Degenerative Disc Disease: What You Need To Know

Illustration of inflamed and degenerated discs in the lower spine.
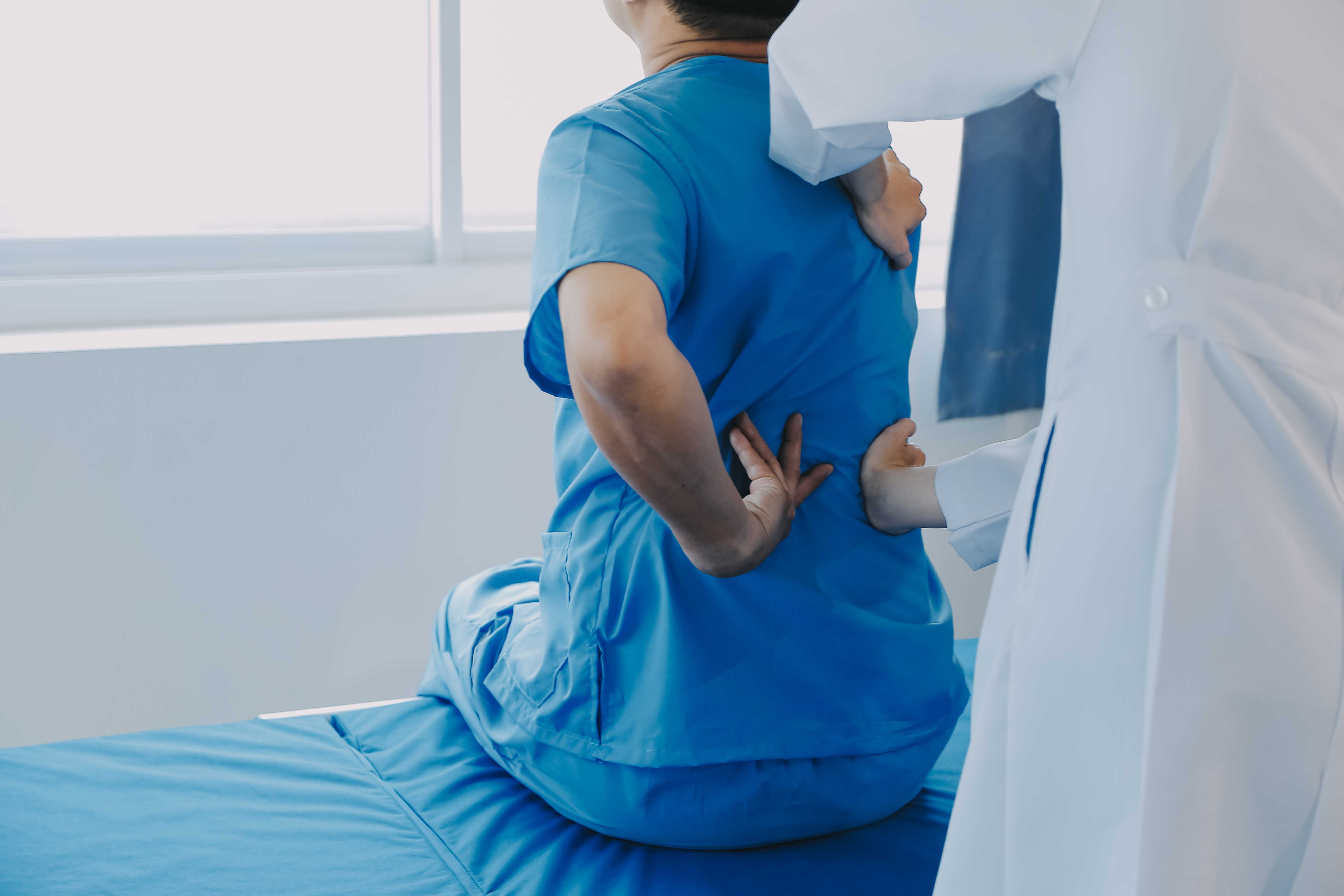
It's often dismissed as just being due to age or something that will pass on its own. However, often it's related to something known as degenerative disc disease. Actually, it isn't truly a disease; it's actually the long, gradual process of wear and tear that the discs in our spine undergo over a lifetime.
With time, discs lose their flexibility and cushioning, resulting in discomfort, stiffness, and restricted movement. Degenerative disc disease can afflict anyone, but it most commonly occurs in those with sedentariness, physically strenuous careers, or improper postural mechanics.
Degenerative disc disease can not only be extremely painful, but may also interfere with one's daily routine, creating discomfort in the simplest actions like bending, sitting, or lifting. Fortunately, treatment is widely available and can effectively manage symptoms while limiting future deterioration.
In this guide, we will look at degenerative disc disease, what it involves, how it occurs, and when a consultation with an orthopedic specialist is recommended.
What Is Degenerative Disc Disease?
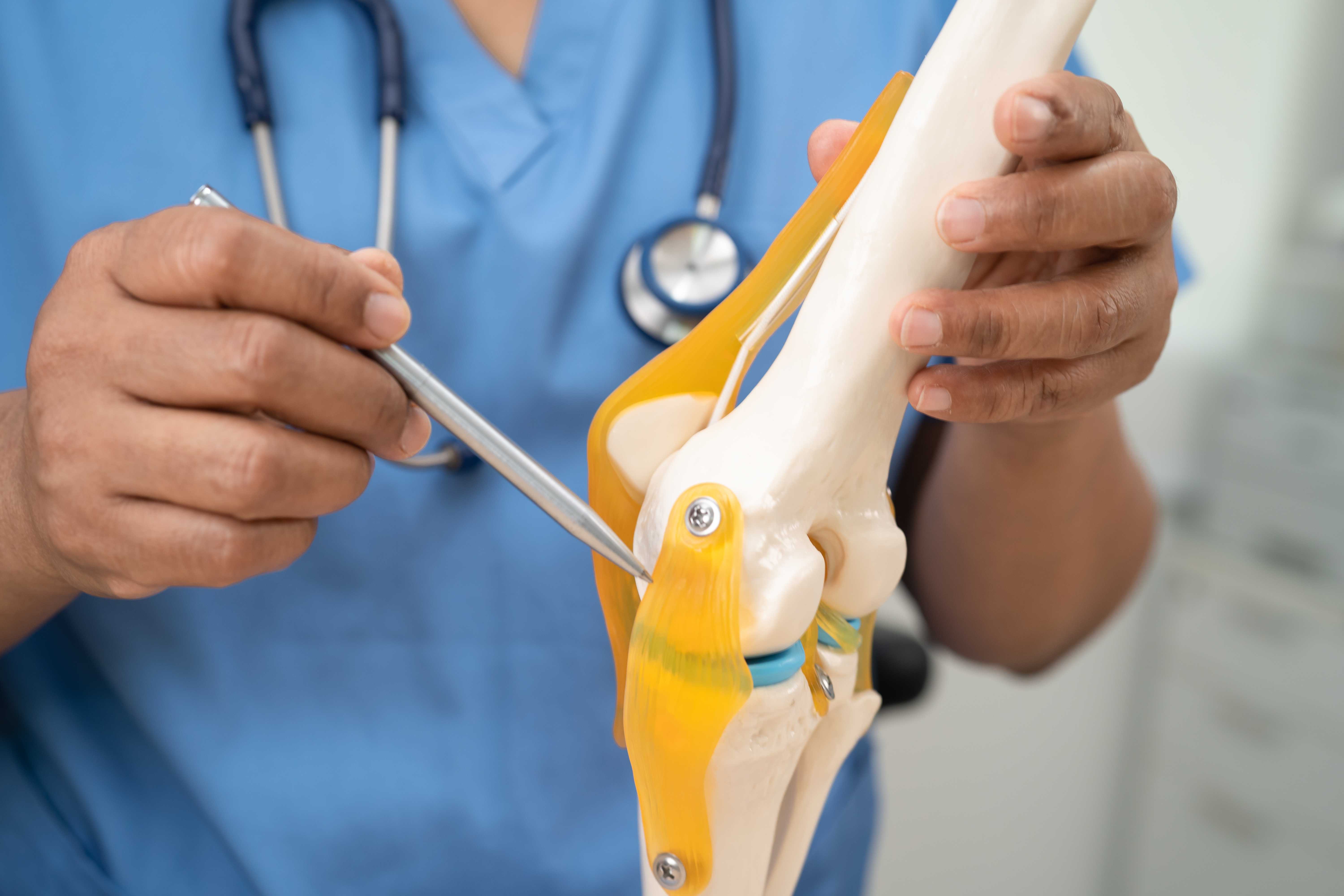
Degenerative disc disease is basically the deterioration of the intervertebral discs that are the shock absorbers situated between the bones that make up the spinal column. These discs cushion the bones in the spine and facilitate smooth motion.
These discs can become thinner and can become dehydrated over a period of time or even have small tears or splits in them, diminishing their effectiveness as a cushion and allowing pain and stiffness to develop.
Whilst it is naturally an aging-related condition, several lifestyle habits or predispositions can cause premature wearing of the discs, such as poor posture or continuous strain and stress to the discs, as well as physical injuries and being physically inactive.
How Does Degenerative Disc Disease Develop?
This generally occurs over a longer period of time. Discs may lose their water content, which decreases their flexibility and makes them more susceptible to injury. Cracks may develop on the outside, which may irritate or inflame nerves in the spine. This may cause bone rubbing, disc herniation, or unstable vertebrae in extreme cases.
Knowing how severe the DDD is and receiving a plan of treatment that's correct requires seeing an experienced orthopedic specialist, such as Dr. Mayank Chauhan in Noida.
Symptoms Of Degenerative Disc Disease
The signs and symptoms are dependent upon which discs are involved and to what extent they are damaged.
- Long-lasting back pain or neck pain - This may be dull or sharp pain, which can be worse when sitting or after bending and lifting.
- Pain in other limbs - Pain can travel to the arms or legs if the nerves close to the affected discs are compressed.
- Stiff and inflexible spine - The spine becomes difficult to move freely, particularly after resting for a long period.
- Movement helps relieve the pain - The condition differs from many other forms of pain in that gentle exercise, like walking, actually offers relief.
- Tingling and numbness in limbs - Nerve compression may cause sensations of tingling in the arms or legs, loss of feeling, and even weakness.
Causes And Risk Factors
Several factors may cause degenerative disc disease:
1. Aging

A woman is holding her back in pain.
This is the most common cause, with the normal effects of wear and tear on our spines being most apparent with age. Spinal discs lose water content over the course of our lives, becoming stiffer and less effective at absorbing impact, leading to degeneration.
2. Sedentary Lifestyle
Lack of movement weakens our core and back muscles that provide support to our spines. As these muscles fail to support our spines, pressure increases directly on the discs, causing more potential damage.
3. Bad Posture
Leaning and slouching over long periods of time causes repetitive, uneven stress on our spines. With time, this added pressure leads to increased wearing out of the discs. This effect will be most noticeable on your neck and lower back.
4. Repetitive Strain Or Heavy Lifting
Jobs that involve repetitive bending and twisting motions, and continuous lifting of heavy items, place great stress on our spines. Long term damage may occur that, over time, may weaken spinal discs further, leading to small tears.
5. Injury Or Trauma
Sudden impacts may damage spinal discs. Falling from great heights and being involved in high-speed accidents may seriously impact spinal discs. Even minor injuries, though, will place stress on our discs and, over time, may cause them to wear out more quickly.
6. Genetics
Some people are predisposed to disk degeneration because of a genetic predisposition that influences their discs' structure, durability, and strength.
7. Overweight Or Obesity
Extra body weight means that there is more pressure exerted on the spine, especially on the lumbar region. As there is added pressure on your spine, there may be an accelerated wear on your spinal discs, and their effects may be exacerbated.
8. Smoking
This restricts blood flow and the amount of oxygen delivered to spinal tissue, reducing the spinal discs' ability to self-repair. It can speed up wear on your spinal discs.
9. Dehydration
Disks need to be adequately hydrated to retain their function as shock absorbers. When a body is dehydrated, spinal discs become less elastic and more prone to cracking and shrinkage.
10. Occupational Hazards
Jobs that require long hours of sitting, prolonged or repetitive twisting, constant lifting of heavy objects, and vibrations (e.g. Driving) put enormous strain on our spines.
Non-Surgical And Surgical Treatment Options
How your treatment is planned depends on the severity of your symptoms and how they are impacting your everyday life. The ultimate goal of your treatment plan will be to help decrease pain and allow you to move better without further damaging your spine.
1. Non-Surgical Treatment Options
Many patients with degenerative disc disease do not need surgery, especially with the earlier diagnoses they receive today.
- Physiotherapy - A significant element in managing symptoms of degenerative disc disease, this focuses on strengthening the muscles of the trunk and back, enhancing flexibility, and achieving appropriate posture. An exercise program will help ease the pressure off your spinal discs. The more stability you have in the spine, the greater long-term relief you will find.
- Medications - A doctor may prescribe anti-inflammatory drugs, muscle relaxants, or pain relievers to assist in reducing pain and inflammation of the nerves and spine. They generally provide short-term pain management and do not aid with more long-term concerns.
- Lifestyle adjustments - Minor lifestyle changes can greatly impact symptom management. Making sure your body mass index is appropriate is a big component. Also, making an effort to maintain proper posture during sitting, standing, and lifting will limit further damage to your spinal discs. Low-impact exercise, such as swimming or walking, will increase your spinal stability.
- Heat and cold treatments - These are common treatment strategies that work in opposite ways. Hot treatments relax stiff muscles and increase blood flow, while cold treatments decrease inflammation and numb painful spots. Alternating between hot and cold treatments may be beneficial.
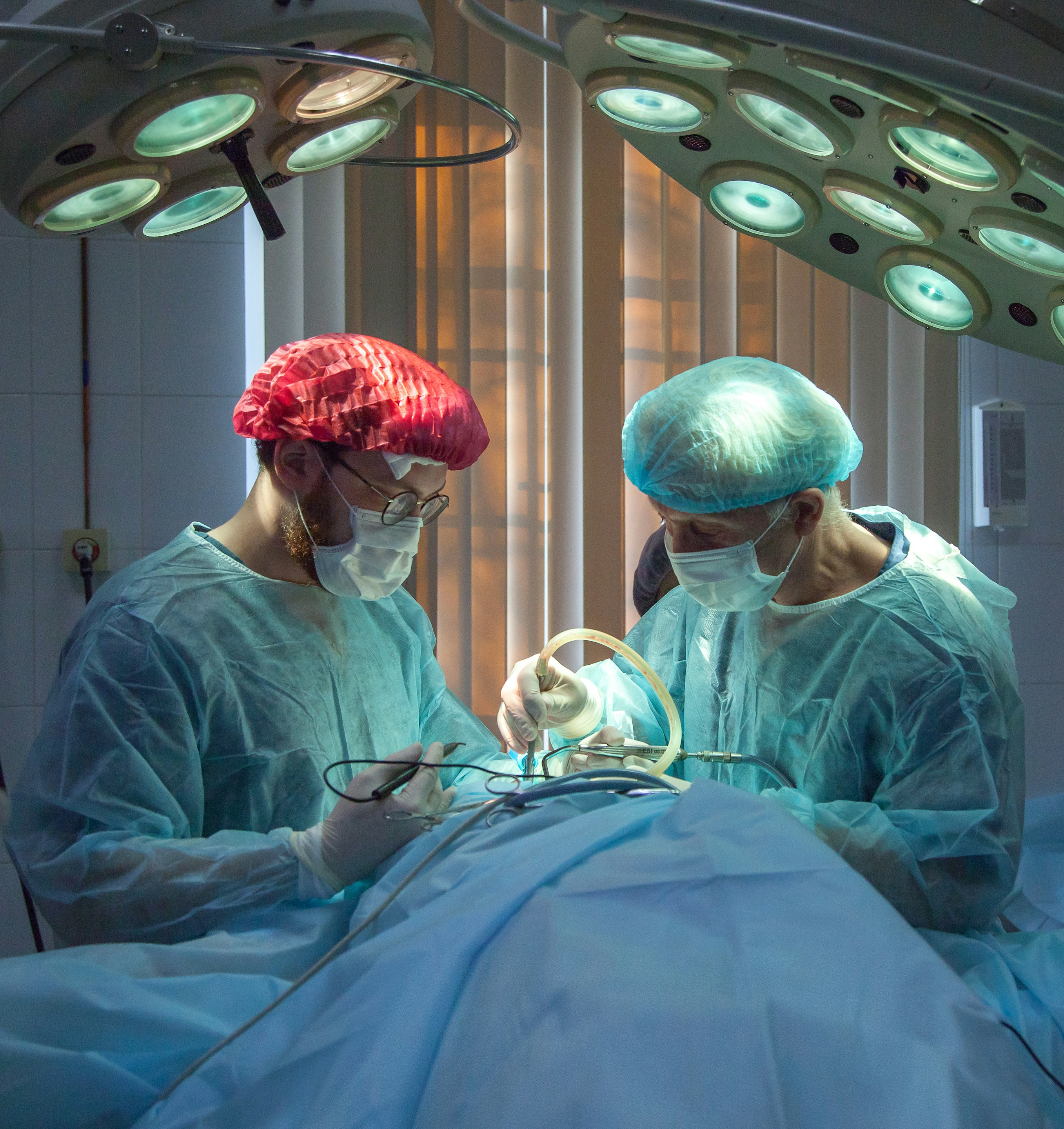
2. Surgical Treatment Options

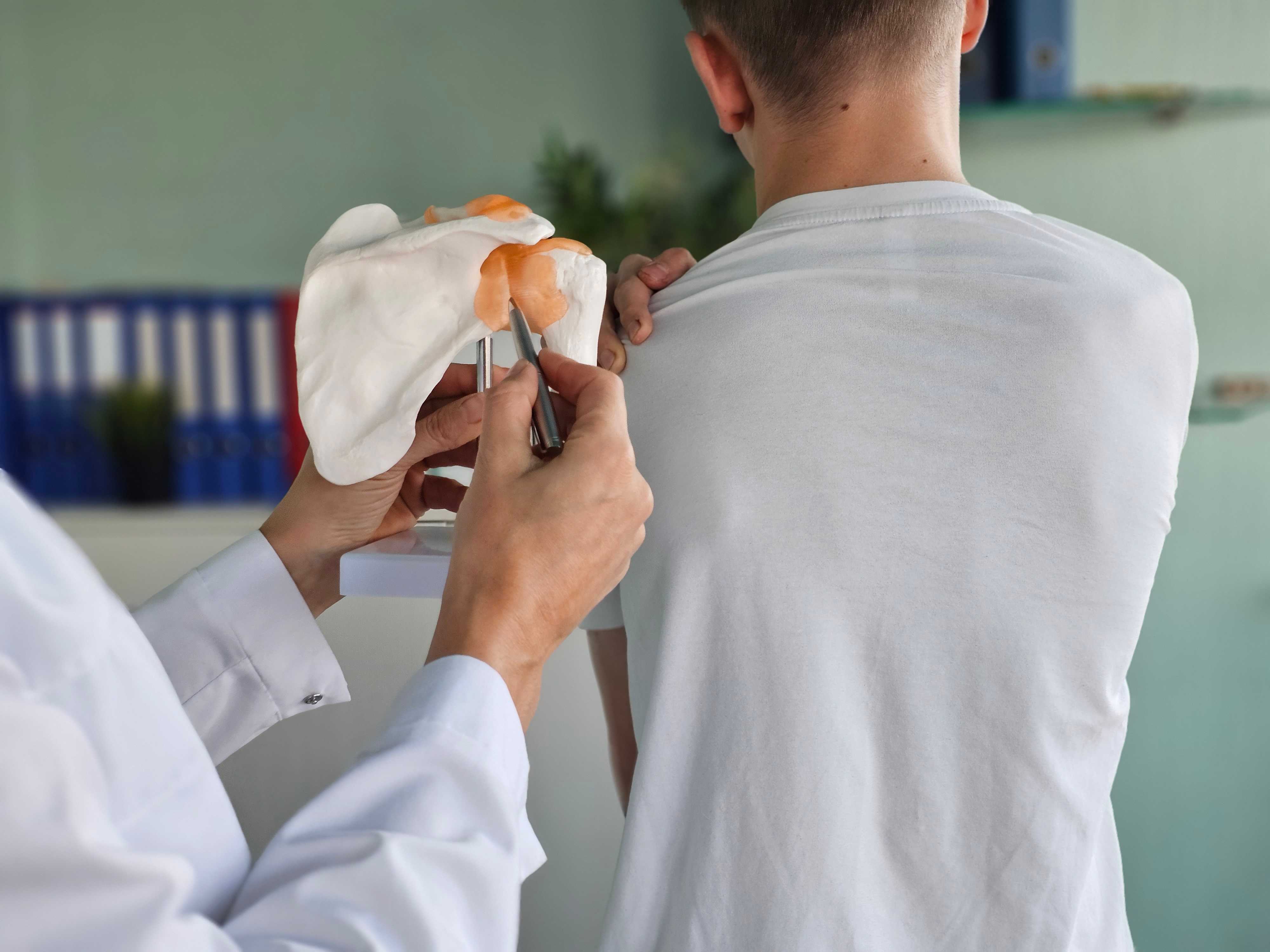
A doctor is explaining the anatomy of a spine.
Surgery is only recommended for individuals who haven’t found relief from non-surgical options and who have extreme pain, nerve compression, or functional loss.
- Discectomy - This operation entails taking away parts of the vertebrae that are damaged or that are herniated in the spine that are affecting the spinal nerve. Relief may be seen in the way the pressure has been taken off of your discs within the spine.
- Spinal fusion - This operation permanently connects two or more of your vertebrae within the spine. The spinal segment is significantly limited in its movement and can bring relief from unstable discs within the spine.
- Artificial disc replacement - This is a more recent type of spinal operation where the damaged spinal disc is replaced with an artificial equivalent, allowing the spine more natural movement.
When To See An Orthopedic Specialist
There are a few 'red flag' symptoms that you should never ignore, as these indicate when it is time to consult medical care:
- Pain lasting several weeks - Constant pain persisting over several weeks may indicate that a degree of disc damage is present.
- Painful tasks are impossible to carry out - If carrying out normal tasks is a painful process, then you should be seeking medical advice.
- Numbness or weakness in your limbs - Numbness and weakness indicate that your nerves are becoming compressed.
- Recurring bouts of back pain - Constant episodes of pain could mean the degeneration within your spine is progressing.
Final Thoughts
Degenerative disc disease is a widespread but treatable disorder. Although the name of the disorder can seem intimidating, seeing a specialist for an early diagnosis and appropriate treatment can lead to a great increase in quality of life.
The symptoms of the disease can be managed with adequate posture control, exercise, early and correct treatment, and it will prevent other problems that are potentially serious.
Seeking treatment from an efficient orthopaedic specialist such as Dr. Mayank Chauhan in Noida would make a significant difference in the way a diagnosis and treatment occur; such patients are provided with answers to their pain and mobility, and overall better health.
Frequently Asked Questions (FAQs)
1. The main reason for the occurrence of Degenerative Disc Disease?
Natural aging leads to the steady deterioration, drying, and reduction in the thickness of discs within the spine.
2. Can degenerative disc disease be cured?
No. However, it can be controlled using correct therapy and lifestyle modifications.
3. Is walking good for DDD?
Yes, it is a non-impact activity that increases range of motion, strengthens the supporting muscles of the spine, and decreases stiffness.
4. In which circumstances should surgery be considered for DDD?
If a lack of mobility, paralysis, or debilitating pain does not resolve with the appropriate non-surgical treatment.