Can Slip Disc Heal Without Surgery? What Orthopedic Experts Actually Say

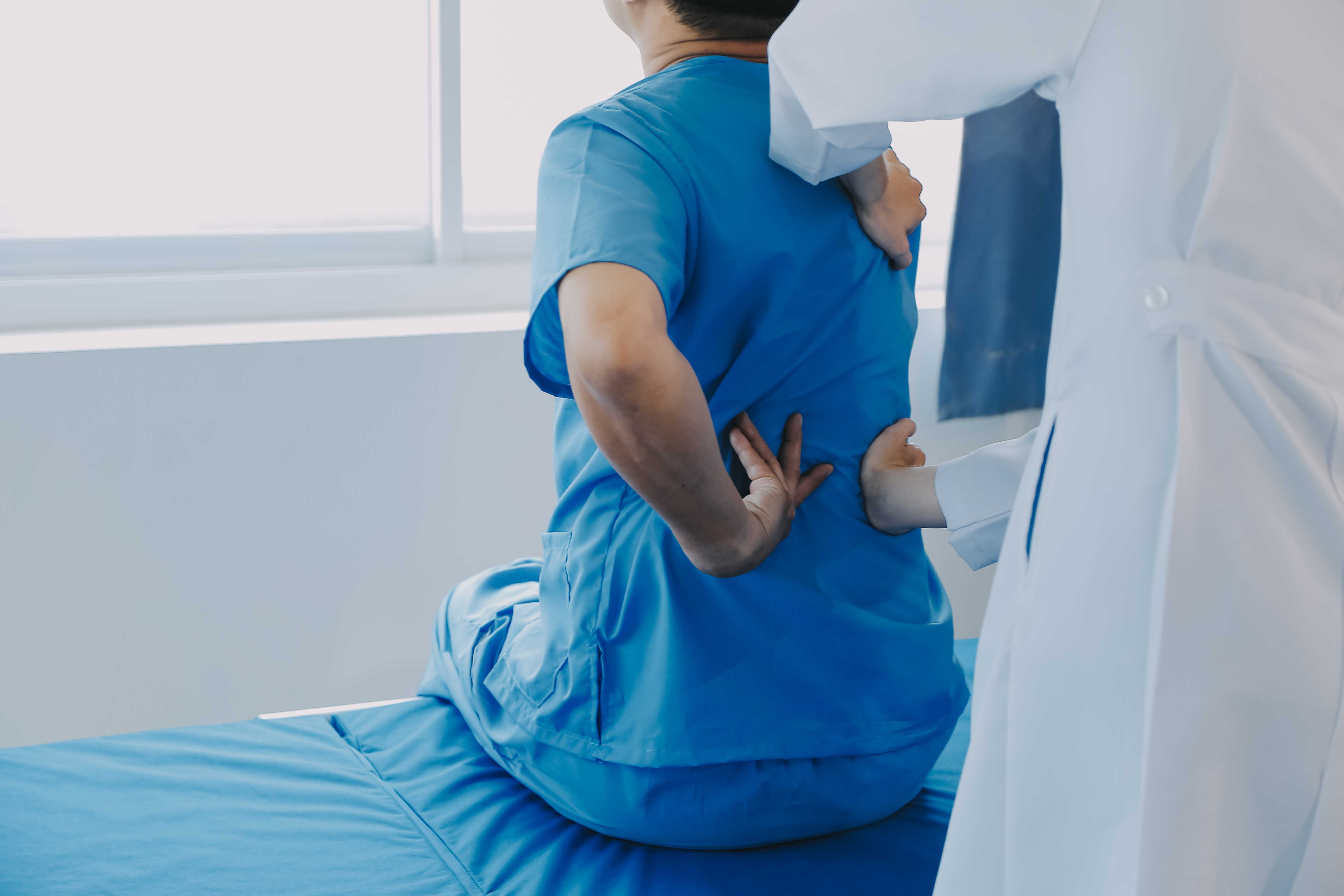
A young man stands indoors pressing his lower back, illustrating acute lumbar pain or muscle strain in a home setting.
This is the first question nearly every patient with a slipped disc asks. It's asked in the consulting room, in WhatsApp groups, in late-night searches when the leg is burning, and sleep feels impossible. And it deserves a direct, honest answer, not reassuring platitudes and not unnecessary alarm.
So here it is: In the vast majority of cases, estimated between 80 and 90 percent, a slipped disc improves significantly with non-surgical treatment alone. Most patients never need surgery. The body has a remarkable capacity to manage disc herniations through its own processes, supported by the right treatment.
But that does not mean every slipped disc heals without attention. "Without surgery" is not the same as "without treatment." And it does not mean that doing nothing, rest, painkillers, waiting, is a strategy that works for everyone. It means the right non-surgical treatment, done consistently, produces good outcomes for most patients.
This guide explains how and why the disc heals, what non-surgical treatment actually involves, how long recovery takes, and critically, which situations genuinely require surgery.
What Actually Happens When A Disc "Heals"
A slipped disc, medically known as a herniated or prolapsed intervertebral disc (PIVD), occurs when the soft inner core (nucleus pulposus) of an intervertebral disc pushes through a tear in the tough outer ring (annulus fibrosus). This herniated material presses on nearby spinal nerves, causing the pain, radiating leg symptoms, numbness, and tingling that patients describe. When we say a disc "heals," three processes can happen, and often all three occur together over weeks and months:
Resorption of the disc material: The herniated disc material that has entered the spinal canal is a biological substance that the body's immune system recognises as foreign. Inflammatory cells, macrophages in particular, are recruited to the site and gradually break down and absorb the herniated material. Studies using MRI follow-up have confirmed that disc herniations reduce in size over time, and in many cases, the herniated fragment disappears entirely on imaging. Larger herniations, paradoxically, often resorb faster than smaller bulges because more disc material creates a stronger immune response.
Reduction in nerve inflammation: Even when the disc material doesn't fully resorb, the acute inflammatory response around the compressed nerve settles over time. As inflammation reduces, nerve pain decreases even if some degree of disc herniation remains visible on MRI.
Adaptation of the nervous system: With appropriate treatment, the nervous system gradually desensitises to the mechanical pressure of the herniation. This "neural adaptation" is why many patients continue to improve even when their MRI shows residual disc changes.
The timeline for this process is typically 6 to 12 weeks for significant improvement, though the MRI changes may take several months to a year to fully resolve.
What Non-Surgical Treatment Actually Involves
The phrase "conservative treatment" often gives patients the wrong impression that it means passive, gentle, low-effort management. In reality, effective non-surgical treatment for a slipped disc is structured, active, and requires commitment. Here's what it looks like in practice.
Phase 1: Acute Pain Management (Weeks 1–2)
The priority is controlling pain enough for the patient to begin moving. This typically involves:
Medications:
- NSAIDs (ibuprofen, diclofenac, etoricoxib) - reduce inflammation around the nerve. First-line for mild-to-moderate disc pain. Used for the shortest effective period.
- Muscle relaxants (cyclobenzaprine, chlorzoxazone) - address the muscle spasm that inevitably accompanies disc herniation, making movement easier.
- Nerve pain medications (pregabalin, gabapentin) - specifically target the burning, electric, or shooting nerve pain (neuropathic pain) that radiates down the leg. More effective for sciatica-type symptoms than standard painkillers.
- Short-course oral steroids - in cases of very severe pain or significant nerve compression, a 5-7 day tapered course of oral prednisolone can rapidly reduce nerve inflammation and provide significant short-term relief, buying time for physiotherapy to begin.
Modified rest: The old prescription of strict bed rest for 2 weeks is outdated and counterproductive. Short relative rest (1-2 days of reduced activity during the most acute phase) is acceptable. Prolonged bed rest causes muscle deconditioning, increases disc pressure in some positions, and slows recovery. After the acute peak, gentle movement is actively encouraged.
Position and posture: For lumbar disc herniation, many patients find lying on their back with knees bent, or lying on their side with a pillow between the knees, most comfortable. Sitting, particularly prolonged sitting with a slumped posture, is typically the worst position during the acute phase. For Noida's desk-working patients, this means working from a raised surface or standing if possible, and taking movement breaks every 30-45 minutes.
Phase 2: Active Physiotherapy (Weeks 2–8)
This is where the recovery happens. Physiotherapy for slip disc is not massage and heat pads, it's a targeted, evidence-based intervention programme.
McKenzie Method (Mechanical Diagnosis and Therapy): The most extensively studied physiotherapy approach for lumbar disc herniation. The central principle is identifying directional preference movements that "centralise" the pain (draw the radiating leg pain back toward the spine). For most lumbar disc herniations, extension movements (backward bending) achieve this. As pain centralises with repeated extension exercises, the herniated material mechanically shifts back toward the disc centre, reducing nerve pressure.
A trained McKenzie physiotherapist assesses each patient's response to specific movements and designs a personalised exercise programme. Success rate when properly applied: 70-80%, significant improvement without further intervention.
Core stabilisation: The deep spinal stabilisers, the transversus abdominis and multifidus muscles, act as the body's natural corset, protecting the disc from mechanical stress. In patients with disc herniation, these muscles are inhibited by pain. Specific core stabilisation exercises progressively retrain these muscles, providing ongoing spinal protection and significantly reducing recurrence risk.
Neural mobilisation (nerve gliding): Gentle exercises that move the compressed nerve through its pathway, such as the "sciatic nerve floss," reduce neural adhesions and improve nerve mobility. Particularly helpful when tingling and radiating symptoms are prominent.
Traction: Mechanical lumbar traction applies a controlled pulling force to the spine, creating negative intradiscal pressure that may draw the herniated material back. The evidence is mixed; some patients respond very well, others do not. Generally worth trying for acute, large herniations when other approaches have been insufficient.
Posture and ergonomics education: For the working population in Noida's corporate sector, understanding how to sit, stand, lift, and sleep, and actually implementing it, is a significant component of both recovery and prevention. This is not a one-time conversation but an ongoing part of physiotherapy sessions.
Phase 3: Injection Therapy (When Needed)

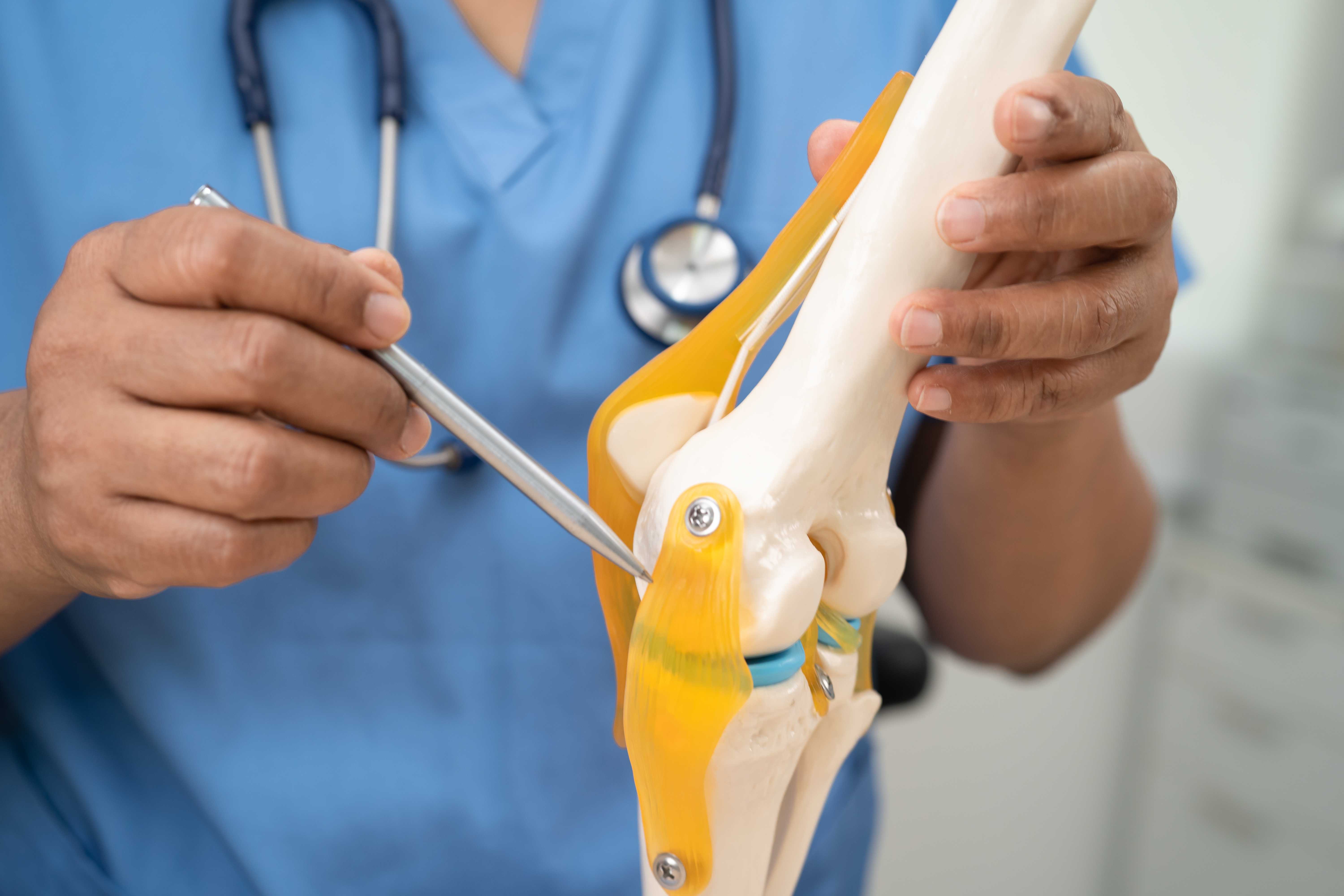
A detailed spine image highlighting a slip disc compressing nerves and causing radiating back pain.
When adequate physiotherapy and medication have not produced sufficient improvement after 4-6 weeks, epidural steroid injection is the next step.
Transforaminal Epidural Steroid Injection (ESI): The most targeted approach is to inject corticosteroid directly around the compressed nerve root under imaging guidance (fluoroscopy or CT). This delivers powerful anti-inflammatory medication to precisely the right location. Most patients experience significant relief within 1-2 weeks of injection. The window of reduced pain typically allows more intensive physiotherapy. Effect duration: 6-12 weeks, sometimes longer. Most patients require one to three injections.
This is not surgery. It is a targeted injection done as an outpatient procedure. It carries minimal risk when done by an experienced clinician under imaging guidance.
How Long Does Recovery Take?
The honest answer depends on several factors: the size and level of the disc herniation, the severity of nerve compression, how quickly treatment is started, and how consistently physiotherapy is done.
General timeline for non-surgical recovery:
- Weeks 1-2: Pain management, modified activity, beginning gentle exercises.
- Weeks 2-6: Active physiotherapy, gradual improvement in leg symptoms, and core work begin.
- Weeks 4-8: Most patients notice a significant reduction in radiating symptoms. Walking distances increase.
- Weeks 6-12: Many patients have returned to full or near-full daily function.
- 3-6 months: Full recovery for most patients. Some residual MRI changes may remain, but without significant symptoms.
Factors that slow recovery:
- Starting treatment late.
- Inconsistent physiotherapy (doing exercises once a week instead of daily).
- Continuing to sit in positions that worsen disc pressure (prolonged slumped sitting).
- Smoking reduces the blood supply and slows tissue healing.
- Obesity increases the mechanical load on the disc continuously.
- High anxiety about the diagnosis, pain catastrophising, is associated with slower recovery and should be addressed.
The Factors That Determine Whether You Need Surgery
Most patients improve without surgery. But a minority genuinely do need it. The key is knowing which category you're in and not delaying necessary surgery while hoping conservative treatment will eventually work.
1. You Do Not Need Immediate Surgery If
- Your symptoms are pain and radiating leg discomfort without significant weakness or neurological deficit.
- Your symptoms have been present for less than 6-8 weeks, and you have not yet had adequate conservative treatment.
- Pain is manageable, and you can function with appropriate medication and physiotherapy.
- There is no loss of bladder or bowel control.
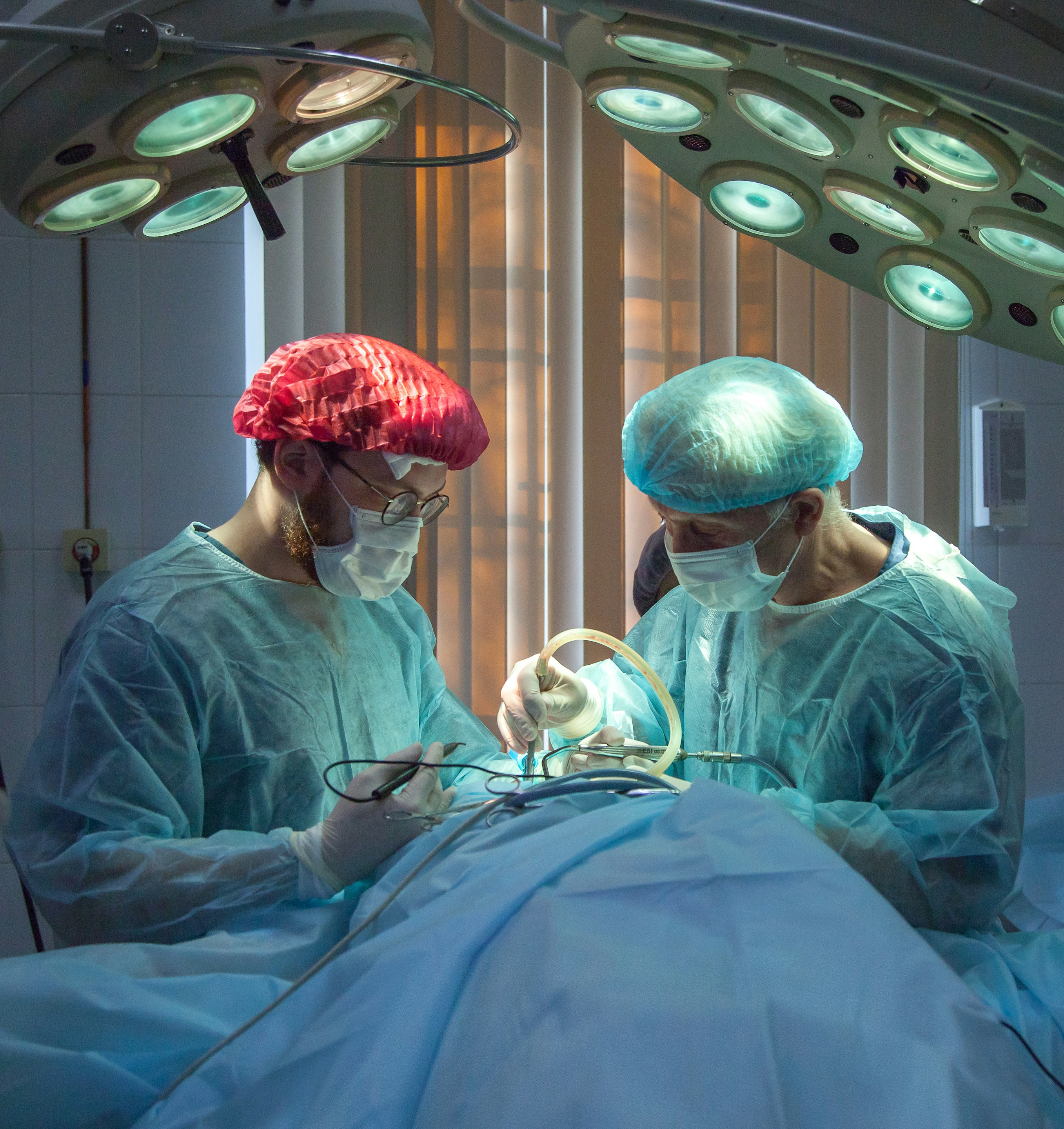
2. Surgery Should Be Seriously Considered If
Conservative treatment has genuinely failed: 6-8 weeks of consistent physiotherapy, medication, and at least one epidural injection have not produced sufficient improvement, and pain remains significantly disabling.
Progressive neurological deficit: Weakness in the leg or foot is getting worse; you're noticing increasing difficulty lifting your foot, walking, or climbing stairs. Worsening motor weakness suggests nerve damage is progressing, and waiting longer increases the risk of permanent deficits.
Foot drop: Inability to lift the front of the foot (dorsiflexion weakness from L4-L5 disc compression) is a motor nerve emergency. Surgery should not be delayed.
3. Immediate Surgery Is Required (Emergency) If
Cauda Equina Syndrome: Loss of bladder or bowel control, difficulty urinating, urinary retention, or faecal incontinence combined with back and leg pain. This is a surgical emergency. A large disc herniation is compressing the cauda equina nerve bundle, and surgery performed within hours to a few days significantly affects long-term outcome. If you or a family member has these symptoms, go to an emergency department immediately. Do not wait for a scheduled appointment.
Common Questions Patients In Noida Ask
1. "My MRI shows a large disc herniation. Does that mean I definitely need surgery?"
Not necessarily. MRI findings alone do not determine surgical need. Many patients with large herniations on MRI recover completely with conservative treatment. The decision for surgery is based on clinical symptoms, neurological examination findings, and response to treatment, not on the MRI report alone.
2."I've had this for 3 months, and I'm not better. Should I just have surgery?"
Three months of symptoms is long enough that surgery should be discussed. But the question is whether you've had three months of adequate, structured conservative treatment, physiotherapy done properly, appropriate medication, and at least one epidural injection. If not, those steps should be tried before surgery. If you've done all of that genuinely and are still significantly disabled, surgery is a reasonable next step.
3." Will the disc herniation come back after it heals?"
The disc that has herniated once is structurally vulnerable. Recurrence risk is real, estimated at 5-15% over five years. This is why post-recovery exercise, particularly core strengthening and ergonomic discipline, is not optional maintenance but active prevention.
4."My doctor in the village said complete bed rest for 6 weeks. Is that right?"
No. Prolonged bed rest is contraindicated for a disc herniation. It worsens muscle deconditioning, maintains disc pressure in lying positions, and delays recovery. Short relative rest during the most acute phase is appropriate; beyond that, guided movement and physiotherapy accelerate healing.
Slip Disc Management In Noida - Dr. Mayank Chauhan At Prakash Hospital
Dr. Mayank Chauhan, Senior Orthopedic Surgeon at Prakash Hospital, Sector 33, Noida, manages slip disc cases from first presentation through full recovery, surgical and non-surgical alike. His approach is explicit: conservative treatment is always tried first. Surgery is recommended only when clinical criteria for it are met, never as a first response to a positive MRI.
For patients currently managing slip disc in Noida with painkillers alone, without physiotherapy or proper evaluation, a consultation will establish exactly where the condition stands and what the best path forward is. To book a consultation with Dr. Mayank Chauhan, call the number listed on the website.
The Bottom Line

Man suffering from lower back pain due to slip disc.
A slipped disc can and very often does heal without surgery. The body's ability to resorb herniated disc material, combined with properly directed physiotherapy and appropriate medication, produces full recovery in 80-90% of patients.
But "healing without surgery" requires active, structured treatment, not passive waiting. And for the patients who genuinely need surgery, particularly those with progressive weakness, foot drop, or bladder involvement, delaying it is harmful.
The key is an accurate diagnosis, a clear treatment plan, and a surgeon who tells you honestly which category you're in. To consult Dr. Mayank Chauhan, Senior Orthopedic Surgeon in Noida, call the number listed on the website.