sarcopenia. Weaker muscles around a joint provide less shock absorption and less stability. The joint bears more direct load as a result.
Bone density decline: Osteoporosis, the loss of bone density, becomes increasingly common with age, particularly in women after menopause. Weaker bones are more susceptible to fractures, including hip fractures, which are among the most serious orthopedic events in elderly patients.
Ligament stiffening: The ligaments that stabilise joints become less flexible with age. This contributes to stiffness, reduced range of motion, and increased injury risk from falls.
Cumulative injury: Decades of physical activity, work, and previous injuries leave their marks. Old injuries that seemed fully healed can contribute to accelerated joint degeneration years later.
The Most Common Joint Conditions In Elderly Patients In Noida
Joint conditions are increasingly common among elderly patients in Noida, often affecting mobility, independence, and overall quality of life with age.
1. Knee Osteoarthritis
By far the most common orthopedic condition in elderly Indians. Prevalence estimates suggest that more than 45% of Indians over 65 have clinically significant knee osteoarthritis. In women, the rate is even higher. Knee OA progresses through grades, from mild cartilage thinning (Grade 1) to bone-on-bone contact with severe deformity (Grade 4). Treatment at each grade looks different: Grade 1–2 responds very well to conservative management; Grade 3–4 often benefits from surgical intervention.
The visible signs of advanced knee OA, such as a bowing of the legs, difficulty straightening the knee fully, and visible swelling around the joint, are familiar to most families with elderly relatives.
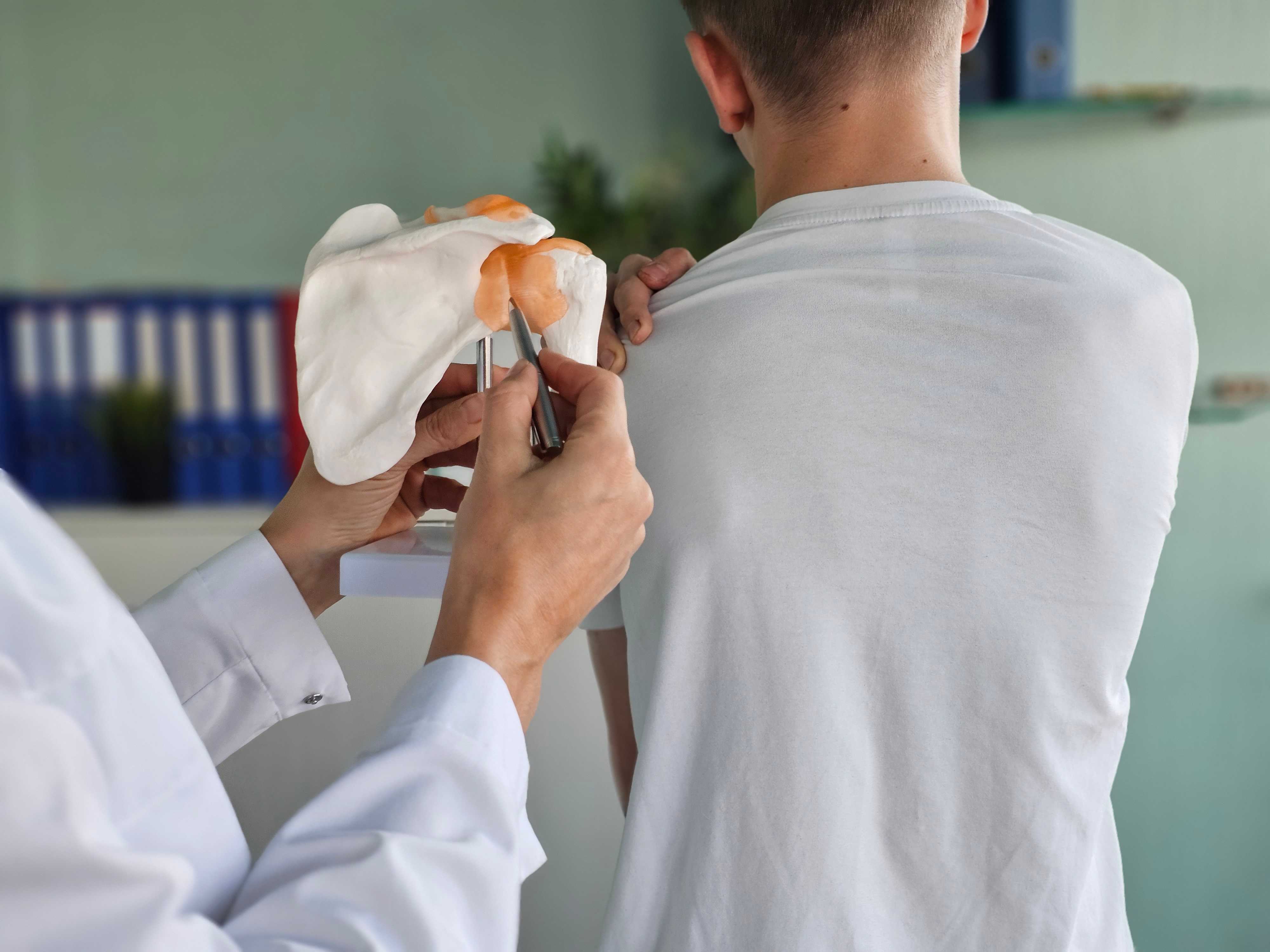
2. Hip Osteoarthritis
Less visually obvious than knee OA, but equally disabling. Hip arthritis causes a characteristic pattern: groin pain (not always where patients expect it), pain radiating into the thigh, and a reduced ability to rotate the leg outward. Walking, getting in and out of cars, and rising from low chairs become progressively harder.
Hip replacement has even higher success rates than knee replacement. In most studies, patients typically describe more complete relief of pain than knee replacement patients. Yet many elderly patients in Noida delay hip replacement significantly longer than necessary, often because the family isn't aware that surgery is an option or because they fear the risks.
3. Osteoporosis And Fractures
Osteoporosis itself doesn't cause joint pain directly, but it dramatically increases fracture risk. Hip fractures in the elderly from falls that a younger person would walk away from are among the most serious medical events of old age. Around 20% of elderly patients who sustain a hip fracture do not survive the following year. The majority of survivors experience significant long-term loss of mobility and independence. Yet osteoporosis is preventable and treatable, and most elderly Indians have never had a bone density scan (DEXA) to assess their risk.
4. Spinal Degeneration
Degenerative changes in the lumbar spine, such as disc dehydration, facet joint arthritis, and spinal stenosis, are nearly universal in people over 70. The key question is whether these changes are causing significant symptoms. Spinal stenosis (narrowing of the spinal canal) causes a characteristic pattern: leg pain and weakness that come on with walking and are relieved by sitting or bending forward. This is different from sciatica and has its own management pathway.
5. Gout
Gout affects elderly patients of both sexes somewhat more commonly in men and causes sudden, extremely painful joint inflammation, most typically in the big toe, ankle, or knee. It is caused by elevated uric acid in the blood, depositing crystals in the joint. Gout is highly treatable, but many elderly patients in Noida manage gout attacks for years with general painkillers rather than getting proper uric acid control.
The Specific Risks Of Untreated Joint Pain In Elderly Patients
Families often assume that elderly joint pain is simply part of ageing and doesn't need active management. This view has consequences.
Fall risk: Painful joints lead to reduced muscle strength, altered gait, and compensatory movements that significantly increase fall risk. Falls in the elderly, particularly hip fractures, can be catastrophic. Joint pain treatment that improves strength and stability reduces fall risk.
Reduced activity and deconditioning: Pain causes inactivity. Inactivity causes further muscle loss. Weaker muscles put more load on already arthritic joints, accelerating the problem. This is a downward spiral that becomes harder to interrupt the longer it runs.
Social isolation and depression: Elderly patients who can't move comfortably stop participating in family activities, outings, and social engagements. Isolation in the elderly is a significant risk factor for cognitive decline and depression.
Medication overuse: Many elderly patients in Noida manage chronic joint pain with long-term NSAID use (ibuprofen, diclofenac) without medical supervision. In elderly patients, prolonged NSAID use carries serious risks of gastrointestinal bleeding, kidney damage, and cardiovascular effects. Proper orthopedic management typically reduces the need for these medications.
Sleep deprivation: Chronic pain disrupts sleep. Poor sleep in the elderly affects cognitive function, immunity, mood, and cardiovascular health. Treating joint pain can dramatically improve sleep quality and overall well-being.
Treatment Approach For Elderly Patients - What's Different

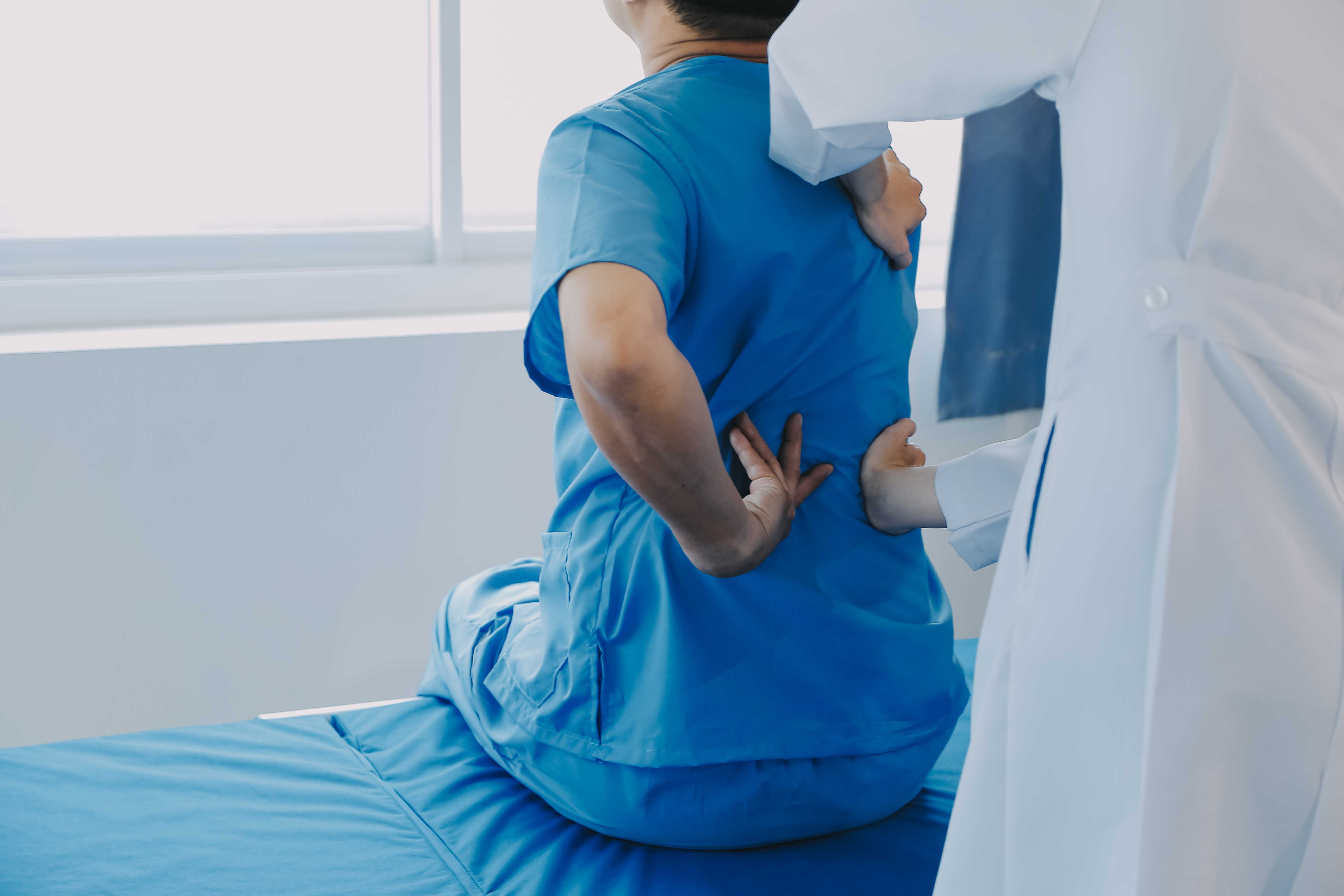
A female doctor is making notes and examining an elderly female patient as she stands in front of her, holding her back in pain.
The principles of joint pain management for elderly patients are similar to those for younger adults, but the execution is different. Elderly patients often have multiple health conditions, take several medications, have lower physiological reserve, and may have social circumstances (living alone, limited family support) that affect what's practical.
1. Modified Exercise And Physiotherapy
Exercise is the most evidence-based intervention for osteoarthritis at any age, and elderly patients benefit enormously from it. The concern that "exercise will make it worse" is almost always wrong. The right exercise makes it better. For elderly patients, exercise recommendations are adapted:
- Seated exercises are often more appropriate than standing exercises initially, particularly for those with balance issues.
- Water-based exercise (hydrotherapy): Exercising in a warm pool takes weight off the joints while allowing a full range of motion. Particularly valuable for elderly patients with severe arthritis or limited mobility.
- Walking aids: A walking stick reduces load on a painful hip or knee by approximately 25–30%. For elderly patients already walking with reduced confidence, a properly-fitted stick is both therapeutic and protective against falls.
- Low-impact activities: Chair yoga, gentle tai chi, and simple stretching can maintain flexibility and build the stabilising muscle strength that protects joints.
2. Medication Considerations
Medication choice in elderly patients requires more careful thought:
- Paracetamol remains the safest first-line option, though its effectiveness in moderate-to-severe arthritis is limited.
- Topical NSAIDs (diclofenac gel applied locally) are preferred over oral NSAIDs in the elderly, with the same local anti-inflammatory effect with far fewer systemic side effects.
- Oral NSAIDs should be used at the lowest effective dose for the shortest possible duration, always with a stomach-protecting medication (PPI), and with kidney function monitoring.
- Supplements: Vitamin D deficiency is extremely prevalent in elderly Indians and should be corrected. Calcium supplementation should be guided by blood levels and dietary assessment.
3. Injections In Elderly Patients
Intra-articular injections of corticosteroid or hyaluronic acid are safe and effective in elderly patients and provide significant relief, particularly for knee OA. They are particularly valuable as a bridge for patients who are not yet ready for surgery, or who have health conditions that make surgery higher risk. PRP (Platelet-Rich Plasma) therapy is also gaining traction in Noida and Delhi NCR for elderly OA patients, offering an alternative for those who prefer a biological approach or who have had limited response to steroid injections.
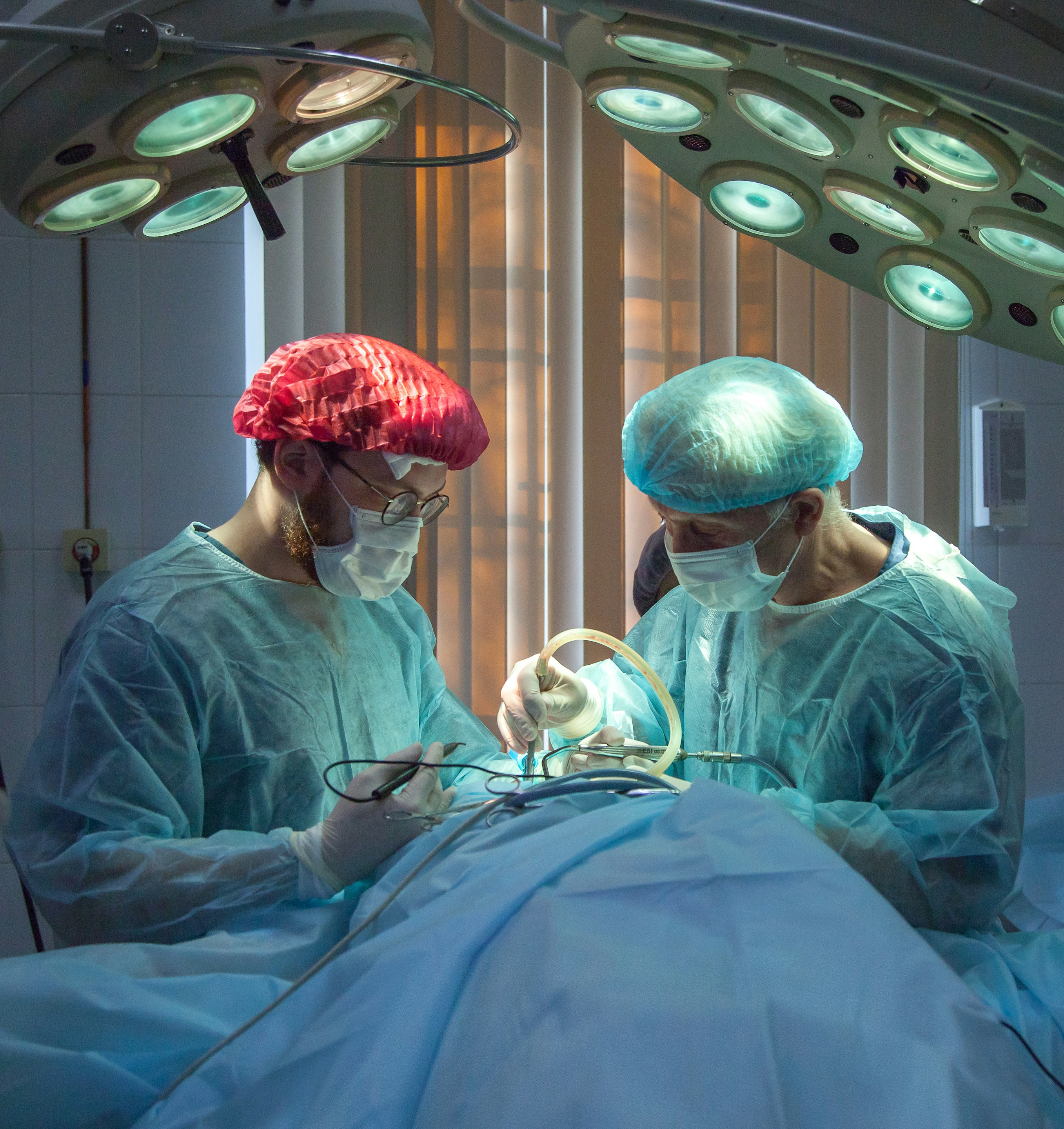
4. Surgery In Elderly Patients - Not As Risky As Families Fear
One of the most common misconceptions among families of elderly patients in Noida is that surgery is "too risky" for their parent or grandparent. This is not well-founded as a general statement.
Joint replacement surgery in medically optimised elderly patients has excellent safety records. Modern anaesthesia, surgical techniques, and post-operative care have made knee and hip replacement routine in patients in their 70s and 80s. The pre-operative medical evaluation identifies and addresses the specific risk factors for each patient.
The question is not "is surgery too risky for elderly patients?" but rather "has this specific patient been properly evaluated for their individual surgical risk?" A well-controlled 75-year-old with knee OA and no other significant health problems is typically a good candidate for knee replacement.
The risks of not treating severe arthritis in the elderly, continued pain, deconditioning, fall risk, isolation, and medication overuse are often greater than the risks of carefully planned surgery.
When To See An Orthopedic Surgeon For An Elderly Relative
Families in Noida sometimes wait too long to seek orthopedic consultation for elderly members. These are the signs that indicate it's time:
- Joint pain that is present every day and affects basic daily activities.
- Difficulty getting up from a chair or bed without assistance.
- A change in gait, limping, shuffling, or leaning to one side.
- Swollen, warm, or deformed joints.
- History of a fall, or increasing fear of falling.
- Pain wakes them from sleep regularly.
- Visible bowing of the legs or knock-knee deformity.
- Inability to walk distances they could manage 6–12 months ago.
A consultation doesn't commit the patient to surgery. It provides a clear picture of what's happening, what the options are, and what the realistic expectations for each treatment are, giving the family and the patient the information to make a properly informed decision.
Dr. Mayank Chauhan - Orthopedic Care For Elderly Patients In Noida
At Prakash Hospital, Sector 33, Noida, Dr. Mayank Chauhan routinely evaluates and treats elderly patients with all forms of joint disease, from early-stage arthritis managed conservatively to advanced joint disease requiring replacement surgery.
His approach with elderly patients includes careful attention to their overall medical status, the practical realities of their home situation and family support, and a treatment plan that is matched to what is realistic and beneficial for that specific person, not a generic protocol.
For elderly patients in Noida, Greater Noida, and surrounding areas for whom travel is a concern, initial consultation availability should be confirmed when booking. To book a consultation for an elderly relative with Dr. Mayank Chauhan, call the number listed on the website.
The Bottom Line

An elderly man sitting at home holding his knee, depicting age-related joint pain commonly seen in osteoarthritis.
Joint pain in the elderly is treatable. Mobility can be restored. Independence can be preserved or recovered. The key is not accepting joint pain as an unavoidable consequence of age and doing nothing. If an elderly parent or grandparent in Noida is living with significant joint pain that's limiting their daily life, they deserve a proper orthopedic evaluation. Not a prescription for pain medication and a suggestion to "take it easy." A real assessment, real options, and a real plan. To book a consultation with Dr. Mayank Chauhan, Senior Orthopedic Surgeon in Noida, call the number listed on the website.