Arthritis Treatment in Noida: Types, Options and When to See an Orthopedic Surgeon
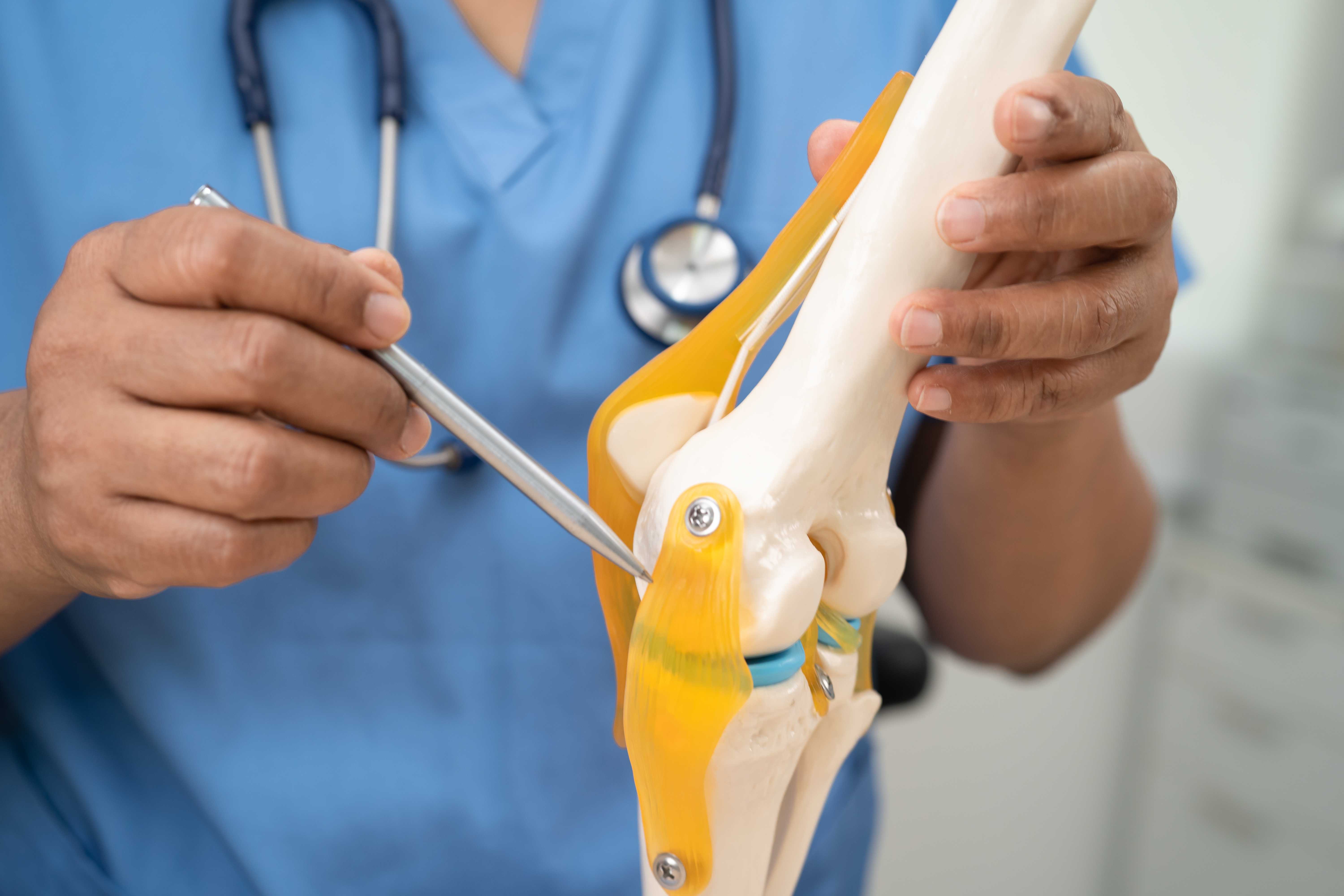
An orthopedic doctor holds a detailed bone model while explaining how bones heal after a fracture during a patient consultation.
Arthritis is one of those words people throw around loosely. Your knee hurts, someone says "oh, it must be arthritis." You wake up with stiff fingers, someone says the same. But arthritis isn't a single disease — it's a family of over 100 conditions, each with its own cause, its own pattern, and its own treatment approach.
Getting that distinction right matters. Because treating rheumatoid arthritis the way you'd treat osteoarthritis doesn't work. Because gout responds to completely different management than psoriatic arthritis. And because the difference between a joint that's been managed well for twenty years and one that needed surgery ten years earlier often comes down to whether the patient got the right diagnosis in the first place.
This guide covers the four types of arthritis most commonly seen by orthopedic surgeons in Noida — what they are, how to recognise them, and what treatment actually involves.
What Is Arthritis, Really?
At its core, arthritis is inflammation in one or more joints. That inflammation causes pain, swelling, stiffness, and — over time — damage to the joint structure. Beyond that, the causes, mechanisms, and affected populations vary significantly.
The joint that bears the most burden in arthritis is almost always the knee. This is because the knee is the largest weight-bearing joint in the body, absorbing forces two to three times your body weight with every step you take. It's also one of the most mechanically complex joints — making it vulnerable to a wide variety of conditions.
The Four Main Types of Arthritis
1. Osteoarthritis (OA) — The Most Common Type
Osteoarthritis is the "wear-and-tear" arthritis. The cartilage that cushions the ends of bones gradually wears down over years and decades, until there's little or no cushioning left and bone begins rubbing directly on bone.
It's the most common form of arthritis in India, affecting millions of people — predominantly those over 50, though it increasingly shows up in younger adults. Obesity, previous joint injuries, repetitive physical work, and genetics all accelerate its development.
What it feels like:
- Pain that's worse after activity and better with rest (in early stages)
- Morning stiffness that eases within 30 minutes
- A grating, creaking sensation in the joint (called crepitus)
- Swelling around the joint that comes and goes
- Reduced range of motion — difficulty climbing stairs, getting up from the floor, or sitting cross-legged
- In advanced stages, a visible deformity — the classic "bowing" or "knock-knee" appearance
OA typically affects joints on one side more than the other, or affects specific joints without a symmetric pattern. The knee, hip, spine, and hands are the most common sites.
Diagnosis:
Physical examination combined with X-rays is usually sufficient to diagnose OA. X-rays show joint space narrowing (as the cartilage thins), bone spurs (osteophytes), and eventually bone-on-bone contact. Blood tests are typically normal in OA — which helps distinguish it from rheumatoid arthritis.
2. Rheumatoid Arthritis (RA) — The Autoimmune Type
Rheumatoid arthritis is fundamentally different from OA. It's an autoimmune disease — the immune system mistakenly attacks the synovium, the thin membrane lining the joints. This causes chronic inflammation that, if untreated, leads to progressive joint damage over time.
RA affects about 0.5–1% of the Indian population, with women being two to three times more likely to develop it than men. It can start at any age — including in young adults.
What it feels like:
- Symmetrical joint involvement — if the right knee hurts, the left knee typically hurts too
- Prolonged morning stiffness — lasting more than an hour (this is a key distinguishing feature from OA, where stiffness resolves within 30 minutes)
- Swollen, tender joints with warmth and redness
- Small joints of the hands and feet are often the first affected
- Fatigue, low-grade fever, and a general sense of feeling unwell — because RA is a systemic disease, not just a joint problem
- Symptoms that flare and subside (rather than being consistently present)
Diagnosis:
Blood tests are central to RA diagnosis — particularly the Rheumatoid Factor (RF) and anti-CCP antibodies. Elevated inflammatory markers (CRP, ESR) support the diagnosis. X-rays show joint erosion in established disease.
RA is primarily managed by a rheumatologist, not an orthopedic surgeon. However, orthopedic intervention becomes relevant when joint damage is severe enough that surgical reconstruction or replacement is needed.
3. Osteoarthritis of the Knee — What Most Patients In Noida Are Actually Dealing With
Worth addressing specifically, because knee osteoarthritis is far and away the most common reason patients in Noida and Greater Noida seek arthritis treatment.
The grading system (Kellgren-Lawrence scale):
- Grade 1: Minimal narrowing, possible osteophytes. Symptoms may be mild or absent.
- Grade 2: Definite osteophytes, some joint space narrowing. Symptoms are noticeable but manageable.
- Grade 3: Multiple osteophytes, significant joint space narrowing. Symptoms significantly affect daily life.
- Grade 4: Large osteophytes, severe joint space narrowing, bone deformity. Significant disability. This is typically when surgery enters the discussion.
The grade matters because treatment at Grade 2 looks very different from treatment at Grade 4.
4. Gout — The Underdiagnosed Type
Gout is caused by the accumulation of uric acid crystals in the joint. When uric acid levels in the blood become too high (due to diet, dehydration, kidney issues, or genetics), crystals deposit in joints — most often the big toe, but also the ankle, knee, or wrist.
A gout attack is typically sudden, severe, and unmistakable — intense pain, swelling, redness, and warmth in a single joint, often waking the patient from sleep. It can be triggered by alcohol consumption, a large protein-rich meal, or dehydration.
Gout is frequently misdiagnosed as a general joint infection or arthritis. The diagnostic clue is the pattern — sudden onset, single joint, very high inflammation — combined with an elevated serum uric acid level and, definitively, joint fluid analysis showing uric acid crystals.
Treatment involves managing the acute attack and long-term uric acid control through medication and dietary modification.
Arthritis Treatment Options in Noida — From Least to Most Invasive
Treatment is always tailored to the type and severity of arthritis, the patient's age and activity level, and how much quality of life is being affected. A good orthopedic specialist doesn't jump to surgery. The approach is staged.
Stage 1: Lifestyle Modification and Conservative Management
For mild-to-moderate osteoarthritis, these measures can be genuinely effective and should always be tried first.
Weight management: For every kilogram of body weight lost, the load on the knee reduces by approximately 4 kilograms. Even modest weight loss produces meaningful pain relief in knee OA.
Exercise: Low-impact activities — swimming, cycling, walking — strengthen the muscles around the knee without adding damaging stress to the joint. Strong quadriceps and hamstrings function as shock absorbers, protecting the knee from impact. Patients are often afraid to exercise because of pain, but the right exercise, done correctly, helps rather than harms.

A man riding a bicycle on an open road, promoting cycling as a low-impact exercise that improves joint mobility, posture and overall physical fitness.
Heat and cold therapy: Ice packs reduce acute swelling. Heat (warm soaks, heating pads) eases stiffness. Neither is curative, but both provide useful symptomatic relief.
Assistive devices: A walking stick, knee brace (particularly an "unloader brace" that shifts weight away from the damaged compartment), and proper footwear all reduce joint stress.
Activity modification: Avoiding high-impact activities (running, jumping), reducing stair use, using a raised toilet seat — these small adjustments collectively reduce the load on a damaged knee.
Stage 2: Medications
Over-the-counter pain relief: Paracetamol and topical NSAIDs (like diclofenac gel) are first-line medications for mild arthritis pain.
Oral NSAIDs: Ibuprofen, naproxen, and etoricoxib reduce inflammation and pain. They're effective but should be used for the shortest possible duration due to stomach and cardiovascular concerns with long-term use.
Glucosamine and chondroitin: Supplements with a mixed evidence base — some patients find benefit, studies are inconsistent. They're safe, and some patients use them long-term with positive subjective results.
For RA: Disease-modifying anti-rheumatic drugs (DMARDs) — methotrexate being the most common — are the cornerstone of RA management. Biologics are used in patients who don't respond to first-line DMARDs.
Stage 3: Injections
Corticosteroid injections: A steroid injected directly into the joint provides fast and significant relief — typically for 3 to 6 months. Can be repeated, but frequency is limited (typically no more than 3–4 per year in the same joint).
Hyaluronic acid (viscosupplementation): A synthetic version of the natural joint fluid is injected into the knee. Acts as a lubricant and shock absorber. Particularly useful for elderly patients who want to delay surgery. Effects last 6–12 months.
PRP (Platelet-Rich Plasma): The patient's own blood is processed to concentrate growth factors, and this is injected into the joint. There's growing clinical evidence that PRP can reduce pain and slow cartilage breakdown in early-to-moderate OA. It's not covered by all insurance plans, but demand in Delhi NCR has grown significantly.
Stage 4: Surgery
Surgery is considered when:
- Non-surgical treatments have been tried adequately and failed
- Pain significantly impacts daily life, sleep, and independence
- X-rays show Grade 3–4 osteoarthritis (significant or bone-on-bone)
Arthroscopic surgery: Useful in select patients — particularly younger patients with associated meniscus tears or loose bodies in the joint alongside early OA. Not curative for advanced arthritis.
High Tibial Osteotomy (HTO): A surgical procedure where the tibia is cut and realigned to shift load away from the damaged compartment. Appropriate for younger, more active patients with OA confined to the medial compartment and good overall joint health.
Partial Knee Replacement: When only one compartment of the knee is arthritic, replacing just that compartment preserves more healthy tissue and offers faster recovery than total replacement.
Total Knee Replacement: The gold standard for end-stage knee OA. Extremely well-studied, with consistently high success rates. Modern implants last 15–25 years. Patients typically experience dramatic pain relief and return to most daily activities.

Orthopedic doctor performing knee replacement surgery.
Arthritis Treatment in Noida — Getting the Right Diagnosis First
One of the most common issues patients face in Noida is getting general back pain or knee pain treatment without a proper diagnosis of what type of arthritis — or what stage — they're actually dealing with. This leads to months of ineffective treatment and sometimes unnecessarily delayed surgical intervention.
Dr. Mayank Chauhan, Senior Orthopedic Surgeon at Prakash Hospital, Sector 33, Noida, approaches every arthritis patient with a thorough evaluation — physical examination, appropriate imaging (X-ray and/or MRI), and blood tests where indicated. The treatment plan is built around the specific patient: their age, activity level, the type of arthritis, its severity, and their personal goals for recovery and function.
Patients from Noida, Greater Noida, and across Delhi NCR consult Dr. Chauhan for both non-surgical arthritis management and surgical treatment, including knee replacement.
To book a consultation, call the number listed on the website.
When Should You See an Orthopedic Surgeon for Arthritis?
Not all arthritis needs to go straight to an orthopedic surgeon. But these signs suggest it's time:
- Knee or hip pain that has persisted for more than 6–8 weeks despite basic treatment
- Pain that is affecting your sleep, your ability to walk, or your daily independence
- Swelling that keeps coming back
- A grating or grinding sensation in the joint
- Visible joint deformity or alignment changes
- A previous X-ray showing significant joint space narrowing
- Leg pain accompanying back pain (possible slip disc — another orthopedic issue)
- Pain that's significantly worse on one side compared to the other
Early consultation leads to early intervention. Early intervention preserves more joint tissue and keeps more options open.
The Bottom Line
Arthritis doesn't have to mean a life of pain or a premature surrender of independence. With the right diagnosis and a structured treatment plan, most patients — whether they're dealing with early osteoarthritis or advanced joint degeneration — can achieve meaningful improvement.
The best outcomes come from catching it early, treating it properly, and not waiting until the joint is completely destroyed before seeking help.
If you're in Noida or Greater Noida and dealing with persistent joint pain, stiffness, or swelling, book a proper evaluation.
To consult Dr. Mayank Chauhan, Senior Orthopedic Surgeon in Noida, call the number listed on the website.